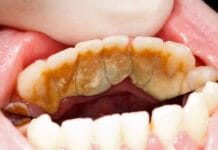
Chronic periodontitis is a chronic inflammation of the gum tissues, caused by an excess of dental plaque and the body’s immune response to the harmful bacteria. Over time, it causes loss of bone and soft tissues, and evidence exists that links chronic periodontitis with an increased risk of certain cancers, rheumatoid arthritis, and even Alzheimer’s Disease.
Periodontitis is a common health problem, affecting nearly half of Americans over the age of 30, and more than 70% of adults over the age of 65. As much as 35% of the US population suffers from severe chronic periodontitis. Unfortunately, although early detection can prevent bone and tooth loss because this disease progresses without pain or significant symptoms, it is often far advanced before patients seek treatment. Worldwide, the estimated economic impact of periodontitis amounts to more than $54 billion per year in lost productivity, and periodontitis is a major contributor to the total $442 billion spent every year on oral diseases.
Standard treatment for periodontitis is scaling and root planing.
However, because periodontitis is caused by several different contributing factors, scaling and root planing are only effective when combined with ongoing patient oral care practices, and in the absence of contributing health factors like stress, diabetes, occlusal trauma, or cigarette smoking. Successful long-term management of periodontitis can be a challenge for dental professionals and patients alike, and as many as 20-30% of patients do not respond favorably to traditional treatment methods.
In recent years, dentists and hygienists have been looking beyond mechanical treatment, to seek to address the many causes of chronic periodontitis and manage the disease more effectively. Antibiotics have been shown to have an additional benefit in many cases, but they significantly increase the risk of antibiotic resistance in subgingival flora and should be avoided when unnecessary. Lasers show promise, especially for soft tissue procedures, but there is not yet sufficient evidence that they are more effective for long-term treatment of chronic periodontitis than SRP. Open-flap debridement is highly effective for mechanically cleaning deep pockets, but the expense and risk of surgery should be considered carefully.
However, 2018 could bring the first clinical trials for a groundbreaking periodontitis vaccine. For 15 years, researchers at the Oral Health CRC at the University of Melbourne have been working on a vaccine, which was finally proven to be effective in mice.
Traditionally, the challenge of using antimicrobial treatments for periodontitis have been:
- a) the oral cavity hosts a complex ecosystem of bacteria, many of which are essential for health and
- b) plaque and periodontitis-causing bacteria live within a biofilm, in which they are physiologically distinct from planktonic cells of the same organism. The functional community of a biofilm is difficult to disrupt without systemic disruption.
The team at the University of Melbourne chose instead to specifically target the bacterium Porphyromonas gingivalis. P. gingivalis is a keystone pathogen in periodontitis, instrumental in forming the biofilm, and levels above the 10-15% threshold of total bacterial load have been demonstrated to predict imminent attachment loss. Previous studies have shown that high levels of P. gingivalis at the site of prior SRP treatments are predictors of the ongoing progression of the disease.
By developing a vaccine that specifically targets P. gingivalis, the team hopes to create a vaccine that triggers the body’s immune system to react and fight this specific, destructive bacteria and disrupt the progression of periodontitis.
In mice, their vaccine has been shown to prevent the dominance of P. gingivalis in subgingival plaque above threshold levels that cause and disease. In 2018, they will begin testing the vaccine in human clinical trials.
A vaccine for periodontitis would be incredibly important since so many people suffer from the disease and don’t seek treatment until they are risking tooth loss. And it would be critical for the 20-30% of people who suffer from chronic periodontitis despite SRP treatments.