Are you in need of CE credits? If so, check out our peer-reviewed, self-study CE courses here.
Test Your Oral Cancer Screening Knowledge
1. Approximately, what percentage of individuals in the United States receive an oral cancer examination?
While high-risk individuals tend to visit their physician more frequently than their dentist, they are less likely to receive a visual and tactile oral cancer examination in a medical office. Conversely, dentists are more likely to perform an oral cancer examination but less likely than physicians to provide risk-factor counseling, such as tobacco cessation.1
Overall, only about 20% of individuals in the United States receive a regular oral cancer examination. This low rate is even more pronounced among Black and Hispanic patients, as well as those with lower levels of education, possibly due to a lack of general access to care.1
Reference
1. Oral Cavity and Nasopharyngeal Cancers Screening (PDQ) – Health Professional Version. (2025, April 14). NIH: National Cancer Institute. https://www.cancer.gov/types/head-and-neck/hp/oral-screening-pdq
2. A comprehensive head and neck cancer examination includes visual and tactile extraoral and intraoral assessments. Because the skin extends beyond the head and neck, its assessment during an extraoral examination is unnecessary.
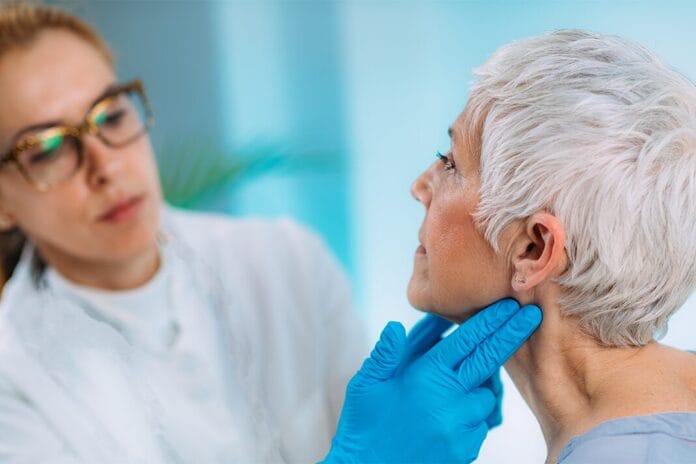
A comprehensive head and neck examination primarily consists of visual inspection with tactile palpation. The exam begins the moment you meet the patient, noting any facial asymmetry, masses, skin lesions, facial paralysis, swelling, or temporal wasting. Listening to them speak is also an important diagnostic step, as a "hot potato," raspy, or hoarse voice can be an early clinical sign of oropharyngeal tumor or laryngeal neoplasms.1
The examination should follow a systematic workflow to ensure no structures are missed:
- Extraoral assessment: An evaluation of the patient's general characteristics, including the skin, eyes, nose, and ears. This is followed by palpation of the thyroid gland and the lymph nodes.
- Intraoral exam: A thorough check of the lips, buccal mucosa, floor of the mouth, gingiva, palate, and tongue. The tongue should be extended with gauze to inspect the lateral borders, followed by a palpation of the floor of the mouth and salivary glands.
- Oropharyngeal inspection: Direct visualization of the soft palate, tonsillar pillars, the posterior pharyngeal wall, and base of the tongue. Examining the base of the tongue may require a laryngeal mirror.
- Referral needs: While the nasopharynx, hypopharynx, and larynx are part of the broader head and neck system, these deeper structures typically require specialized instruments, such as a laryngeal mirror or a fiber optic scope, often warranting a referral when persistent symptoms (like hoarseness) are present.1
Reference
1. Cancer Screening Protocols. (n.d.). Oral Cancer Foundation. https://oralcancerfoundation.org/discovery-diagnosis/cancer-screening-protocols/
3. What is the most frequently involved site for oral squamous cell carcinoma to develop?
While the lips have historically been the primary site for oral squamous cell carcinoma (SCC), newer data show the distribution has shifted. The tongue is now recognized as the most frequently involved subsite, accounting for approximately 41.7% of cases. The hard palate, by contrast, remains the least common site for SCC, accounting for only 2.3% of all cases.1
Distribution of oral SCC by subsite:
- Tongue: 41.7%
- Lip and floor of the mouth: 16.5% each
- Gingiva: 10.6%
- Buccal mucosa: 6.7%
- Retromolar trigone: 5.6%
- Hard palate: 2.3%1
Reference
1. Stepan, K.O., Mazul, A.L., Larson, J., et al. Changing Epidemiology of Oral Cavity Cancer in the United States. Otolaryngol Head Neck Surg. 2023; 168(4): 761-768. https://pmc.ncbi.nlm.nih.gov/articles/PMC10154079/
4. Dental clinicians only need to conduct a head and neck examination at every appointment for patients with risk factors for oral cavity and oropharyngeal cancer.
