The profession of dental hygiene is continuously evolving to address the needs of varying populations through medical-dental integration and increased access to care. Currently, a need exists to facilitate discussion and promote increased collaboration between speech-language pathologists, oral health professionals, and other health care professionals involved in the management of patients with dysphagia.
Dental interventions provided to patients with dysphagia can be complementary to and consistent with the goals of treatment developed by speech-language pathologists. Minor adaptations to conventional treatment can assist patients with swallowing difficulties to comfortably receive the dental treatment they require.1
What is Dysphagia?
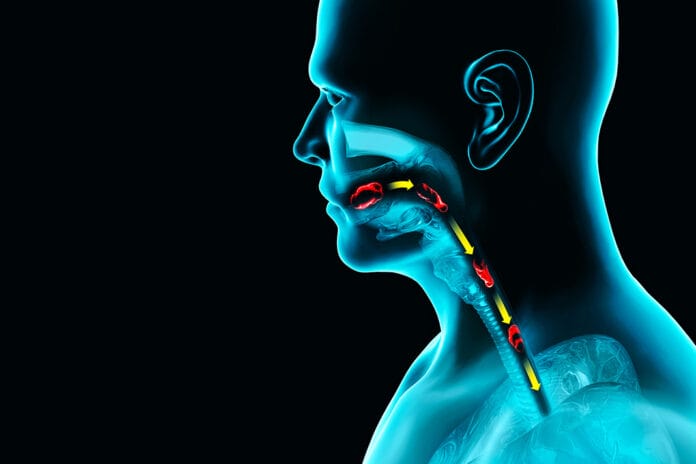
Dysphagia occurs when there is a problem with the neural control or the structures involved in any part of the swallowing process. Swallowing is a complex process made up of 50 pairs of muscles and many nerves that work to receive food into the mouth, prepare it, and move it from the mouth to the stomach.2
Dysphagia is found in one in 25 adults in the United States.3 Between 70% to 90% of older people have some degree of swallowing dysfunction.4 People with dysphagia have difficulty swallowing and may even experience pain with swallowing. Some people may be completely unable to swallow or may have trouble safely swallowing liquids, foods, and saliva.2
Dysphagia may make it difficult to take in enough calories and fluids to nourish the body and can lead to additional medical problems.2
Causes of Dysphagia
Dysphagia is a symptom of various underlying medical conditions and can be attributed to age-related changes and neurological, cognitive, respiratory, and gastrointestinal diseases. These conditions may cause anatomical and functional changes along the swallowing tract.3
Dysphagia is most frequently found in older adults. Any condition that weakens or damages the muscles and nerves used for swallowing, however, may cause dysphagia. Examples include cerebral palsy, Parkinson’s disease, stroke, or head injury. People born with abnormalities of the swallowing mechanism (such as a cleft palate) may not be able to swallow normally.4
Cancer of the head, neck, or esophagus as well as the treatment for these cancers, may cause swallowing problems. Dementia, memory loss, and cognitive decline may make it more difficult to chew and swallow.4 Swallowing difficulties resulting from cognitive issues may stem from varying levels of alertness, reduced awareness of food or fluid in the oral cavity, and decreased sensory processing.3
Several types of medications can contribute to dysphasia. Oxybutynin and tolterodine affect the musculature of the esophagus. Diuretics, calcium channel blockers, and antihistamines can cause xerostomia and impair the ability to move food within the oral cavity. Antipsychotic and neuroleptic drugs (haloperidol, risperidone, and clozapine) can also cause xerostomia, and some can cause movement disorders, which may affect the muscles of the face and tongue used in swallowing.4
Anti-epileptic medications, benzodiazepines, narcotics, and smooth muscle relaxants used to relieve severe muscle spasms decrease voluntary muscle control, which may affect swallowing.4
Diagnosis and Treatment of Dysphagia
Dental professionals may help patients recognize the first signs of dysphagia and provide a referral to a speech-language pathologist for diagnosis. Different treatments for the types of dysphagia and a variety of tests look at the stages of the swallowing process to assess where the issue is.2
The flexible endoscopic evaluation of swallowing with sensory testing (FEESST) uses a lighted fiberoptic tube, or endoscope, to view the mouth and throat while examining how the swallowing mechanism responds to stimuli such as a puff of air, food, or liquids.2
A videofluoroscopy (VFS) is a test in which a clinician takes a videotaped x-ray of the entire swallowing process by having a patient consume several foods or liquids along with the mineral barium to improve the visibility of the digestive tract. The images help identify where in the swallowing process the issue is. This test takes approximately 15 minutes and is available in most hospitals.2
These tests help speech-language pathologists determine what changes can be made to offer a safe swallowing strategy. Broad intervention techniques include restoration of normal swallow function via rehabilitative exercises and changes to diet consistency and patient behavior.3 Changes may be in food texture, size, head or neck posture, or behavioral maneuvers such as a chin-tuck.2
