When working clinically, a common question I receive is: “Will my wisdom teeth make my teeth crowded?” Many discussions in dental hygiene forums end with little consensus.
Many studies have investigated the possible link. But is it really that simple? Can one single entity be the cause of mandibular anterior crowding?
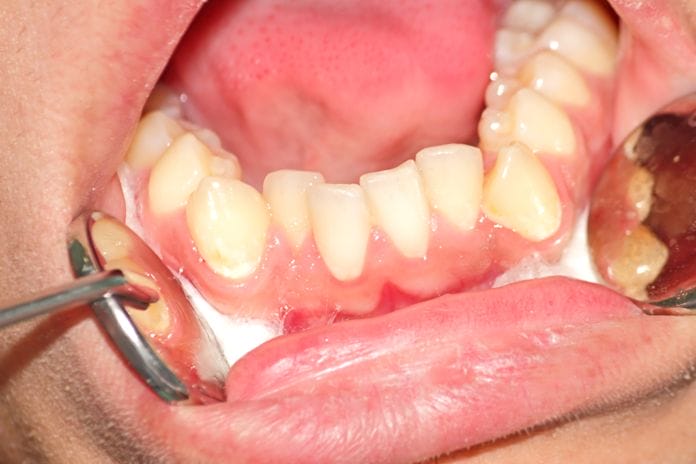
I have found that mandibular anterior crowding is one of the most common concerns among patients as they age. Mandibular anterior crowding has been observed in patients with previous orthodontic treatment as well as those with no previous orthodontic treatment.
The primary scapegoat for anterior crowding seems to be third molars. This seems to be the case because mandibular anterior crowding is observed around the time the third molars are erupting. This event causes many clinicians and patients to assume a cause-and-effect relationship between the two events. However, it is important to remember correlation does not equal causation.
Lifelong Dimensional Changes
A systematic review published in The Scientific World Journal reviewed studies that included patients with impacted, erupted, extracted, or congenitally missing third molars. Some of the studies reviewed were longitudinal, and others were cross-sectional; there was no difference between the different groups.1 This indicates that third molars are not the culprit of mandibular anterior crowding. Additionally, there are other studies that have concluded the same.2,3,4
If we rely on the science, we can dismiss the idea that third molars are the etiology of mandibular anterior crowding. Other studies have postulated the possibility of changes in the mandible that affect the arch dimensions. Some studies suggest the changes are due to post-orthodontic instability, which is reasonable, but what about people who have never had orthodontic treatment? Are there indications that these individuals have the same changes in their arch dimensions?
The short answer is yes, patients who have never had orthodontic treatment also show dimensional changes throughout life. One study evaluating patients without previous orthodontic treatment showed a reduction of inter-canine width and a decrease in mandibular arch length throughout life with the changes becoming milder after the second decade of life.5
40 Years of Changes
Another longitudinal study that followed patients over a 40-year time span documented changes in overjet, overbite, arch length, inter-canine width, inter-molar width, arch depth, and irregularity index. Their findings confirmed that there are physiological changes to both dental arches throughout life. Details of the findings are as follows:
- Changes in overjet were insignificant, although a minor decrease in overjet was reported at around 0.14mm.
- No significant change in overbite was found in the subjects of this study, although previous studies have indicated an increase in an overbite.
- A significant decrease in arch length was observed in both the mandible and the maxilla. A decrease in arch length contributes to a gradual anterior migration of the teeth. Mesial drift of the first molar appears to be instrumental in the decrease in arch length. This migration may be caused by changes in intrinsic forces from the tongue and lips as we age.
- Inter-canine width significantly decreased as well more so on the mandible. This, too, can be attributed to mesial drift of the first molars.
- Inter-molar width increased on both arches, with the increase in the maxilla being more pronounced.
- Arch depth decreased in both arches, again this is attributed to mesial drift of the first molars. Little’s irregularity index, an index used in orthodontics to measure mandibular anterior crowding, increased significantly only in the mandibular arch. You can view an example of the measurements used in Little’s irregularity index 6
These studies indicate that we are all susceptible to mandibular anterior crowding. One study even classifies it as “natural,” comparing it to male baldness. This study dives deep into the tensegrity of the dental arch and alludes to external and internal forces breaking down the stability leading to crowding.7 This supports the previous studies hypothesis of changes in intrinsic forces of the lips and tongue as a contributing factor.
