I can still see the faces of the patients who stumped me the most. They are people who I thought were going to be my biggest success stories but weren’t. They presented with halitosis, visible staining and calculus, dark red, inflamed gingiva, and were in just the initial stages of periodontal disease. They were otherwise healthy, successful people, and I was going to save them from the scourge of periodontal disease.
Of course, this is what they want, I thought. Look at how impeccably dressed and groomed they are. They looked so put together until they opened their mouth. Early in my career, I would present their treatment plans almost as an afterthought. Obviously, they were interested in fixing their mouths, and I was just the dental hygienist to do it.
But they didn’t seem interested in their disease and were ambivalent about any treatment. They were just there for a cleaning.
Evolving Patient Education
Initially, I figured they hadn’t really heard what I had just told them about their mouths. Maybe if I threw in some facts about tooth loss, it would hit home to them.
Nope. OK, I had just the thing. I would do such a great job of cleaning them up that the results would speak volumes. But I never got the results that I was hoping for because home care didn’t change, habits didn’t change, and I didn’t change my approach.
Over time, I became more adept at reading my patients and discovering their motivations. I began to focus on a holistic approach to health and the oral-systemic link. My patient education evolved to become much more individualized.
To do this, I talked with the people in my chair. More importantly, I listened to them. Soon I was tying any oral manifestations to their systemic concerns. Patients who were once quiet and guarded began to share information that was pertinent to their long-term oral health. It was amazing how people who did not originally have any chief complaints were soon sharing their concerns about their breath, the color of their teeth, and wanting to know why their gums bleed when they brush.
Something as simple as tying a brochure about bone loss to the patient’s own radiographs became the precursor to a lightbulb moment. I would show them the brochure and explain the disease process and then have them turn and look at their radiographs. Then I would ask them to find anything that resembled something they had just learned. It is amazing how well people can interpret bone loss after a few minutes. The ownership they have when they find the signs on their specific radiographs is game-changing. As ownership of their disease increased, the results of treatment improved.
As I became more adept at individualizing my approach to patient education, the acceptance rate for nonsurgical periodontal therapy and recare appointments skyrocketed.
Stop, Drop, and Roll
In school, we had role-played under the watchful eyes of our instructors about how to talk to patients about their oral health. A significant amount of time was spent learning to negotiate difficult patients and how to de-escalate their frustration surrounding suggested treatment, including cost and the necessity of the treatment.
While this does come up in private practice, I found that it wasn’t nearly as often as I would have thought. Kind of like how many times I learned that if I was on fire, I should stop, drop, and roll. Luckily, this information has been useless to me up to this point. I will truly value the knowledge if I ever do catch on fire, though, just like learning how to communicate with difficult patients proves handy occasionally.
What baffled me was the ambivalent patient and the apathetic patient. I met those people much more often. They are the people who tell you, “My mom lost her teeth at 22, so what can I do? Genetics, right?” I heard that statement or “my family just have bad teeth” on a weekly basis. People who had given up their power and ownership of their health because they accepted what they felt was inevitable.
Obviously, sometimes this is just ignorance of the facts and simple to rectify. But sometimes it is just easier for people to feel powerless because then they are not responsible for any outcomes. If you never had a chance, it is easier to not really try. Expectations of failure lead to failure. Expectations are ghosts from the past and future that distract us from the present.
As you get your patients to let go of the belief that there is some preordained way that things are supposed to be, you create an environment of authenticity that allows things to be whatever they really are. You return the power, and the responsibility to the person, freeing them from predetermined outcomes.
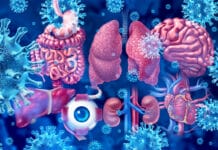
As health providers, it is essential that we understand the need for connection. Patients need to connect signs, symptoms, habits, and home care to their oral health. They then need to connect their oral health to their overall health. And to do this, they really need to connect to you, their dental hygienist. Insurance companies have convinced people that their teeth and eyes are somehow not a part of their bodies. They will pay for a hurt toe, but treating teeth and eyes is not their concern. You must get two more insurance plans if you feel the need to eat or see.
As holistic approaches to health and wellness increase in popularity, it is getting easier for dental hygienists to introduce the oral-systemic link. Talk to your patients about their physical, mental, and oral health. Include them in developing a care plan and maintenance intervals. Train them to recognize signs of disease. Help them find their own motivation to care about their oral health because you can’t want it for them.
Before you leave, check out the Today’s RDH self-study CE courses. All courses are peer-reviewed and non-sponsored to focus solely on high-quality education. Click here now.