If these interventions do not help, medical or surgical intervention may be necessary. In progressive conditions such as amyotrophic lateral sclerosis (ALS), a feeding tube in the stomach may be needed long-term.2
Oral Health Issues Associated with Dysphagia
Many approaches used in the management of oral and pharyngeal dysphagia can place the oral cavity at greater risk of disease. Dietary modification techniques used to alter bolus or liquid flow and compensate for inadequate swallowing function can increase oral retention. In doing so, this approach may facilitate the growth of oral microorganisms that lead to dental decay.1
Prolonged accumulation of plaque will also increase a patient’s risk of forming periodontal disease.1
Regular oral care is important in mitigating the problems associated with dysphagia, particularly for patients at risk of aspiration.1 Food or liquid that stays in the airway may enter the lungs and allow harmful bacteria to grow, resulting in aspiration pneumonia.2 Maintenance of good oral health has been shown to decrease the risk of aspiration pneumonia across several clinical settings ranging from residential aged-care facilities to neurologic intensive care units.1
Dysphagia is recognized as a risk factor for aspiration pneumonia. However, studies have shown that it alone is generally not enough to cause pneumonia unless other risk factors are also present. These risk factors include poor oral hygiene, periodontal disease, untreated dental caries, and nocturnal denture wearing.1
Due to the increased oral microbial burdens, nocturnal denture wearing has been found to present a comparable risk of developing pneumonia as a history of swallowing difficulties, stroke, or respiratory disease.1
Masticatory performance reflects the capacity to reduce the size of food particles and the number of chews necessary to render food ready for swallowing. It is affected by the number of teeth in functional occlusion, the maximal biting force, and denture wearing. The salivary flow rate also affects masticatory performance, which declines with a reduction in salivary flow.5
Tooth loss is directly related to the deterioration of swallowing function by influencing the oral preparatory stage of swallowing. Chewing ability is dependent on the number of remaining teeth; therefore, tooth loss can be expected to indirectly disturb the coordinated execution of pre-swallow and swallowing behaviors.5
Saliva facilitates speech, lubricates mucosa, facilitates mastication and swallowing food and bacterial clearance, and cleanses the oral cavity. The dryness of the mouth affects both the oral phases of swallowing and can lead to impaired bolus formation and oropharyngeal bolus transport. A decrease in saliva secretion is frequently accompanied by swallowing problems and is common in older people, with incidence ranging from 20% to as high as 60%.5
Dental Treatment Considerations for Patients with Dysphagia
Given the diverse etiologies that may result in swallowing difficulties, a single management strategy is unlikely to be effective. A dental professional’s role is to complete an oral assessment to determine the presence of oral pathology and treatment needs, evaluate current oral hygiene, make recommendations to the patient and other health professionals involved in management regarding appropriate oral care, introduce and demonstrate oral hygiene techniques to the patient, and review oral health and oral hygiene on a regular basis.1
Dental health history forms should include questions about dysphagia. Dental hygienists may ask how long the condition has been present, the degree of severity, and what if any, treatment options have been implemented. Follow-up is needed at each visit to track the progression of the condition.3 Dental professionals should be aware of complications such as frequent choking, gagging, inability to control saliva, nasal regurgitation, and coughing.4
The major concern is aspiration during dental treatment. To avoid aspiration, treat the patient sitting upright or no more than a 45-degree incline. Allow frequent breaks, protect the airway with a rubber dam, and use high-volume evacuation. Reduce handpiece water flow, and during hygiene appointments, use ultrasonics minimally with high-volume evacuation or hand scaling only. Shorter recall appointments of 3-4 months may be beneficial.4
Keep in mind that local anesthetic use in the posterior may exacerbate swallowing issues; use local infiltration rather than nerve blocks.4
Oral Health Recommendations for Patients with Dysphagia
Due to the variety of protocols presented in the literature and the diversity of the etiologies associated with dysphagia, no definitive oral care or oral hygiene regimen can be applied to all patients with dysphagia. The two main objectives are mechanical cleansing and reducing the risk factors of dental decay.1
