The scary “C” word, cancer, could naturally cause a clouded judgment to anyone affected by it. You have a hard time seeing the light at the tunnel and question everything leading up to the diagnosis.
“Why me?” “Am I going to die?” “No, are you sure?” These are all thoughts that could run through a worried mind. At least it did for my mother.
The intraoral and extraoral soft tissue examination (IO/EO) is a vital part of a clinical exam. You may vaguely remember writing down every detail of your patient in dental hygiene school so you could pass this portion during check-off.
I was in the middle of my first year of spring clinicals at Western Kentucky University when I had the honor of doing a prophy on my mother. I thought, “Easy morning, easy check-off.” I went over her medical history, and as far she knew, she was healthy with no medical issues. Then, we proceeded to normal protocols. At the end of her appointment, the dentist (Dr. Terry Dean) came in for the final check-off. He pointed out some oral findings that I did not notice, such as enamel hypoplasia on her lower centrals and some other minor findings.
As a first-year student, I was still learning quite a bit but still felt discouraged I did not notice some findings. However, when he examined my mother’s neck, he asked her if she had any trouble swallowing. She chuckled and asked, “Well, isn’t it normal to choke on your food or beverages a time or two?” He calmly explained how crucial it is to see her physician in regard to her thyroid. Now, I’m thinking, how did I miss that?! What did I not feel?!
A Complete Exam
A complete examination covers the following three areas:1
- The general examination briefly assesses the patient’s overall appearance.
- The extraoral head and neck soft tissue examination focuses on the head and neck.
- The intraoral soft tissue examination determines if the soft tissue is within normal limits.
From the time our patient comes back into the operatory or even the building, we are observing them. Their general appearance, gait, symmetry, and mobility gives us clues about their health.1 Take note of any findings of scars, lesions, or facial asymmetries.
When we review their medical history, it is more than updating medications. I personally think some patients think this is all we want to know. “No changes pertaining to my dental health” is a common response. I have to get really specific with what I want to know.
Unfortunately, some patients may not see a physician on a regular basis. It is our job to note and explain any concerns. For example, taking blood pressure is extremely important because you could prevent a possible heart attack or stroke.
Extraoral Head and Neck Examination
Dr. Karen Burgess of the University of Toronto offers insights into this exam here. Here are some of the key points that she raises.
Asymmetries − Have the patient sit in the dental chair or to the side of the chair and stand directly in front of them and note significant asymmetries. Examples include scars from previous surgeries, nerve paralysis from CVA/stroke, tumors, and infections. Note the size and location.1
Lymph node examination − Dr. Burgess explains, “These are in the head and neck area and should be palpated gently to observe for tenderness or enlargements. Normal lymph nodes are either not palpable, or you may feel a lymph node that is the size and shape of a small pea or lentil. These are also mobile and non-tender.”1
If there is tenderness, this indicates inflammation or drainage of infection. When you are palpating with the flat of your fingertips, use an on and off motion walking your fingers along the preauricular, postauricular, suboccipital, submandibular, submental, cervical, and supraclavicular lymph nodes.1
TMJ examination − Place fingers over TMJs and ask patient to open and close their mouth, slide jaw to the right/left, and note any pain, tenderness, clicking, popping, crepitus, deviations, or limited opening.1
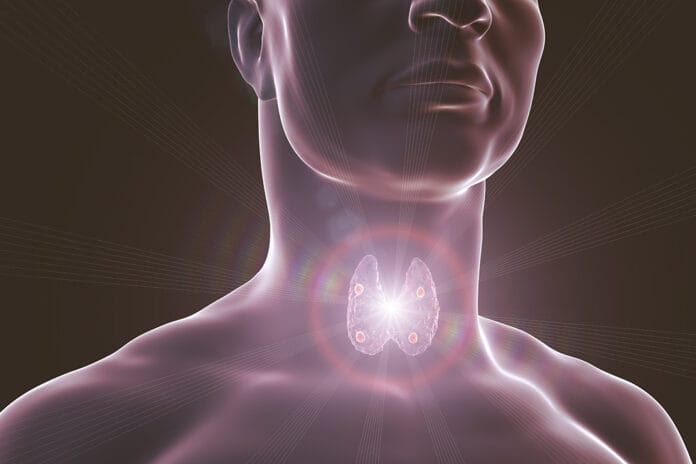
