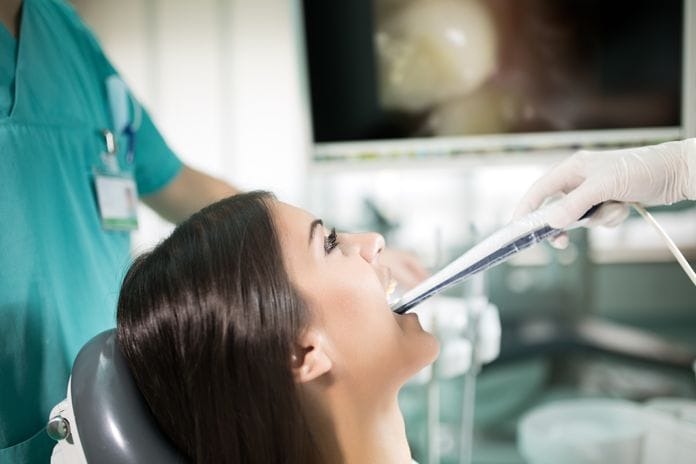
At the beginning of my dental hygiene career, I was fortunate to have an intraoral (IO) camera, at least I was told this by the dentist. I was excited because I was told I should be…but I hated that camera! It was heavy and hard to maneuver; that was 1996. In 2006, I was exposed to a lightweight Schick IO camera. It was at this time I truly fell in love with using an IO camera, and I have not looked back since.
How did this metamorphosis happen?
The dentist I began working for in 2006 took time to guide me on what to look for when using an IO camera and how to properly capture the image. He also advised me on how to case present using appropriate verbiage. Once my confidence was built, it was like riding a bike – super easy. I have heard hygienists complain they don’t have enough time in their appointments to use their camera; I disagree! Knowing what to look for, how to capture the image, and present to patients comes naturally after practice. Hygienists are short-cutting patients, and themselves, when the camera sits around collecting dust. Putting the camera to work increases case acceptance, thus allowing the dental practice to increase their bottom line, while promoting optimum care for patients.
Why should you fall in love with an IO camera?
It shouldn’t be because you were told you should love this piece of technology, it should be because you cannot live without it! Would we want to do a prophy without the option to use an ultrasonic? Along the same lines, we should not want to discuss anything happening inside our patients’ mouths without being able to tell the story of what is happening. Let’s be honest, that hand mirror on your countertop, the one with splatters all over it, yep that one, is not an adequate tool to “show” patients anything inside the deep, dark cavern of a mouth. You cannot see anything with a hand mirror compared to what you can show a patient with an IO camera.
Let’s evaluate a photograph with an IO camera together.
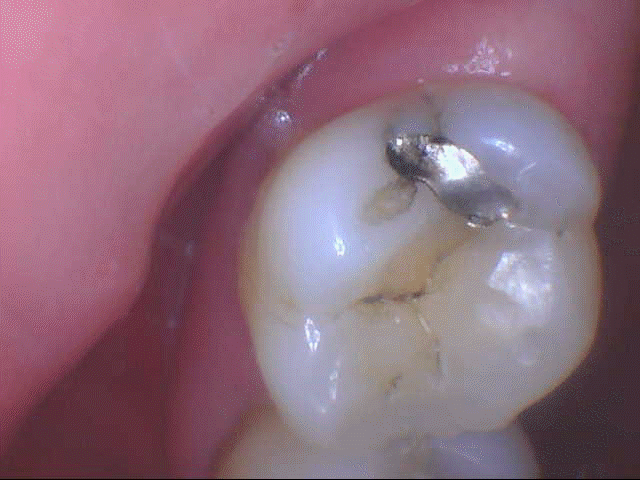
Image 1 above clearly shows minor breakdown of the amalgam on this tooth, a couple of cracks on the amalgam, and a crack on the distal aspect. Without the lighting and accessibility that comes with IO technology, we would not be able to “clearly” see the leakage that is occurring. Also, we can maneuver the image to shed light on any other potential problems (cracks, decay, chipped areas, occlusal issues) that can be observed while using this tool.
I like to use the terminology, tool, because I have often heard patients state, “Oh, the doctor got another new toy!” No, the doctor did not get a toy! Toys are for kids, who are good at the dental office; you can find those in a basket at the front desk. When I hear this, I explain, “This intraoral camera is not a new toy, we are now utilizing this amazing tool to show you better what is going on in your mouth. We have found it is no longer adequate to use an old hand mirror. As we both know, you cannot adequately see inside your mouth to truly value why we are making this diagnosis today.” When we idealize our tools as such, the level of respect for our diagnoses will increase, and the value that the IO camera brings to your hygiene appointment will become immense.
When do you expect me to use a camera?
