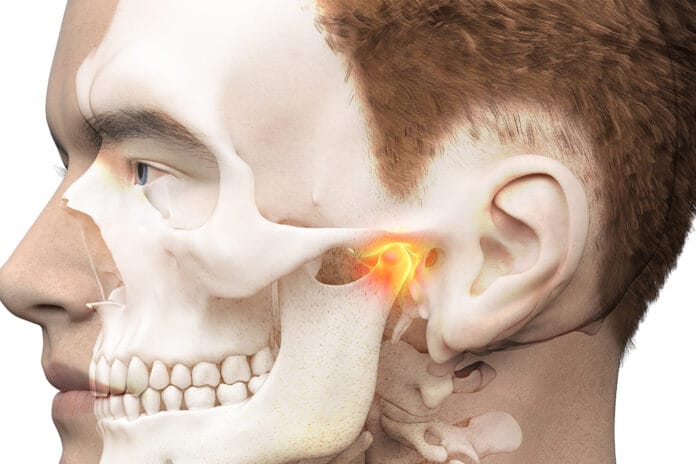
The temporomandibular joint (TMJ) examination is part of routine screening not only for dentists but also for dental hygienists. During our extraoral exam, we palpate the joint, try to detect the movements of condyles during opening and closing, see if it’s deviating to one side or the other, and try to feel for any crepitus, popping, or clicking.
We ask dental patients if they feel any pain or tenderness in the joint or the muscles around the joint. We are required to document all these findings. Based on these findings, the doctor can recommend orthodontics to treat malocclusion or arrest parafunctional habits like bruxism by recommending a nightguard.
Hygienists are trained to focus on the mouth and what is happening inside it. Sometimes we forget that the temporomandibular joint is a neighbor to many other organs and structures on the face, and any change in TMJ function might affect these neighbors. On the lateral end of the joint socket, we have the ear apparatus, medially we have the airway, and superiorly we have air sinuses.
Dental hygienists can observe the TMJ beyond occlusal issues, and can hopefully help guide patients with any discomfort they may have had for a long time without knowing its origin. Following are a few conditions that we can discuss with them.
Connection to Female Hormones
Temporomandibular disorder (TMD) is a condition that is loosely characterized by pain and dysfunction of the masticatory system. The dental patient has pain in masticatory muscles, TMJ, and associated hard and soft tissues.1
A large majority of patients treated for TMD are women. Literature suggests the disorder is 1.5 to 2.0 times more prevalent in women, especially in ages 20 to 40, while males had a more uniform age distribution.1,2 Female patients also show greater tenderness and pain as compared to males.2 The age and gender distribution related to the severity of TMD indicates a hormonal link to female hormones.1 Extensive research needs to be done to pinpoint the exact role that the hormone cycle might play in the severity of TMD.
As hygienists, we can inform patients that simply being of the female gender and in the age of 20 to 40 increases their chances of having TMD. Keeping track of the monthly cycle can help pinpoint when the condition is more severe. Taking NSAIDs and physiotherapy like deep massage, hot/cold compressions, or acupressure may help temporarily reduce TMD symptoms.3
Headache
A patient might complain of suffering from frequent headaches during a hygiene appointment. By asking about the history of headaches and doing an extraoral, TMJ, and occlusal exam, a hygienist might get some idea if the headaches have TMJ origins or not. There is a positive correlation between headaches, myofascial pain, and TMD. By palpating the myofascial trigger points (MTrP), the exaggeration of pain can confirm that the headaches have an MTrP origin.