Thyroid gland − In a CE course, Nancy Burkhart and Leslie DeLong describe this as “found inferior to the larynx and just superior to the clavicles on either side of the trachea. It consists of two lobes connected by an isthmus. Palpate the gland using a bimanual technique where one hand supports the tissue, and the other hand palpates the gland on one side, and the reverse is done to examine the opposite side of the gland. The normal thyroid gland should not be visible and is most often not palpable. In addition, the area surrounding the gland should elevate smoothly and symmetrically during swallowing.”2
Intraoral Soft Tissue Examination
Knowing your anatomy and different variations of normal are crucial when checking to see if your patient has any abnormalities. If there is an abnormality, note if it is a macule, ulcer, polyp, etc. The size (measured with a periodontal probe), color, location, texture, and consistency are necessary to note. Remember, you need to check the following areas:1
- Lips and labial mucosa
- Buccal mucosa and vestibular mucosa
- Hard and soft palate
- Oropharynx and fauces
- Tongue
- Floor of the mouth
- Gingiva and alveolar mucosa
Personal Case History
My mother decided to take the advice from Dr. Dean to see her physician. They ordered an ultrasound, and it showed a one-centimeter nodule. She was then referred to an endocrinologist where they performed a fine needle aspiration. If you are unfamiliar with this type of biopsy, this is when the patient lays on their back, the neck is arched, and the specialist numbs the facial area.
An ultrasound is performed for visual, and the needle aspirates the tissue of concern. It feels like someone is moving a straw around the inside of your throat. They place a bandage over the area, and you go about your day as normal. My mother then awaited results, and it came back as papillary carcinoma.
I was in the middle of my local anesthesia course when she informed me of this terrible news. My heart sank, and my stomach was in knots. How could this be? At age 49, how does my mother just now find out that her thyroid is extremely unhealthy?
We partnered up during the lab/clinical portion of the course the next day, and I decided to be the patient first. My poor clinic partner witnessed me having the worst anxiety attack. My instructors spoke with me privately, asking what was going on. I told them if Dr. Dean did not advise my mom to seek medical attention, who knows how long this cancer would have remained and spread to other organs!
An appointment was then made with an ear, nose, and throat surgeon. The options were discussed, and a total thyroidectomy was decided to be the best treatment with possible radiation treatment. The surgery took three to four hours and was successful. The surgeon explained that instead of her thyroid gland looking like a butterfly, it was so encapsulated with her throat that to make sure all thyroid tissue was removed (see Figure 1).
Radiation treatment was necessary. If any thyroid tissue remained, then it risked cancer remaining and growing. She was in the hospital overnight and had a Jackson Pratt Drain. I stayed with her the entire night and witnessed a very gruesome 12 hours.

When she was released, she was instructed to limit turning her head from side to side. Unfortunately, she developed an extremely stiff neck and had a lot of muscle spasms (see Figure 2). She slept propped up for a week. Follow-up with the endocrinologist was next with radiation treatments.
Her TSH (thyroid-stimulating hormone) had to be above 30 (high) in order to receive the radioactive iodine in the form of I-131. For those who are unfamiliar with this, radioactive iodine “is a therapy used in the treatment of some thyroid cancers, specifically papillary and follicular thyroid cancer. For the thyroid gland to make thyroid hormone, the first step in the process is for the thyroid cells to ‘take up’ iodide from the bloodstream. Iodide is one of the building blocks used to produce thyroid hormone. By making the iodine radioactive (in the form of (I-131), it becomes toxic to cells that accumulate iodine from the bloodstream, in turn killing these cells.”3
I-131 is a pill, and you have to prepare for this. My mother had to follow a low iodine diet for two weeks. By doing this, it causes thyroid hormones to absorb the I-131. She waited for three weeks and eventually had to receive Thyrogen shots to boost her TSH. This boost made her feel absolutely terrible and extreme fatigue.
