Some people claim that the eyes are the window to the soul. As a dental professional, have you ever thought that the tongue and mouth are the window to your patient’s health? We can gain quite a bit of insight and information about our dental patients just by a thorough exam of the tongue, mucosa, and surrounding structures of the oral cavity.
Hopefully, you are already completing oral cancer evaluations at your patient’s hygiene visits; if not, I urge you to begin. Oral cancer is a profoundly serious cancer. The most recent statistics from The American Cancer Society estimated 54,010 new cases of oral cavity or oropharyngeal cancer in the United States each year, with approximately 10,850 deaths resulting from oral cavity or oropharyngeal cancer.1 So, it really is that important to do the oral cancer exams at each appointment; you could help save a life.
Aside from cancer, numerous other systemic diseases can manifest in the oral cavity. As a dental hygienist, you are in a perfect position to recognize the change or abnormality first, alerting the patient to what could be a bigger nondental issue. I will not be able to list all the systemic disorders that could possibly manifest in the oral cavity, but I will try to highlight several that may be more common.
Common Examples of Systemic Disorders
Thrush or oral candidiasis (see Image 1) causes creamy, white lesions, usually on the tongue or buccal mucosa. It is common in infants and can also be related to the use of antibiotics, wearing dentures, xerostomia, use of corticosteroids, or overuse of mouthwash in adults. Research shows that candida is a normal organism in your mouth, and normally our bodies keep the organism in balance, so it is not a problem. But sometimes, it can overgrow and cause more severe symptoms when other systemic issues are present.
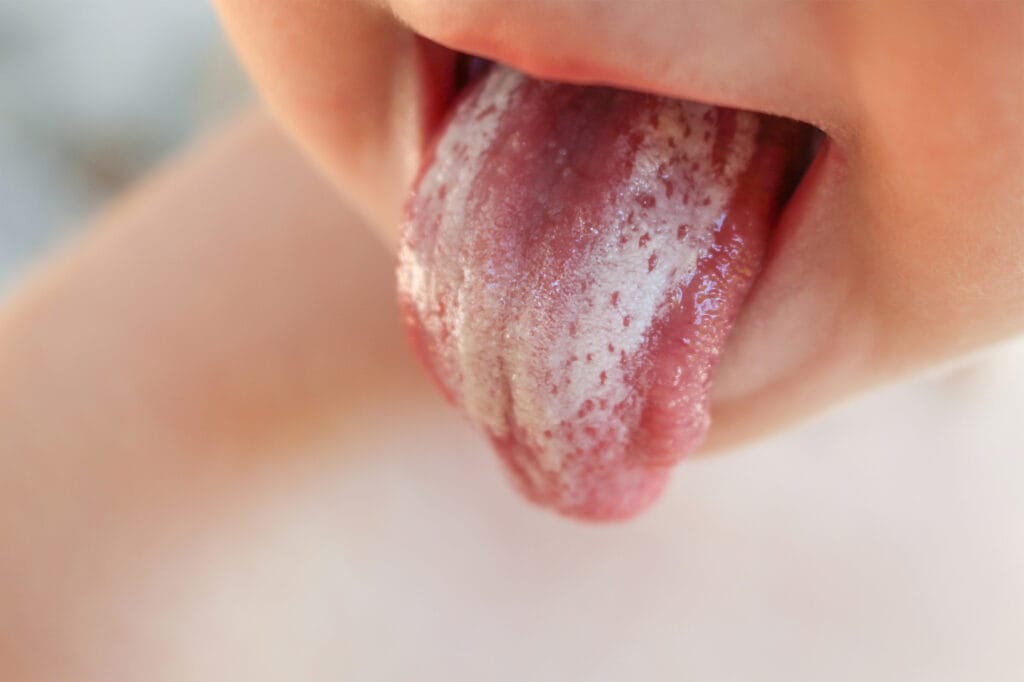
Patients with weakened immune systems such as diabetes, cancer, HIV, or leukemia have less ability for the body to fight pathogens and, coupled with diabetic patients’ higher glucose levels, lead to a more favorable condition for candida to grow.2
If you notice candida, dig a little deeper with your patient to see if they have been recently diagnosed with another condition. If not, have a conversation with them about the possibility of an underlying medical condition and refer to their primary care physician if warranted. The treatment for candidiasis in the mouth, throat, or esophagus is usually an antifungal medicine for seven to 14 days. Medications include clotrimazole, miconazole, or nystatin. For severe infections, the most common treatment is fluconazole (an antifungal medication) taken by mouth or through a vein.2
Atrophic glossitis, (see image here) which is also identified as smooth tongue because of a smooth, glossy appearance with a red or pink background. According to the American Academy of Family Physicians, the smooth quality of the tongue is caused by the atrophy of filiform papillae.
