Does anyone else feel terrible when a patient nervously asks, “Am I getting a shot?” and you have to break the news of several injections?
Maxillary quadrant anesthesia is often approached with a PSA, MSA, and multiple infiltrations over anterior teeth. While this is a valid approach, I prefer to minimize injections for my patients and anesthetize a maxillary quadrant with only two injections, the PSA for molars and the ASA for premolars and anterior teeth. The ASA nerve block can improve the experience for patients and clinicians.
The anterior superior alveolar nerve (ASA) injection is commonly called an IO, which stands for the infraorbital nerve. The IO nerve serves soft tissue, specifically the upper lip and gingiva, side of the nose, and lower eyelid. The ASA branches from the IO at the infraorbital foramen and innervates the teeth from maxillary central to mesiobuccal root of the first molar. This is true for 72% of people. In other patients, the middle superior alveolar nerve (MSA) is present and provides sensory information from the premolars. If the MSA is present, it also joins with the IO nerve at the foramen and will be blocked with an IO/ASA injection. For clarity, I will reference this nerve block as the ASA in this article, but either name is commonly understood and accepted.
The ASA nerve block is extremely useful for SRP procedures where half mouth anesthesia is desired, or for restorative procedures on more than 1-2 teeth in the region. There is a palatal approach to numbing these areas called the AMSA, but palatal injections are understandably not popular among patients or hygienists, so this article will focus on the standard ASA nerve block.
Anatomy
I still remember the horror that rippled through our hygiene school classroom when we heard about this injection. We were incredulous we would have to aim our needles at the eye! I believe this is a common concern among new and experienced clinicians, but while it feels strange, this injection is completely safe. The bony ridge of the orbit below the eye protects it by preventing us from advancing the needle too far. We will not be creating any pirates, I promise.
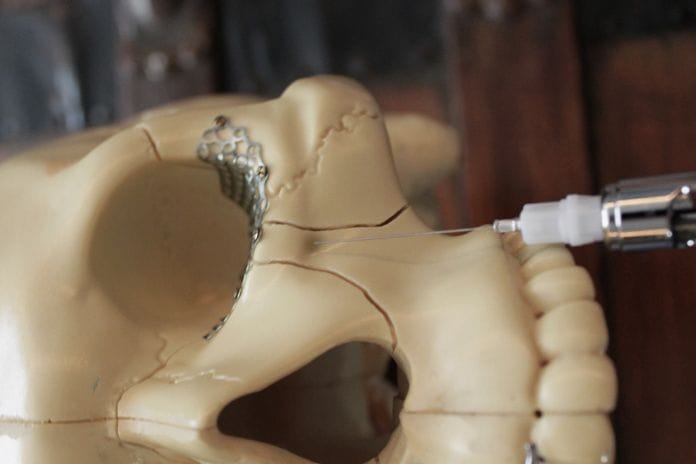
Now that this important concern is cleared up let’s examine the steps of giving this injection. First, palpate the bony infraorbital ridge below the patient’s eye. You will feel it sink in slightly in the infraorbital notch. Right below that notch, there is a slight depression in the skin. This is the infraorbital foramen, and our target when depositing the anesthetic. If you ask the patient, they will report a slight tingling/discomfort when the area is pressed. Note, I do not ask my patients if it hurts them while poking around under their eye. I used this tip to practice on myself and my friends until I was confident I could locate the foramen. When getting ready to inject, you can keep your finger on the foramen as you retract the tissue with your non-dominant hand. This helps you visualize the target as the needle advances and makes it easy to apply pressure to the location after you deposit.
Injection Site
Malamed states the ASA injection site is the mesiobuccal fold above the first premolar, as this is the landmark that provides the shortest path through the tissue to the IO foramen. Intraorally, this injection will look quite similar to the MSA, just one tooth forward. Sometimes the buccal frenum will be in the way, and in that case, I choose an injection site anterior to it. Any site between the first premolar and central incisor will work as long as the anesthetic is deposited into the foramen.
Needle and Volume
A long needle is generally recommended, although for children and adults with petite facial structure, a short needle may be used. This injection has a landmark that can be located extraorally, so if you are unsure of the depth needed, you can locate the IO foramen and view its distance from the injection site to determine the needle length needed.
The depth is 16mm on average or half the length of the long needle. Hygienists are better than most at estimating length in millimeters, but most of us do not work with 16mm pockets (thank goodness!), which is why I find the half needle guideline to be most practically useful.
After insertion, keep the needle parallel with the long axis of the tooth and gently contact bone. This will be the upper rim of the infraorbital foramen. Aspirate and deposit .9 to 1.2mL. After slowly depositing, withdraw the needle, safely recap, and apply gentle pressure extraorally over the site of the IO foramen for 1-2 minutes.
Malamed states you can apply pressure during deposition of the anesthetic as well. The pressure pushes the anesthetic through the foramen and allows the ASA nerve to be anesthetized. It also greatly reduces the risk of a hematoma. The IO nerve will be blocked fairly quickly, but keep in mind it will take a little longer for the teeth to be profoundly numb from the ASA. This is not like the IA injection, where we know we are ready to proceed with treatment when the lip is numb. It’s best to touch the buccal gingiva of the affected area with an explorer to determine if the patient is profoundly anesthetized.
Considerations
As with other injections for teeth near the midline, there is a chance the patient has crossover innervation from the other side and will require an additional infiltration.
Lack of pressure over the foramen following the injection can lead to anesthesia of the lips, lower eyelid and side of the nose without blocking the ASA nerve, leading to the need for additional injections. Some patients may be alarmed if they are not told to expect these areas of soft tissue to be anesthetized. Most people are unconcerned when they know in advance what to expect, and that their face will feel normal after the anesthetic wears off.
Finally, this injection is similar to the IA in the sense it provides anesthetic right at the foramen and does not provide localized hemostasis from epinephrine. Often this is not a concern, but if the patient has bleeding which is difficult to control, localized injections can deliver epinephrine to constrict the blood vessels and help with the bleeding. I have not noticed an issue using the ASA for my SRPs, but it is something to be aware of, especially when anesthetizing for anterior composites with erythematous tissue nearby.
Conclusion
While the above should be taken into consideration, the ASA injection is a safe, simple anesthesia option that minimizes the number of injections and the volume of anesthetic deposited. The landmarks are easy for the clinician to locate, and the injection is comfortable for the patient. Reducing the volume of anesthetic is particularly useful for children, people with heart conditions, or any other patient that needs limited cartridges of local anesthetic. The ASA is a great option to increase our patients’ comfort and safety. Everyone is a fan of fewer shots!
Need CE? Click Here to Check Out the Self-Study CE Courses from Today’s RDH!
Listen to the Today’s RDH Dental Hygiene Podcast Below:
References
Malamed, S. F. (2013). Techniques of Maxillary Anesthesia. Handbook of Local Anesthesia. 6th ed., pp. 197-200. St. Louis, MO: Mosby.