Mechanical cleansing is achieved primarily through toothbrushing. Encourage patients to use an electric toothbrush, floss, and interdental brushes. If there is a concern with the ability to manage thin fluids, a damp toothbrush or interdental brush can be used. If a patient is unable to expectorate or has postural/positioning concerns, a piece of gauze or an oral swab can be used to remove debris.1
To reduce risk factors of dental decay, patients with dysphagia should be encouraged to use a toothpaste with higher fluoride content greater than 1000 ppm and one that has reduced or no sodium lauryl sulfate (SLS) or other foaming agents such as cocamidopropyl betaine (CAPB).1
Individualized oral hygiene recommendations should consider the patient’s medical status, the nature and degree of swallowing impairment, oral versus non-oral nutrition, the degree of diet modification (food and fluids), neurological deficits affecting oral musculature, oral symptoms and their management (xerostomia), risk status for decay and periodontal disease, and concomitant conditions (physical disability, intellectual disability, complex communication needs, sensory impairment).1
John Ashford, PhD, CCC-SLP, states, “Oral hygiene is often thought of as a ‘care’ like bathing or hair brushing. It is not. It is an infection control procedure for patients. Oral hygiene is just as important for patients who are fed by tube as those who are fed orally.”6
Reduced oral intake may result in a reduction of nutritive sources for oral bacteria, reducing dental decay. However, mastication and fluid intake that usually disturb plaque deposits are absent when non-oral feeding is implemented, resulting in an increased build-up of calculus and resultant periodontal disease.1
The degree of swallowing impairment in relation to oral hygiene recommendations is discussed in Table 1.
| Dysphagia Severity | Oral Hygiene Recommendations |
| Minimal dysphagia | Normal oral hygiene: Twice daily toothbrushing with fluoridated toothpaste.
Daily interdental cleaning. |
| Mild-moderate dysphagia | Toothbrushing: With high fluoride (>1000ppm) or low foaming toothpaste twice daily.
Interdental cleaning: Flossing or interdental brushes at least twice daily. |
| Moderate dysphagia | Toothbrushing: With high fluoride or low foaming toothpaste after each meal.
If the patient is unable to tolerate the foaming of toothpaste, follow measures for severe dysphagia. |
| Moderately severe-severe dysphagia | Toothbrushing: Dry/damp, no toothpaste. Interdental care at least twice daily.
Topical application of fluoride product with swabbing to remove excess. |
Table 1 Oral hygiene recommendations based on dysphagia severity. Adapted from Lim1
The collaboration of dieticians, speech-language pathologists, oral health professionals, and caretakers alongside patients with dysphagia is essential in promoting good oral hygiene practices and mitigating associated risks. Each profession offers a unique perspective and expertise to maintain adequate nutrition and hydration while minimizing the risk of aspiration and supporting the quality of life for those with dysphagia.1
Before you leave, check out the Today’s RDH self-study CE courses. All courses are peer-reviewed and non-sponsored to focus solely on high-quality education. Click here now.
Listen to the Today’s RDH Dental Hygiene Podcast Below:
References
- Lim, M. Basic Oral Care for Patients with Dysphagia – A Special Needs Dentistry Perspective. Journal of Clinical Practice in Speech-Language Pathology. 2018; 20(3): 142-149. https://www.researchgate.net/publication/330926503_Basic_oral_care_for_patients_with_dysphagia_-_A_Special_Needs_Dentistry_perspective
- Dysphagia. (2017, March 6). NIH: National Institute on Deafness and Other Communication Disorders. https://www.nidcd.nih.gov/health/dysphagia
- Quek, H.C., Lee, Y. S. Dentistry Considerations for the Dysphagic Patient: Recognition of Condition and Management. Proceedings of Singapore Healthcare. 2019; 28(4): 288-292. https://doi.org/10.1177/2010105819868252
- Curl, C., Boyle, C. Dysphagia and Dentistry. Dental Update. 2014; 41(5): 413-422. https://www.dental-update.co.uk/content/special-care-dentistry/dysphagia-and-dentistry/
- Furuta, M., Yamashita, Y. Oral Health and Swallowing Problems. Current Physical Medicine and Rehabilitation Reports. 2013; 1(4): 216-222. https://doi.org/10.1007/s40141-013-0026-x
- Ashford, J. (2018, July 16). Oral Hygiene and Dysphagia – Care and Complications. American Speech-Language-Hearing Association. https://leader.pubs.asha.org/do/10.1044/oral-hygiene-and-dysphagia-care-and-complications/full/