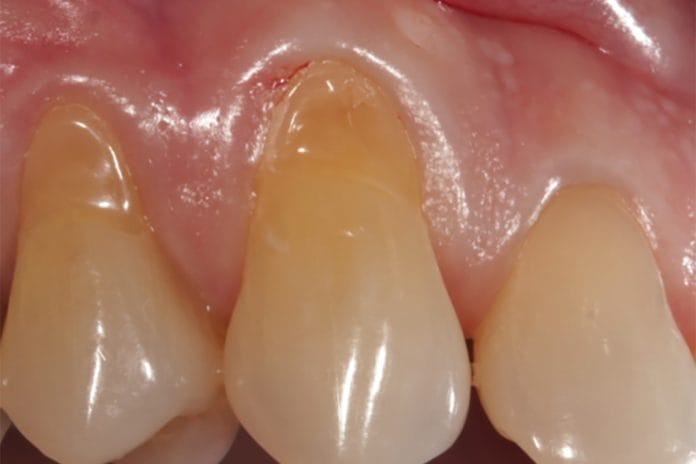
Gingival recession is something most of us see in our patients’ on a daily basis. It is defined as the apical migration of gingiva, which can cause various problems for our patients, including sensitivity, periodontal complications, esthetic concerns, and decay.1 Gingival recession results from many different factors, such as patient habits (i.e., picking with their fingernails), periodontal disease, bruxism, and orthodontic treatment.
Dental hygienists can educate patients on how best to prevent recession. Fortunately, surgical options are also available when patient education techniques aren’t enough.
The three most common types of surgical soft tissue grafting are the subepithelial connective tissue graft, free gingival graft, and the allograft. The first two mentioned are considered autografts because they are taken from the patient’s own mouth, while the third mentioned is an allograft because the tissue used comes from a donor.
Surgical Grafting
Subepithelial connective tissue grafts use the underlying layer of tissue (the epithelium). For this surgical procedure, tissue is most commonly taken from the patient’s palate. An incision is made in order to access the underlying layer of epithelial connective tissue, and a portion is removed. This portion is then transplanted to the site of recession and sutured into place. The superficial keratinized layer on the palate is also closed with sutures.
This type of graft can be used in areas that lack keratinized tissue and sites that may be of aesthetic importance. The patient may be provided with a stent or a bandage to protect the palate during the initial phase of healing. According to one study, “Subepithelial connective tissue graft procedures provide the best root coverage due to the availability of keratinized tissue compared to the other types of grafting.”2
The second type of autograft is the free gingival graft; this graft is similar to the first but differs in the fact that the tissue taken from the donor site of the patient includes the top portion of keratinized tissue as well as the underlying layer of epithelium. This type of graft can be used in areas similar to the subepithelial connective tissue graft but may not be the best option for areas that are of aesthetic concern because the tissue taken can be thicker and bulkier in appearance and not match the surrounding tissue color.1,3
The third type of graft is the allograft, which uses cadaver tissue instead of the patient’s own for the surgical procedure. This may be a good option for patients who have so many areas of recession that enough tissue could not be harvested from the patient. It may also be indicated for patients who have severe dental/surgical anxiety and are not comfortable with the other two types of procedures. A large benefit from this type of procedure is that the patient only has one surgical site. One study compared allografts and free gingival grafts and concluded that “there was an excellent blending of color and texture,” and their free gingival graft counterparts had slightly less color matching as well as visible borders where the free gingival graft started and stopped.3
Esthetic Considerations
Soft tissue grafting can also be used to address esthetic concerns for implants. One study concluded that “augmentation using a connective tissue graft may result in better mucosal color match and more facial dimensional gain compared to implant sites without soft tissue grafting.” This may be especially true for anterior implants where esthetics are of a very high concern.4
I find it easiest to evaluate and document patients for recession at the same time I check probe depths. Whenever you take your patients’ assessments, you can then discuss any areas of recession you may have found and the different treatment options that are associated with it. Using an intraoral camera to show patients the recession may help them gain a better understanding of the importance of treating it.
Evaluating their habits is helpful if you notice a patient has generalized recession, ask what type of toothbrush they’re using at home, and even have them show you how they brush. I find my patients who use electric toothbrushes don’t comprehend that the toothbrush does all of the work for them, so they don’t need to aggressively brush. So many electric toothbrushes come with pressure sensors as well, which is helpful.
If you see signs of wear on the teeth or the patient reports sore jaw muscles and joints, they may be clenching and/or grinding and may be in need of an appliance or referral to an orthodontist, sleep specialist, and/or myofunctional therapist.
A localized area of recession may indicate a localized periodontal problem or other pathology that may warrant additional diagnostics like imaging.
As it pertains to the surgical treatments for gingival recession, if you do not provide these services in your office, referring your patient to a periodontist or oral surgeon for an evaluation may be warranted.
Before you leave, check out the Today’s RDH self-study CE courses. All courses are peer-reviewed and non-sponsored to focus solely on high-quality education. Click here now.
Listen to the Today’s RDH Dental Hygiene Podcast Below:
References
- Shah, R., Thomas, R.S., Mehta, D.S. Recent Modifications of Free Gingival Graft: A Case Series. Contemp Clin Dent. 2015; 6(3): 425-427. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4550001/
- Tatakis, D.N., Chambrone, L., Allen, E.P., et al. Periodontal Soft Tissue Root Coverage Procedures: A Consensus Report from the AAP Regeneration Workshop. J Periodontol. 2015; 86(2 Suppl): S52-55. https://www.ncbi.nlm.nih.gov/pubmed/25315018
- Agarwal, C., Tarun Kumar, A.B., Mehta, D.S. Comparative Evaluation of Free Gingival Graft and AlloDerm(®) in Enhancing the Width of Attached Gingival: A Clinical Study. Contemporary Clinical Dentistry. 2015; 6(4): 483-488. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4678545/
- Hosseini, M., Worsaae, N., Gotfredsen, K. Tissue Changes at Implant Sites in the Anterior Maxilla With and Without Connective Tissue Grafting: A Five-year Prospective Study. Clin Oral Implants Res. 2020; 31(1): 18-28. https://www.ncbi.nlm.nih.gov/pubmed/31529645