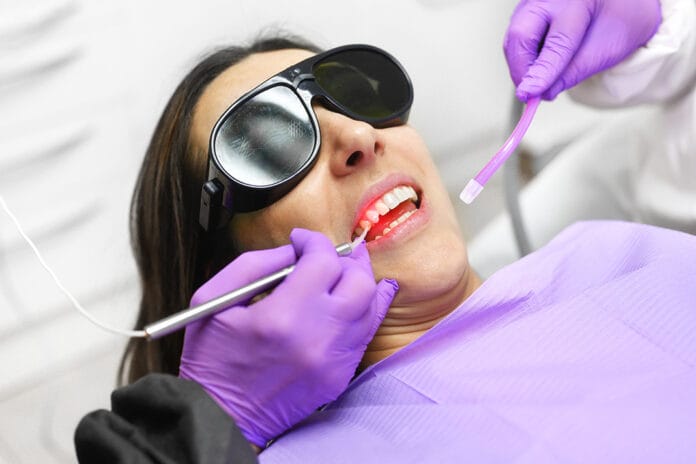
March 2020 has forever changed our world as well as the way we treat patients in the dental setting. Adhering to strict Center for Disease Control and Prevention (CDC) guidelines to ensure the safety and health of our patients, ourselves, and co-workers have been the standard of care since AIDS surfaced in the 1980s.
The onset of COVID-19 has required an upgrade to our personal protective equipment (PPE) and standard of care. Prevention of person-to-person transmission of COVID-19 and any other unknowns are at the summit of our priorities as we care for our patients.
Besides the updated CDC recommended PPE, we must think beyond the standard of care and consider enhanced options for our patients’ overall oral and systemic health. Pre-procedural rinses are given to patients to reduce the pathogen count in the oral cavity, which inadvertently also reduces aerosol contaminants. Why wouldn’t we also pre-treat the very sulcus that we navigate with our instruments?
Laser-assisted Hygiene
Diode lasers can be used as an adjunct to hygiene maintenance and therapeutic procedures by assisting in the bacterial reduction of the sulcus, decontamination of diseased tissue, potential biostimulation of osteoblasts, collagen fibers and fibroblasts, and prevention of bacteremia.1-5 Diode lasers can reduce dentin hypersensitivity, as well as promote healing of cold sores and aphthous ulcers.6-8
There are numerous benefits and ways diode lasers can be used in the dental setting. In this article, though, we will focus on the decontamination properties of the laser and how the laser can be utilized in dental hygiene. This article aims to stimulate curiosity and interest in laser-assisted hygiene therapy and encourage laser training to enable a successful laser program for your hygiene department.
Laser Bacterial Reduction
Diode lasers are low-level lasers that are attracted to dark pigmentation. Sweeping the laser just below the gingival margin (.5-1mm) at an interval of five to 10 seconds per side (buccal and lingual) of each tooth can reduce subgingival bacteria by the billions. It is painless and only takes four to five minutes to complete.
This procedure is called laser bacterial reduction (LBR), and most patients are thrilled to know we can decontaminate microbes below their gingiva.
The benefits of LBR include:
- Prevention of bacteremia
- Reduced microbes in aerosols (as a result of decontaminated pockets)
- Kills periodontal pathogens
- Healthier gingiva
- Reduced inflammation
- May induce biostimulation of bone and tissue (osteoblasts and fibroblasts)
- Painless, quick, and easy
Gaining Confidence with Lasers
Approximately eight years ago, I completed my first laser certification at an eight-hour continuing education seminar. Half of the day was study and half of the day was clinical (learning proper laser technique on a pig jaw). It was a good introduction to laser therapy, but I did not gain the confidence required to fully incorporate the diode laser into our practice on a consistent basis. It did, however, give me my training wheels to ease into this “new era” of laser-assisted dentistry.
A few years later, I went through another diode laser training and certification. This time I dusted off our diode laser and carted it with me for hands-on training. With this training, I developed the confidence of proper laser technique but still lacked the know-how of patient education, chairside introduction, and laser discussion.
Not knowing the proper verbiage to use made promoting laser therapy rather difficult. As a result, I used my laser only on occasional periodontal cases, not using it to its fullest potential ─ definitely not getting our money’s worth from the laser and training.