My mother had a high dosage of the I-131 pill, and, during this first week, she could not be around young children, had to use a private toilet, no sharing of utensils or glassware, and social-distancing from her husband. One week after this, she had a full-body scan. Unfortunately, she had to repeat the process of the pill but a smaller dosage.
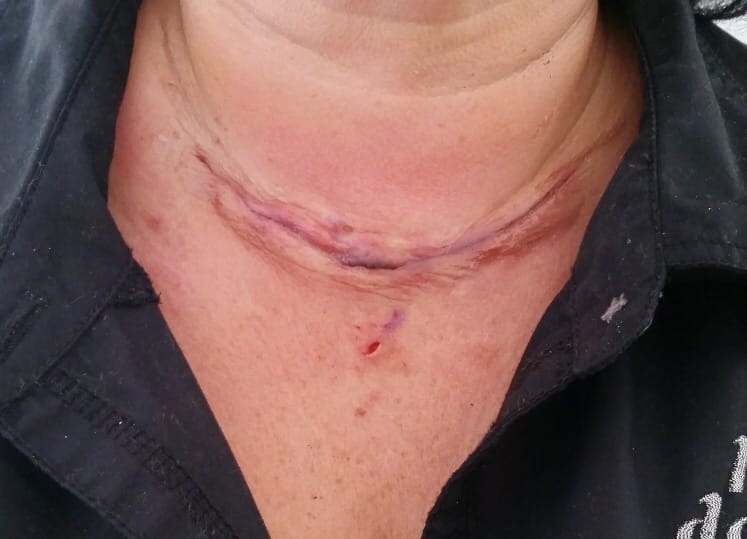
Fast forward to the present time (more than six years later), my mother has to take Synthroid medication for life, multiple ultrasounds to evaluate growths, and regular doctor visits with her endocrinologist (see Figure 3). She has come to terms with the long-life commitment to this new lifestyle and is thriving. She is forever thankful for my dental hygiene program and especially Dr. Dean.

Now sit back and reflect. We see our patients pretty regularly and at least hope to develop trust and comfort with them. The relationship with them develops an understanding of the importance of oral health. Are you evaluating their extraoral and intraoral anatomy thoroughly?
Personally, I think if we make a habit of incorporating this system with every patient at every appointment, greater respect and thankfulness will shine through our patients. Practice makes perfect.
I understand there are days where we run behind and might consider skipping this step but don’t you believe your patients’ deserve this extra time and thoroughness? The more we perform this examination, the faster we will be able to detect any abnormalities. Hygienists do more than clean teeth; we can change and even save someone’s life.
Before you leave, check out the Today’s RDH self-study CE courses. All courses are peer-reviewed and non-sponsored to focus solely on pure education. Click here now.
Listen to the Today’s RDH Dental Hygiene Podcast Below:
References
- Burgess, K. (n.d.). Extraoral And Intraoral Soft Tissue Examination. University of Toronto Faculty of Dentistry. Retrieved from https://iits.dentistry.utoronto.ca/extraoral-and-intraoral-soft-tissue-examination.
- Burkhart, N.W., DeLong, L. (2019, January 31). The Intraoral and Extraoral Exam. Retrieved from https://www.dentalcare.com/en-us/professional-education/ce-courses/ce337.
- Kim, C., Mandel, S. (2020, October 19). Radioactive iodine (I-131) Therapy for Thyroid Cancer. OncoLink Team. Retrieved from https://www.oncolink.org/cancers/thyroid/treatments/radioactive-iodine-i-131-therapy-for-thyroid-cancer.