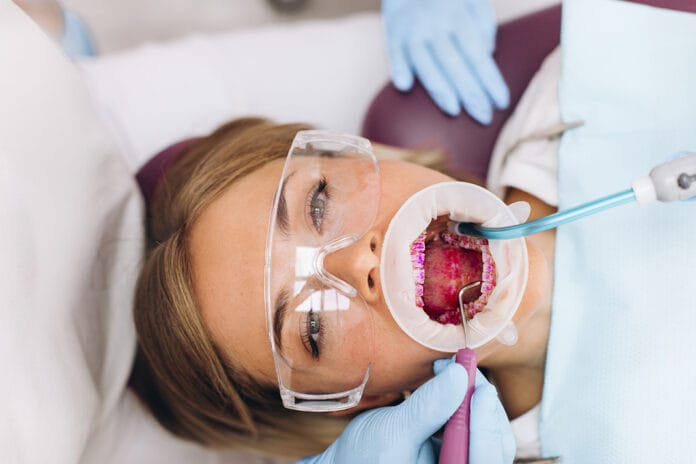
The work environments of dental hygienists are not all the same; some are private practices, while some are group practices (DSO) or public clinics. Dental hygienists also treat patients in different ways, depending on allowable duties and/or equipment available in the office ‒ all according to the individual patient’s needs.
Many dental providers understand the “traditional” way of dental hygiene and what they learned in their hygiene program. New technology and treatment modalities arise, though, leading to changes in the way we treat patients in our field. One newer modality is called guided biofilm therapy (GBT).
I reached out to Sarah Crow, RDH, from Massachusetts, to learn more about GBT. She has been using this type of therapy for two years. Sarah reports she has been in the dental world for almost 20 years with orthodontics experience and then became a dental hygienist in 2014. Today, she works in a private practice that uses GBT daily. Sarah describes GBT as a “completely different” way through a dental hygiene appointment.
Machado: What made you decide to become a dental hygienist? What is your why?
Crow: Since I was 18 years old, I always knew I wanted to be a dental hygienist. I felt as though it would be a professional and rewarding career. What I didn’t realize was that my late grandmother was also a dental hygienist in her day. She was in one of the first graduating classes of the Forsyth School for Dental Hygienists back in 1927! I was, of course, shocked to learn this information about my grandmother and knew at that moment that this was meant to be, and dental hygiene was in my blood.
Machado: So, what actually is GBT?
Crow: GBT stands for guided biofilm therapy. It is, in my opinion, a high-level dental hygiene experience for patients that provides an ergonomic solution for the clinician. This involves a stand-alone unit that can be placed on a table or countertop or installed as a portable unit that can be used in multiple operatories.
Machado: Are you aware of the history of GBT? Is your office the only office around you using GBT?
Crow: GBT has been around for many years in Europe and originated in Switzerland. There are very few offices in my area of Massachusetts using the GBT system; however, the trend is moving quickly.
Machado: How was your first interaction with GBT?
Crow: My first interaction with GBT was an in-office training provided by the number one trainer in North America at the time. She provided us with a full day of in-office training, including didactic and clinical implementation.
I have to say, as much as I love learning new things, this was a packed day. Learning what to say to the patient and how to say it was probably the most important part. The hands-on skills would come with time. I knew that. What I was more concerned about was how I was going to get my patients to be just as excited about this new technology as I was!
Machado: Are there any additional training or certifications for GBT?
Crow: Yes, GBT has multiple online and in-person training you’ll need to use this system.
Machado: What are the requirements for GBT? What do you need to perform GBT? Describe the process.
Crow: GBT provides a comprehensive removal of the oral biofilm while also applying a natural antimicrobial used as a medicament that has the capability to go up to four millimeters subgingival.
The process includes, first and foremost, a conversation with the patient. Getting your patient excited about what’s coming next is the “gem” of the dental hygiene appointment.
I usually say something like, “OK, you’re going to love this! Today’s dental hygiene appointment will be a little different from what you’re used to. I’m going to use an air, water, and powder spray. The powder is a natural antimicrobial that will remove the bacteria from your mouth and provide a medicament that can go under the gums and treat the hard-to-reach areas. It’s fast, effective, and very comfortable. It is a little messy, though. It kind of feels like a car wash going off in your mouth!”
They usually have a little chuckle and reiterate that they love the fact that it’s fast.
Sometimes they’ve experienced a prophy jet in the past and think that’s what they are getting. If they mention anything of the sort, I explain that this is much different and is a newer technology in the United States.
Then I proceed to place a lip and cheek retractor for isolation. I then hand them the patient mirror, and they chuckle again at the look of themselves wearing the retractor. I then ask them to look at their teeth and see if they can see any bacteria.
I’ll say, “Can you see your teeth? Look closely and tell me if you can see any bacteria. It’s almost impossible to see, so I’m going to use this disclosing gel which I will be using as a guide but is a great learning tool as well.”