I paired up with Joy Raskie at Advanced Dental Hygiene (ADH) last year and went through the most fruitful diode laser training of them all! The most important process of this ADH training was learning the right verbiage for talking with patients about diode laser therapy and how it is such a positive attribute to their oral health as well as their systemic health. Joy’s excitement for laser therapy, paired with her method of training, is contagious and inspiring. Reminding patients that the immune system starts with the mouth is a real eye-opener for most. Most are thankful and glad to be offered laser bacterial reduction prior to any instrumentation as protection from systemic bacteremia while gaining a healthier mouth.
Since most insurance companies do not cover laser therapy, simply present the LBR option to your patients, pause, and allow them time to inquire further. Let them ask the insurance and pricing questions. Advise them of your fee and that it is not usually an insurance-covered benefit. Do not be afraid to offer it to patients whom you may not expect will say yes. On average, I have discovered that eight out of 10 patients want this therapy and are willing to pay the out-of-pocket expense for health. By not offering each patient the same opportunity to have laser-assisted hygiene therapy, you are actually saying no for them.
The diode laser has many other beneficial options that we need to be aware of, such as:
Laser decontamination (LD) ─ Think of LBR as the pre-treatment. LBR kills periodontal pathogens in the pockets prior to instrumentation. In contrast, LD kills the periodontal pathogens embedded in the tissue and is done after nonsurgical periodontal therapy (D4341/D4342) or scaling in the presence of inflammation (D4346). Since the laser is attracted to dark pigmentation, which inflamed and necrotic tissue is, the laser tip removes necrotic and diseased tissue.
The technique is integral and is taught through proper laser training that includes hands-on training. While LBR focuses on the diode laser in the pocket parallel to the long axis of the root, LD is slightly focused toward necrotic tissue with an initiated tip. Proper settings, technique, and methods are taught in great detail during required laser training. While I have been to numerous laser courses, I found the most thorough and easy to understand was Joy Raskie’s Advanced Dental Hygiene program.
Laser decontamination (LD) is used to treat those areas of significant inflammation and diseased tissue by killing the pathogens in the tissue and actually removing the necrotic/degranulation tissue from the sulcus so new and healthy tissue is stimulated.
Lesions (herpes lesions and aphthous ulcers) ─ Isn’t it frustrating when your patient arrives, is seated in the chair, and you discover they are afflicted with an active labial herpes lesion? Most patients are not aware that we should not treat them when they have an active cold sore, and many employers do not want that patient to leave without a hygiene therapy appointment.9
Frustration surfaces when we have to reluctantly reschedule their therapy appointment ─ several weeks or months down the road. What if we could quickly and easily treat that herpetic lesion and instantly send it into healing mode? The patient gets their sore safely treated, they are rescheduled for their hygiene therapy appointment, and everyone is left with a happy “win-win” scenario! Advise your patient that you can help prompt a cold sore into healing mode even sooner if they come in as soon as they feel the “tingling” onset. More good news for the patient who suffers from herpetic outbreaks is that it most likely will not recur in that same spot again. Bonus!
The same type of treatment can be used to comfort a painful aphthous ulcer. Some patients are prone to getting multiple aphthous ulcers at a time, especially during the fresh garden tomato season! Casually inform patients about all of the potential benefits of laser therapy while doing their LBR. It’s a good time for small talk and educational chat regarding the diode laser.
Treating oral lesions such as herpes lesions and aphthous ulcers takes approximately two minutes. It involves sweeping an uninitiated tip in a circular motion approximately 3 mm from the lesion (starting at 6-8mm and slowly moving toward the lesion in a circular motion) for 30 seconds in three to four intervals, starting 1-2mm outside of lesion border and working inside. It is important to ask the patient if they feel any tingling and/or numbing every 15 seconds or so. This helps gauge that you are using the proper setting. Exact detail, laser mode, and technique are taught in laser training with a certified instructor.
Dentinal desensitizing ─ Dentinal hypersensitivity can turn a dental appointment into a traumatic experience for both patient and practitioner. This scenario can lead to canceled or missed appointments as patients do not look forward to “being poked” by the hygienist. Dentinal exposures can also make eating and drinking certain foods at certain temperatures quite painful.
Treating sensitive root surfaces quickly and easily with a diode laser will make friends out of the most anxious patient. The technique is very similar to lesion treatment and is learned with hands-on training with a certified instructor. As the laser slows down the fluid in the dentinal tubules by making it more viscous (coagulates the protein), thus preventing the tidal wave effect of fluids abruptly slamming into the nerves causing the immediate sensation of pain.10 Patients will appreciate your care, concern, and “magical pain reduction abilities” as their dental anxieties and dentinal hypersensitivities lessen with each visit.