Every dental appointment should include a comprehensive review of the patient's medical, dental, and social history, alongside a thorough head and neck examination. While this examination is universal, clinicians should be exceptionally vigilant with patients who exhibit high-risk behaviors.1
Because squamous cell carcinoma (SCC) accounts for approximately 90% of all oral cavity and oropharyngeal cancers, understanding the major risk factors may improve early detection:1
- Behavioral and lifestyle: Tobacco and alcohol risk are dose-dependent. However, using both together creates a synergistic effect that increases the risk of developing oral cavity and oropharyngeal SCC. Often practiced in Asian, Migrant Asian, and other communities, chewing betel quid ("paan") is also a risk factor.1,2
- Environmental and demographic: UV exposure is the likely risk factor associated with lip SCC. Risk also increases with age and is historically more prevalent in males.1
- Viral and genetics: Human papillomavirus (HPV) infections (especially HPV-16) are specifically associated with the rise in oropharyngeal SCC.1 Epstein-Barr virus (EBV) can contribute to the development of nasopharyngeal cancer in specific geographical regions.3 Rare hereditary disorders, such as Fanconi anemia, also increase the risk of developing oral cavity and oropharyngeal SCC.1
References
1. Cancer (Head and Neck). (2026, March 17). American Dental Association. https://www.ada.org/resources/ada-library/oral-health-topics/cancer-head-and-neck/
2. The American Cancer Society Medical and Editorial Content Team. (2021, March 23). Risk Factors for Oral Cavity and Oropharyngeal Cancers. American Cancer Society. https://www.cancer.org/cancer/types/oral-cavity-and-oropharyngeal-cancer/causes-risks-prevention/risk-factors.html
3. Oral Cavity and Nasopharyngeal Cancers Screening (PDQ) – Health Professional Version. (2025, April 14). NIH: National Cancer Institute. https://www.cancer.gov/types/head-and-neck/hp/oral-screening-pdq
5. What procedure is recognized as the gold standard for the definitive diagnosis of oral cancer?
In 2026, an estimated 60,480 new cases of oral cavity and oropharyngeal cancer will be diagnosed in the United States. With approximately 13,150 deaths projected for the year, these cancers are expected to claim roughly one life every 40 minutes.1
To reduce this rate of morbidity and mortality, identifying mucosal abnormalities at an early stage and reaching a definitive diagnosis is critical. Currently, the gold standard for definitive diagnosis remains a punch or surgical biopsy followed by a histopathological review.2 Accordingly, any adult patient presenting with a suspicious lesion should undergo a biopsy immediately.3
There is a caveat to the use of cytological adjuncts: they are not a substitute for a traditional biopsy. Instead, they serve as a diagnostic aid when a biopsy is not advisable, not possible, or not indicated. In specific situations, including patient preferences, when a biopsy is too risky, or the site is not easily accessible, a cytological adjunct can further inform the need for biopsy.2
References
1. The American Cancer Society Medical and Editorial Content Team. (2026, January 13). Key Statistics for Oral Cavity and Oropharyngeal Cancer. American Cancer Society. https://www.cancer.org/cancer/types/oral-cavity-and-oropharyngeal-cancer/about/key-statistics.html
2. Urquhart, O., Bhosale, A.S., Martins-Pfeifer, C., et al. Living Evidence-Informed Guideline on the Early Detection of Oral Squamous Cell Carcinoma and Potentially Malignant Disorders: Cytology Adjuncts to Determine the Need for Biopsy, Version 2026 1.0. J Am Dent Assoc. 2026; 157(3): 224-234. https://jada.ada.org/article/S0002-8177(26)00037-1/fulltext
3. Cancer (Head and Neck). (2026, March 17). American Dental Association. https://www.ada.org/resources/ada-library/oral-health-topics/cancer-head-and-neck/