I proceed to paint on my favorite disclosing solution. This will allow me to discern, based on color, between bacteria that have been in the mouth for more than 48 hours and will also let me know if there are aciduric bacteria present. I will point out this cavity-causing bacteria to the patient. I quickly explain the difference between hard bacteria and soft bacteria and what we call them.
I’ll take a piece of floss and show the technique as they watch with a patient hand mirror the purple-stained plaque vanish from the interproximal spaces. I like to mention how dangerous this biofilm is and how it can enter into the bloodstream via their bleeding gums and cause issues in other parts of their bodies. I’ll often correlate the amount of plaque in particular areas of their mouth with their perio charting. Explaining that this is the reason their gums are bleeding and how it needs to be removed daily.
I will also remind them that this is why I took their blood pressure at the beginning of the appointment. Verbally connecting all parts of the appointment to the patient helps take them through the appointment journey.
Once oral hygiene instruction is completed, I will start up my favorite aerosol and water controlling device. This compact device is superior to any suction and aerosol device I’ve ever used. When used in conjunction with the retractor, the patient is so comfortable that I often feel like I’m working on a typodont with incredible direct vision and access.
I start with the device’s air handpiece and begin to debride the disclosed biofilm. The handpiece is pointed towards the gingiva allowing the erythritol-based powder to access the subgingival spaces. Once I’ve removed the biofilm, I will use utilize the device’s unique ultrasonic handpiece to remove any present calculus that wasn’t removed by the air handpiece.
Once complete, I may check contacts with hand instruments, oftentimes to find nothing left behind. I proceed to place varnish, then remove the retractor and sit the patient up. Usually, if it’s their first time, they’ll say something like, “Wow, that was so comfortable, and like nothing I’ve ever experienced before. I think I fell asleep!”
Machado: Can you do nonsurgical therapy/SRP with GBT?
Crow: Yes, absolutely. The perio handpiece on the unit is specifically designed to reach up to 10 mm subgingivally and allows erythritol to be delivered deep into the periodontal pockets.
Machado: How long is this GBT process?
Crow: The process is about 20 minutes, depending on the patient. Each appointment time is one hour. The actual prophylaxis takes approximately twenty minutes, depending on the patient.
Machado: With GBT, does this change recommendations or further treatment or recall?
Crow: I will recall each patient based on their specific needs. Mostly three or four months.
Machado: Are there any contraindications for GBT?
Crow: Like any air-polishing device, patients suffering from respiratory tract infection, chronic bronchitis, or asthma must not, under any circumstances, be treated with an air polishing device. The jet of air and powder could cause respiratory difficulties.
Predisposed persons may be sensitive to cetylpyridinium chloride (CPC). If allergic reactions are observed, stop using the product and completely remove the powder from the mouth. It is easy to remove any erythritol powder from the patient’s mouth since the teeth are easily visible due to the use of a retractor, and high-speed evacuation is being utilized. The clinician would simply rinse the patient’s mouth with water from their air-water syringe.
Machado: Are there any differences in infection control or precautions?
Crow: There are a lot of pieces to the specialized unit device. This requires a little extra time spent in the sterilization area. The unique ultrasonic handpiece breaks down into five pieces before it’s bagged and placed into the autoclave. The air handpiece must be flushed with a syringe of water after each use, wiped, and bagged as well.
Wiping down the machine in between patients is quick and easy. Running line cleaner through these lines is done nightly. The device makes this easy with a quick touch of the foot pedal when both handpieces are lifted from the device. The ultrasonic water supply comes from the enclosed bottle of distilled water.
Machado: What do your patients think about GBT? What are their reactions?
Crow: I have patients leaving their periodontists to come to our practice because of this technology. I have also had new patients that have Google searched dental offices in the area using this technology and came to us for just that.
I always believe it’s important to work closely with a periodontist if a patient doesn’t respond to periodontal therapy regardless of what system one is using to provide care.
Machado: Can you think of a patient case that stands out to you involving GBT?
Crow: Yes, an implant patient. I knew I was delivering a stellar dental hygiene visit that was so much more beneficial than the standard scaling and polishing of the past. Think about your implant patients. Oftentimes, clinicians struggle to access implants to properly debride them or, even worse, are afraid to cause long-term damage. The erythritol powder is effective on implants because it cannot damage them and does more than just remove the biofilm. It provides that natural antimicrobial at the very same time. I like to use the perio handpiece to access all-on-four cases allowing full access to the implant and the thorough removal of dangerous biofilm.
In Closing
The dental profession is so large, involving many specialties, technologies, and patient care processes. The growth continues to expand every day to benefit patients’ oral health. Dental hygienists must continue to learn and evolve as well.
GBT is a great example of new innovation for dental hygiene intervention. Sarah reports that “using GBT every day has reignited my love for dental hygiene clinical practice, and I can’t wait to share it with the rest of the dental hygiene world!”