Several of my female patients have recently presented with the same pathological condition of lichen planus. They were treated in the same way with a topical corticosteroid cream, triamcinolone, that was applied to the affected areas in the buccal mucosa, gingival tissues, and/or tongue two to three times a day.
The dental patients’ questions about the immune system deficiency triggered my interest in doing more research into the condition. Although I remembered learning about the lichen planus in hygiene school, during the rush to remember so many different cases in pathology class, some details had begun to slip my mind.
During the research of this autoimmune disease, I gathered that lichen planus can affect more than just the oral mucosa and can present in the esophageal mucosa, larynx, and conjunctivae, or mucous membrane of the eyes. This disorder can also appear in other places of the body, such as the skin of the wrists, legs, trunk, genital region, scalp, and nail tissues. Though these areas are the most common, this condition can appear anywhere on the body.1
Etiology of Lichen Planus
Lichen planus appears to present due to a T cell-mediated reaction that causes negative effects against the basal epithelial keratinocytes, but the true cause is unknown. It appears most in people with a genetic predisposition, but other related conditions linked to lichen planus include those associated with liver dysfunction, such as hepatitis B or C.2
Clinical Appearance of Lichen Planus
Most dental professionals are aware that the normal emergence of lichen planus presents as the typical white, lacy appearance of the buccal mucosa, also known as Wickham’s striae (see Image 1). However, other lesions that appear can be described as purple in color and “flat-topped papules and plaques.” The plaques can also be labeled as pruritic or itchy to the patient. Some lesions in the acute phase of the disease can follow the Koebner phenomenon, meaning that new lesions may appear at the site of a skin injury such as a cut or scrape.3
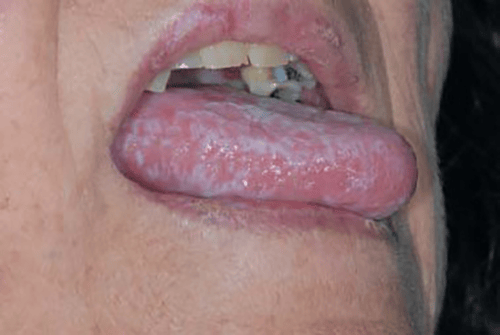
(CC BY 3.0 via Wikimedia Commons)
Papules are sometimes known to coalesce or come together to form one larger lesion. The papules may also become darker in color, atrophic (degenerative), hyperkeratotic (thickened), or appear as vesicles or blisters. In oral cases, a yeast infection can accompany lichen planus. When affecting the scalp, alopecia can occur.3 Erosive lichen planus, a variant of the condition, can also present and results in areas, generally in the oral or genital regions, of ulcerated lesions that result from autoimmune damage to the basal cell layer of the mucosa.4,5
The most common time for lichen planus to appear is between the ages of 30 and 70, and the condition does not favor a gender with no noted racial predisposition.
Links, Triggers of Lichen Planus
A genetic predisposition is often associated with this condition, but other conditions have also been linked to lichen planus. Helicobacter pylori (H. Pylori), which is associated with peptic ulcer disease, has also been shown to be statistically significant in the link to lichen planus. Viral and bacterial infections, vaccinations, and even dental restorative materials have also shown links to causing lichen planus.3
Some triggers that can cause lichen planus flare-ups include receiving the hepatitis C vaccination and interactions with gold, arsenic, iodides, chloroquine, quinacrine, quinidine, antimony, phenothiazines, and diuretics. Stress can also provoke a lichen planus episode.
Oral Care of Lichen Planus
When treating oral cases of this condition, it is very important for the patient to practice meticulous oral hygiene and prohibit the use of tobacco products. Beyond triamcinolone, steroid injections and mouth rinses that have calcineurin-inhibiting properties, such as cyclosporin or tacrolimus, are also used. In cases where itching on the skin is present, antihistamines may be prescribed. In severe cases that are not limited to just oral mucosa, photochemotherapy light treatment, retinoid drugs, and cyclosporine or hydroxychloroquine can be used.3
It is important to note that lichen planus in severe or erosive states can increase a patient’s risk of developing oral cancer, especially when the use of tobacco and/or alcohol accompanies the condition. Though noted previously that lichen planus does not favor a gender, it is also vital to note that the female gender is a risk factor of a higher incidence of malignancy in lichen planus lesions. Research evaluating the incidence of malignancy, erosive lichen planus and tongue lesions were also noted to be clinically evident risk factors.5
As oral care providers, noting lichen planus in the oral cavity of our patients (or elsewhere) should alert our attention to the possible necessity of collaboration and referral with the patient’s primary physician or potentially a specialist. Always be aware of lesions that are not healing properly as well as location, shape, and changes in lesions. Though lichen planus can present as benign and even asymptomatic for many, it can result in further disease for some.
Before you leave, check out the Today’s RDH self-study CE courses. All courses are peer-reviewed and non-sponsored to focus solely on high-quality education. Click here now.
Listen to the Today’s RDH Dental Hygiene Podcast Below:
References
- Lichen Planus. (2021, March 9). Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/lichen-planus/symptoms-causes/syc-20351378
- Lavanya, N., Jayanthi, P., Rao, U.K., Ranganathan, K. Oral Lichen Planus: An Update on Pathogenesis and Treatment. Journal of Oral and Maxillofacial Pathology. 2011; 15(2): 127-132. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3329692/
- Katta, R. Lichen Planus. American Family Physician. 2000; 61(11): 3319-3324. https://www.aafp.org/afp/2000/0601/p3319.html
- Gall, R., Navarro-Fernandez, I.N. (2021, July 30). Lichen Planus Erosive Form. StatPearls. https://www.ncbi.nlm.nih.gov/books/NBK560700/
- Giuliani, M., Troiano, G., Cordaro, M., et al. Rate of Malignant Transformation of Oral Lichen Planus: A Systematic Review. Oral Diseases. 2019; 25(3): 693-709. https://pubmed.ncbi.nlm.nih.gov/29738106/