An Aid to a Healthier Immune System
We are blessed to have the assistance of social media and television educating our patients on the correlation between mouth health and whole-body health. This oral-systemic link needs to be a routine conversation during dental health checkups.
Did you know that the average medical doctor only gets one hour of oral training during medical school? This is because they consider the dentist to be the “physicians of the mouth.” Use your health history as an educational tool. It will set up the backdrop discussion regarding the importance of laser bacterial reduction therapy as an aid to a healthier immune system.
So, if your office is considering purchasing a laser, I highly recommend searching out a training company that not only teaches you the basics of lasers but also dives deep into verbalization and hands-on training so you can feel confident in talking about laser therapy as well as delivering laser therapy to all your patients. I found great success with Advanced Dental Hygiene and can tell you, it was time and money well spent. Your patients will thank you for caring and will appreciate having the latest technology to help protect against microbial pathogens.
After all, a strong immune system starts with a healthy mouth. Let’s strive to integrate diode lasers into the hygiene operatories as a new standard of care.
Need CE? Click Here to Check Out the Self-Study CE Courses from Today’s RDH!
Listen to the Today’s RDH Dental Hygiene Podcast Below:
References
- Kreisler, M., Haj, H., D’Hoedt, B. Clinical Efficacy of Semiconductor Laser Application as an Adjunct to Conventional Scaling and Root Planing. Lasers Surg Med. 2005; 37(5): 350-355. https://pubmed.ncbi.nlm.nih.gov/16365890/
- Fontana, C.R., Kurachi, C., Mendonca, C.R., et al. Microbial Reduction in Periodontal Pockets under Exposition of a Medium Power Diode Laser: An Experimental Study in Rats. Lasers Surg Med. 2004; 35: 263-268. https://pubmed.ncbi.nlm.nih.gov/15493030/
- Moritz, A., Schoop, U., Goharkhay, K., et al. Treatment of Periodontal Pockets with a Diode Laser. Lasers Surg Med. 1998; 22: 302-311. https://pubmed.ncbi.nlm.nih.gov/9671997/
- Kreisler, M., Christoffers, A.B., Willershausen, B., et al. Effect of Low-level GaA/As Laser Irradiation on the Proliferation Rate of Human Periodontal Ligament Fibroblasts: An in vitro Study. J Clin Periodontal. 2003; 30: 353-358. https://pubmed.ncbi.nlm.nih.gov/12694435/
- Assaf, M., Yilmaz, S., Kuru, B., et al. Effect of the Diode Laser on Bacteremia Associated with Dental Ultrasonic Scaling: A Clinical and Microbiological Ttudy. Photomed Laser Surg. 2007 Aug; 25(4): 250-6. doi: 10.1089/pho.2006.2067. PMID: 17803380. https://doi.org/10.1089/pho.2006.2067.
- Brugnera, A., Zanin, F., Ladaladro, T.C., Pinheiro, A., Pecora, J.D. (2006, February 28). LLLT in Treating Dentinary Hypersensitivity: New Concepts, Proc. SPIE 6140. Mechanisms for Low-Light Therapy. Retrieved from https://www.spiedigitallibrary.org/conference-proceedings-of-spie/6140.toc
- Bello-Silva, M.S., Moreira de Freitas, P., Corrêa Aranha, AC, et al. Low- and High-intensity Lasers in the Treatment of Herpes Simplex Virus 1 Infection. Photomedicine and Laser Surgery. 2010; 28(10): 135-139. Retrieved from http://doi.org/10.1089/pho.2008.2458
- Babu, B., Uppada, U.K., Tarakji, B., et al. Versatility of Diode Lasers in Low-level Laser Therapy for the Management of Recurrent Aphthous Stomatitis. J Orofac Sci. 2015; 7: 49-53. Retrieved from https://www.jofs.in/text.asp?2015/7/1/49/157392
- Kohn, W.G., Collins, A.S., Cleveland, J.L., Harte, J.A., Eklunt, K.J., Malvitz, D.M. Center for Disease Control and Prevention. Guidelines for Infection Control in Dental Health-Care Settings – 2003. MMWR 2003; 52 (Report No. 17). Retrieved from http://www.cdc.gov/mmwr/PDF/rr/rr5217.pdf
- Asnaashari M, Moeini M. Effectiveness of Lasers in the Treatment of Dentin Hypersensitivity. J Lasers Med Sci. 2013; 4(1): 1-7. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4281970/