As you read earlier, I have been practicing for quite some time, yet it took me many years to appreciate the value the IO camera brought to hygiene appointments. Until my most recent employment experience, I had not done it this way, but I can tell you that “old dogs can learn new tricks.” At new patient appointments, patients take part in having intraoral and extraoral images. I will only touch on IO images at this time and explain the best use of the camera.
Begin by drying off the entire upper arch and take images of every tooth in that arch, and then repeat for the lower arch. Captured images usually include the occlusal surfaces on bicuspid and molar teeth and usually lingual surfaces of anterior teeth. Although I use my judgment to capture additional areas that may be important for patients to view. When I previously heard in a CE class to take a picture of all teeth, I thought, they are out of their mind. Now, I have experience doing this and feel it’s crazy not to take images of all teeth.
Why do I feel this way?
The saying, “a picture says a thousand words” cannot be truer than when we use IO camera technology in dentistry. For those of you using your cameras, you have heard patients comment on how gross something looks or how they become more concerned when they see a crack on their tooth with that “ugly, silver filling.” Do you think that a patient would be able to say those words looking into a hand mirror? We all know the answer to this question.
I find having initial photos allows you the ability to go back to the very first time you saw your patients’ gingiva and teeth. If you have a patient with periodontal disease or gingivitis, you can reflect back to show them when there are improvements. We all love the amount of calculus that can be found on the lingual of the lower anteriors and removing it, right? What better feeling than to show your patients before and after photos of this transformation. They truly believe you are a magician when they see this. However, with this, I have also noticed many patients taking accountability and not “allowing it to get like that again.”
Another important time to use the camera would be for documentation of abnormalities when performing head and neck exams. It is much easier to capture the image of a suspicious area, so you can compare the area from visit to visit. It also emphasizes to the patient the importance of returning for recare visits to have a suspicious area evaluated routinely. It’s time to get your dusty cameras off the shelf, put them, and your level of expertise, to work for the health of patients and the productivity of your practice.
What camera is best?
This article is not designed to promote one camera versus another, rather to simply encourage dental staff to use one of the most underutilized tools in the office. Back to my good old days, you will recall, I said I hated the first camera I used. Why? It was bulky, heavy, and hard to use. The best camera for you is one you will use.
At my current job, I started out using a camera that had a special focusing device. I hated it because it was hard to capture a quality image. At one of our staff meetings, I made it known that I appreciated the value the camera brings to co-diagnosis. However, I was not doing co-diagnosing any justice with the current camera. Our doctor had spent a lot of money on IO cameras in the past, but once he bought a lightweight, easier to use maneuver IO camera, I pulled it out as much as I could to educate patients. What a value this became to our practice when we were better able to display and discuss our findings in our dental exams.
Again, when can you find time to use this camera you oh so love? Be sure you have the camera installed in a very accessible area; an area which will not deter you from grabbing it the minute you see something “suspicious” the patient or doctor should see. Pick it up anytime throughout the appointment because you can and should. Ultimately, it will save you time explaining what you are seeing. After I capture an image, I continue treatment. I find this to be when patients think about that “ugly” image they just viewed. More questions may arise, and while you work, you are able to educate further; this saves time as well.
At the end of treatment, once you have captured the images you need, sit your patient up, advise them of your concerns, and explain what you believe the doctor will discuss in his/her exam. Now for the slam dunk, when your doctor arrives for the exam, you can display the area(s) of concern. At the same time explaining you have informed Mr. Smith of these areas, and you have advised him you will likely be recommending treatment x, y, z for these areas. Did I say slam dunk? Yes, I did! By having these images available, you have reduced time in attempting to look into the dark cavern of a mouth, have clearly shown the patient your concerns, and have given a visual clue to your dentist on areas to evaluate. This will allow them to pre-diagnose before the clinical exam, which also reduces time.
How does this affect our bottom line?
Use of the IO camera allows clinicians to have a correlated image to what is actually going on within the mouth. This tool will increase your bottom line with diagnosis, but moreover, assists your insurance coordinator with submitting the proper documentation the first time with claims. I have heard in many CE classes that insurance claims with photos are processed before those without. Practices who follow this easy guideline will usually save time because they do not have to re-process claims. These offices are likely getting reimbursements more quickly, as well.
I would be willing to bet we all want to give our patients the best care; it is in our nature as healthcare providers. Utilizing the IO camera should become second nature in delivering optimum patient care. Without the use of an IO camera, we not only shortchange patients but we also shortchange ourselves in the treatment we provide. Having an intra-oral photo can save time, even though many think it will not. This occurs mostly because “a picture says a thousand words;” words we do not have to use to educate patients on their needs. It is time to dust off your IO camera and put it to work!
SEE ALSO: Why You’re Missing Out if You Aren’t Using an Intraoral Camera
DON’T MISS: The Many Lives of the Mysterious Full Mouth Debridement