It is often linked to an underlying nutritional deficiency of iron, folic acid, vitamin B12, riboflavin, or niacin. Other etiologies include systemic infection (e.g., syphilis), localized infection (e.g., candida), amyloidosis, celiac disease, and xerostomia triggered by some medications and Sjögren syndrome.
It is interesting to note that there seems to be a cause-and-effect between nutrient deficiencies and atrophic glossitis. Nutrient deficiencies cause atrophic glossitis; however, atrophic glossitis contributes to nutrient deficiencies as well. It is well understood how nutrient deficiencies cause atrophic glossitis, but the symptoms associated with it often reduce the intake of nutrients, causing further nutrient deficiencies, leading to a never-ending cycle that prolongs atrophic glossitis.7
The tongue can also be very sore or cause patients a painful sensation. Replacement of the missing nutrient or treatment of the possible underlying condition can treat the glossitis.3 After co-diagnosis with your dentist and discussion with the patient, refer to their primary care physician to evaluate the patient.
Deep linear ulcerations are some of the visible oral signs of Crohn’s disease, which is an inflammatory bowel disease. The ulcers are not uncommon, especially in pediatric populations, and are maybe the first signs of the disease. As the dental hygienist, you could be the first health care provider to see these signs and alert the patient.
Authors in an Inflammatory Bowel Diseases article noted, “Visible oral manifestations include cobblestone appearance of the mucosa, deep linear ulcerations, and mucosal tags. Other signs may include swelling of the lips, angular cheilitis, hyperplasia of erythematous gingiva, and recurrent ulcerations. Orofacial granulomatosis may be an early indicator of Crohn’s disease even without intestinal symptoms.”4
Patients that present with any of those signs should be referred for evaluation. Medications can be prescribed by the treating physician that suppresses the immune system’s abnormal inflammatory response and offers relief of symptoms.
Violet or brown tumors may be linked to Kaposi’s sarcoma (see Image 2), “a rare type of cancer caused by a virus called Kaposi sarcoma─associated herpesvirus (KSHV), also known as human herpesvirus 8 (HHV8). KSHV is in the same family as the Epstein-Barr virus (EBV), the virus that causes infectious mononucleosis (mono) and is linked to several types of cancer. The cancer develops from the cells that line lymph or blood vessels. It usually appears as tumors on the skin or mucosal surfaces such as inside the mouth as violet or brown, red plaques or tumors of the tongue, palate, and gingivae, but these tumors can also develop in other parts of the body, such as in the lymph nodes, the lungs, or digestive tract.
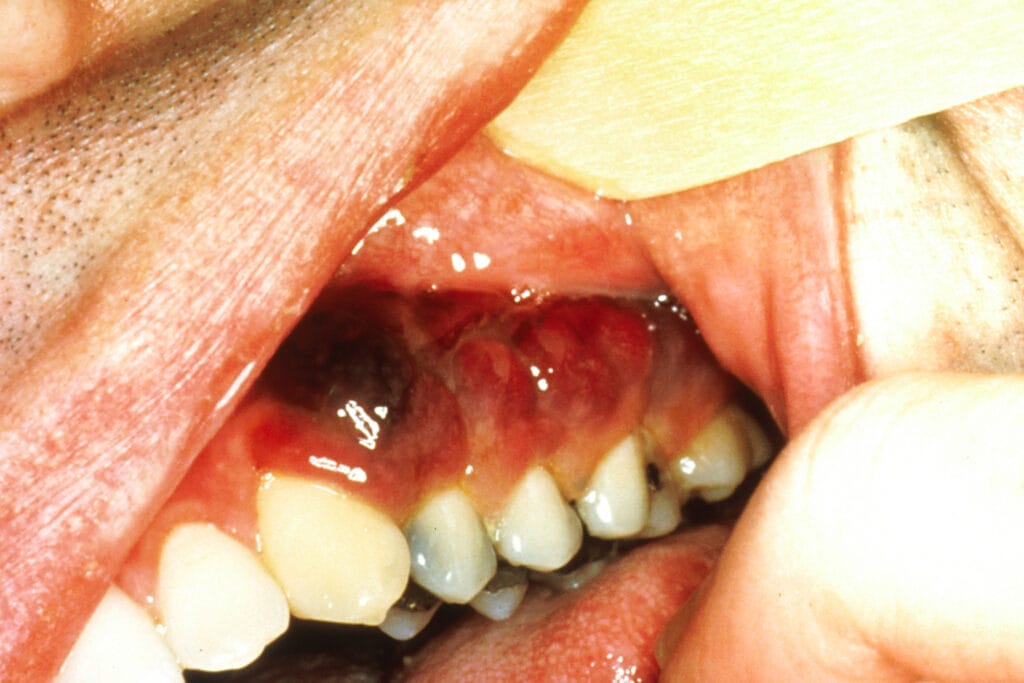
There are at least five different types of Kaposi sarcoma, including 1) epidemic (AIDS-associated), which is the most common in the United States. 2) classic (Mediterranean). 3) endemic (African). 4) iatrogenic (transplant-related), and 5) HHV8 (Human Herpesvirus 8).”5
If you notice these lesions during an examination, please discuss a referral with the patient to determine the etiology and seek treatment which usually consists of antiretrovirals, chemotherapy or radiation therapy.