Headaches appear more frequently in patients suffering from TMD as compared to people without TMD (27.4% vs. 15.2%). The headaches can either be migraines which consist of aura, unilateral throbbing, and pain of varying intensity along with sensitivity to the light and sound, nausea, neck stiffness, and fatigue, or tension headaches that are bilateral nonthrobbing with mild pain.3
The International Classification of Headache Disorders recommends establishing a relationship between TMD and headaches regarding onset, development, and improvement. Headaches attributed to TMD (HTMD) can be managed in different ways. Some options that can be discussed with a patient are splints that stabilize temporal and occlusal relationships, psychological therapy such as cognitive behavior therapy, physical therapy, deep massage, electrical or laser stimulation, moist heat, active relaxation therapy, and medications including NSAIDs, steroids, muscle relaxants, and antiepileptic drugs. Improvement of parafunctional habits like abnormal tooth contact can also help in the improvement of headaches.3
Meniere’s Disease
Many TMD patients might suffer from otologic symptoms such as fullness of the ear, otalgia, loss of hearing, vertigo, and tinnitus. All these symptoms are also present in Meniere’s disease, which is a disease of the inner ear and has idiopathic origins. Although no relationship has been established between Meniere’s disease and TMD, research has shown that treatment of TMD with an orthotic device helps reduce the otologic symptoms associated with Meniere’s disease.4
By asking a patient whether they have ringing in the ears or any other otologic symptoms, a hygienist can educate the patient and guide them towards treatment options for not only the TMD but also Meniere’s disease. A referral may be necessary to an appropriate health care provider such as an ear, nose, and throat (ENT) specialist, audiologist, or neurologist.
Obstructive Sleep Apnea Hypopnea Syndrome
Obstructive sleep apnea hypopnea syndrome (OSAHS) is a sleep disorder characterized by intermittent upper airway collapse resulting in oxygen desaturation and sleep fragmentation. Pharyngeal anatomy, nasal issues, lung capacity, and dilator muscle anatomy are all contributing factors to OSAHS.5 For a definitive diagnosis, a sleep study is recommended and can establish if OSAHS is present.
Continuous Positive Airway Pressure (CPAP) was the device of choice for patients suffering from sleep apnea, but intolerance and noncompliance reduced its effectiveness. In recent years, oral appliances have been developed for OSAHS patients showing positive results. Mandibular Advancement Device (MAD) is an intraoral device that prevents the collapse of the airway by altering the position of the jaw and tongue by protruding the mandible forward. MAD has been shown to increase airway space.5
Asking patients about their sleep, snoring, and fatigue might indicate some connection between mandibular joint position and sleep apnea, and the patient can be guided towards proper treatment. This, in turn, will positively affect a patient’s quality of life.
As diagnostic tests and exams become more refined, more connections between oral conditions and systemic conditions are being found. Chronic systemic conditions in patients can be helped with as little as correction of condyles inside the socket or fixing the bite. These minor changes might improve the quality of our patient’s life and make our work even more rewarding.
Before you leave, check out the Today’s RDH self-study CE courses. All courses are peer-reviewed and non-sponsored to focus solely on high-quality education. Click here now.
Listen to the Today’s RDH Dental Hygiene Podcast Below:
References
- Warren, M.P., Fried, J.L. Temporomandibular Disorders and Hormones in Women. Cells, Tissues, Organs. 2001; 169(3): 187-192.
- Schmid-Schwap, M., Bristela, M., Kundi, M., Piehslinger, E. Sex-specific Differences in Patients with Temporomandibular Disorders. Journal of Orofacial Pain. 2013; 27(1): 42-50. https://doi.org/10.11607/jop.970
- Abouelhuda, A.M., Kim, H.S., Kim, S.Y., Kim, Y.K. Association Between Headache and Temporomandibular Disorder. Journal of the Korean Association of Oral and Maxillofacial Surgeons. 2017; 43(6): 363-367. https://doi.org/10.5125/jkaoms.2017.43.6.363
- Monzani, D., Baraldi, C., Apa, E., et al. Occlusal Splint Therapy in Patients with Ménière’s Disease and Temporomandibular Joint Disorder. ACTA Otorhinolaryngologica Italica. 2022; 42(1): 89-96. https://doi.org/10.14639/0392-100X-N1641
- Basyuni, S., Barabas, M., Quinnell, T. An Update on Mandibular Advancement Devices for the Treatment of Obstructive Sleep Apnoea Hypopnoea Syndrome. Journal of Thoracic Disease. 2018; 10(Suppl 1): S48-S56. https://doi.org/10.21037/jtd.2017.12.18