Impact of Overcrowding
For patients who have had orthodontic treatment, encouraging them to keep their permanent lingual retainer may be the best preventive measure we can offer to reduce the risk of anterior crowding. A longitudinal study following patients 12 years post orthodontic treatment found “after retention (at least 10 years after removal of all retainer devices), more than 70% were classified as showing moderate to severe crowding.”8
Cosmetic concerns are not the only issue with anterior crowding. A recently published longitudinal study shows anterior crowding is a risk factor in periodontal disease progression. This is an important aspect of anterior crowding that dental professionals should discuss with their patients. Additionally, for patients that prefer to forgo orthodontic treatment, closely monitoring the periodontal health of patients with anterior crowding is warranted.9
Mandibular anterior crowding is not a dental issue that is going away anytime soon. A better understanding of the etiology can help dental professionals better educate their patients. Changes in forces and mesial drift appear to be the main etiological factors currently.
Beyond orthodontic treatment, there doesn’t appear to be many options for correcting anterior crowding. More importantly, it appears anyone with a relatively full complement of teeth is at risk of becoming a victim of anterior crowding. The next time a patient voices concerns about anterior crowding, I hope this knowledge and science supporting it will help you confidently explain the etiological factors associated with anterior crowding and dispel misinformation.
Now Listen to the Today’s RDH Dental Hygiene Podcast Below:
References
- Zawawi, K.H., Melis, M. The role of mandibular third molars on lower anterior teeth crowding and relapse after orthodontic treatment: a systematic review. Scientific World Journal. 2014; 2014: 615429. doi:10.1155/2014/615429. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4032723/
- Al-Balkhi, K.M. The effect of different lower third molar conditions on the re-crowding of lower anterior teeth in the absence of tight interproximal contacts one-year post orthodontic treatment: a pilot study. J Contemp Dent Pract. 2004; 5(3): 66–73. Retrieved from https://pubmed.ncbi.nlm.nih.gov/15318258-the-effect-of-different-lower-third-molar-conditions-on-the-re-crowding-of-lower-anterior-teeth-in-the-absence-of-tight-interproximal-contacts-one-year-post-orthodontic-treatment-a-pilot-study/
- Sidlauskas, A., Trakiniene, G. Effect of the lower third molars on the lower dental arch crowding. Stomatologija. 2006; 8(3): 80–84. Retrieved from https://pubmed.ncbi.nlm.nih.gov/17191063-effect-of-the-lower-third-molars-on-the-lower-dental-arch-crowding/
- Genest-Beucher, S., Graillon, N., Bruneau, S., Benzaquen, M., Guyot, L. Does mandibular third molar have an impact on dental mandibular anterior crowding? A literature review. J Stomatol Oral Maxillofac Surg. 2018; 119(3): 204–207. doi:10.1016/j.jormas.2018.03.005. Retrieved from https://pubmed.ncbi.nlm.nih.gov/29571816-does-mandibular-third-molar-have-an-impact-on-dental-mandibular-anterior-crowding-a-literature-review/
- Mauad, B.A., Silva, R.C., Aragón, M.L., Pontes, L.F., Silva Júnior, N.G., Normando, D. Changes in lower dental arch dimensions and tooth alignment in young adults without orthodontic treatment. Dental Press J Orthod. 2015; 20(3): 64–68. doi:10.1590/2176-9451.20.3.064-068.oar. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4520140/
- Tsiopas, N., Nilner, M., Bondemark, L., Bjerklin, K. A 40 years follow-up of dental arch dimensions and incisor irregularity in adults. Eur J Orthod. 2013; 35(2): 230–235. doi:10.1093/ejo/cjr121. Retrieved from https://pubmed.ncbi.nlm.nih.gov/22015823-a-40-years-follow-up-of-dental-arch-dimensions-and-incisor-irregularity-in-adults/?from_single_result=A+40+years+follow-up+of+dental+arch+dimensions+and+incisor+irregularity+in+adults
- Consolaro, A., Cardoso, M.A. Mandibular anterior crowding: normal or pathological? Dental Press J Orthod. 2018; 23(2): 30–36. doi:10.1590/2177-6709.23.2.030-036.oin. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6018449/
- Schütz-Fransson, U., Lindsten, R., Bjerklin, K., Bondemark, L. Twelve-year follow-up of mandibular incisor stability: Comparison between two bonded lingual orthodontic retainers. Angle Orthod. 2017; 87(2): 200–208. doi:10.2319/031716-227.1. Retrieved from https://www.researchgate.net/publication/306434672_Twelve-year_follow-up_of_mandibular_incisor_stability_Comparison_between_two_bonded_lingual_orthodontic_retainers
- Alsulaiman, A.A., Kaye, E., Jones, J., et al. Incisor malalignment and the risk of periodontal disease progression. Am J Orthod Dentofacial Orthop. 2018; 153(4): 512–522. doi:10.1016/j.ajodo.2017.08.015. Retrieved from https://pubmed.ncbi.nlm.nih.gov/29602343-incisor-malalignment-and-the-risk-of-periodontal-disease-progression/