Blisters and bullae are common with pemphigus vulgaris (see Image 3), an autoimmune disease where the immune system produces antibodies against proteins in the skin and mucous membranes.
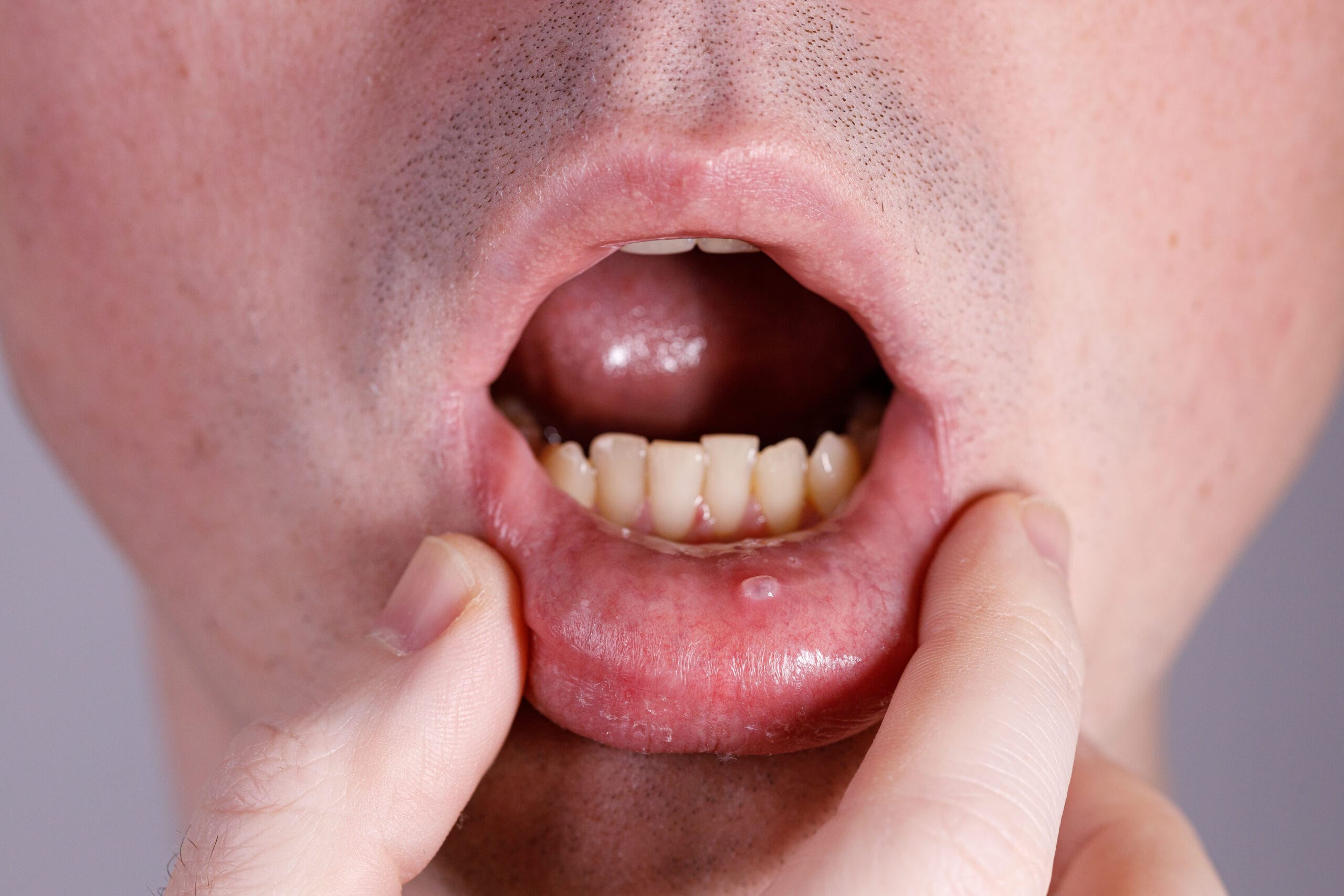
The authors of an article in Case Reports in Dentistry noted, “Antibodies break bonds between cells leading to the formation of skin blisters. It is a potentially fatal dermatosis with both cutaneous and oral manifestations; they appear as blisters that rupture rapidly, resulting in painful erosions. Buccal mucosa, lips, and soft palate are most involved. Their manifestations in the oral cavity often precede those on the skin by many months or may remain as the only symptoms of the disease.”
Pemphigus usually affects patients in the fourth and fifth decades of life, with females reportedly being affected more frequently than males. More than 50% of the affected patients have been reported with initial manifestations on the oral mucosa followed by skin involvement. The average duration of the oral lesions is found to be between three months and one year.6
Again, keen observations are key! You could be the first to see these lesions, and it is vitally important that the oral manifestations of the disease are recognized on time to make a proper diagnosis and initiate timely treatment.
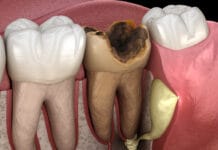
Chalkiness of enamel usually is present clinically first with bulimia nervosa patients. Bulimia nervosa is a serious and potentially life-threatening eating disorder. Many people with this disease will secretly binge eat large quantities of food and then later purge in an attempt to rid their system of the extra calories for fear of gaining weight.
Other clinical signs include decay, sensitivity, painful bleeding gingiva, erosion, swollen salivary glands due to frequent self-induced vomiting, and the tissues of the mouth and tongue may be dry, red, and sore. Also, be aware that patients with bulimia may have chronic sore throats, and hemorrhages under the skin of the palate can be visible. Not only does bulimia negatively affect your oral health but your overall general health as well. If you notice these signs, please have a discussion with your patient about the cause and effect of this disease.
Many other clues in the mouth may indicate impactful habits or problems your patients may be having. We are all aware of the link between healthy gingiva and a healthy heart, which is always valuable information to share with your periodontal patients. Xerostomia or dry mouth may present for several reasons, the normal aging process, medications, stress, and anxiety, including depression. Diabetes may also affect the production of saliva. There are several products available to our patients to help relieve the effects of xerostomia, so please have a conversation with them on ways to help.
Bruxism, which can be seen clinically due to attrition, chipped or loose teeth and scalloped tongue and may be a result of anxiety, stress or tension. Diseases such as dementia and epilepsy may increase a patient’s risk for bruxism which can lead to TMJ problems or a sleep disorder. Those cervical abrasions and whitish wrinkled patches of buccal mucosa let us know the patient uses snuff, and we should always have the blunt but caring talk about oral cancer and the increased risk that smokeless tobacco presents. And, the list goes on and on.
In closing, remember that hygienists help play a vital role in the early detection of possible underlying medical conditions or autoimmune diseases of our patients. It is our responsibility to refer our patients to the proper medical or dental colleagues for further evaluations and the best possible care for our patients.
Before you leave, check out the Today’s RDH self-study CE courses. All courses are peer-reviewed and non-sponsored to focus solely on pure education. Click here now.
Listen to the Today’s RDH Dental Hygiene Podcast Below:
References
- American Cancer Society (2021). Key Statistics for Oral Cavity and Oropharyngeal Cancer. Retrieved from https://www.cancer.org/cancer/oral-cavity-and-oropharyngeal-cancer/about/key-statistics.html
- Centers for Disease Control and Prevention. Fungal Diseases. Candida Infections of the Mouth, Throat, and Esophagus. Retrieved from https://www.cdc.gov/fungal/diseases/candidiasis/thrush/index.html
- Common Tongue Conditions in Primary Care. Am Fam Physician. 2010 Mar 1;81(5):627-634. https://www.aafp.org/afp/2010/0301/p627.html
- Rowland, M., Fleming, P., Bourke, B. Looking in the Mouth for Chohn’s Disease. Lippincott, Williams & Wilkins. 2010; 16(2): 332-7. Retrieved from https://www.researchgate.net/publication/26765510_Looking_in_the_Mouth_for_Crohn’s_Disease
- Kaposi Sarcoma Treatment – Health Professional Version. (2018, July 27). NIH: National Cancer Institute. Retrieved from https://www.cancer.gov/types/soft-tissue-sarcoma/hp/kaposi-treatment-pdq
- Kuriachan, D., Suresh, R., Janardhanan, M., Savithri, V. Oral Lesions: The Clue to Diagnosis of Pemphigus Vulgaris. Case Reports in Dentistry. 2015; 2015(Article ID 593940). Retrieved from https://doi.org/10.1155/2015/593940
- Chiang, C.P., Chang, J.Y., Wang, Y.P., Wu, Y.H., Wu, Y.C., Sun, A. Atrophic Glossitis: Etiology, Serum Autoantibodies, Anemia, Hematinic Deficiencies, Hyperhomocysteinemia, and Management. J Formos Med Assoc. 2020 Apr; 119(4): 774-780. doi: 10.1016/j.jfma.2019.04.015. Epub 2019 May 8. PMID: 31076315.