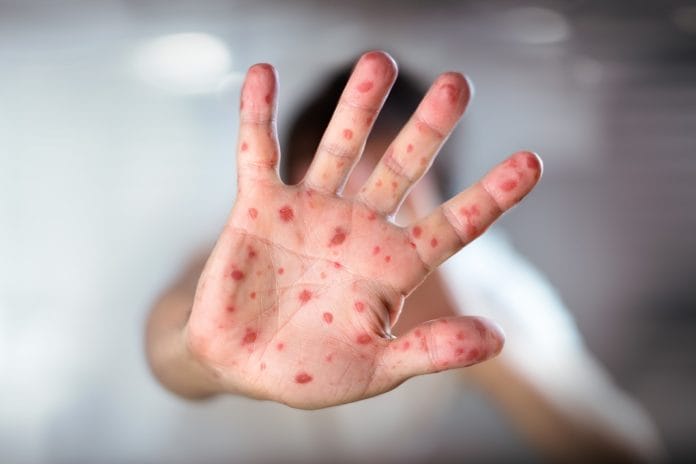
We may see a record-breaking number of measles cases in the United States for the first time this year, the highest since the elimination of measles in the year 2000. From January 1 through April 19, there have been 626 individual cases of measles confirmed in 22 states.
I would like to emphasize these are confirmed cases; there could be more unconfirmed cases.1 The concern surrounding this recent outbreak can be better understood by considering the basic reproduction number or R0 (pronounced R-not). The basic reproduction number for measles is 12 to 18. This means each person with measles, on average, would infect 12-18 other people in a totally susceptible population.2
The good news is that here in the United States we do not live in a totally susceptible population. However, measles is considered one of the most highly contagious viruses that lives in the nose and throat of infected individuals. The virus can live in an airspace for up to two hours where an infected person coughed or sneezed. In addition, “Infected people can spread measles to others from four days before through four days after the rash appears,” according to the Centers for Disease Control and Prevention.3
A Spot We Can’t Miss
As dental professionals, do we play a role in this outbreak? The answer is yes. The measles has two phases: a prodromal stage and an exanthem stage (this is the widespread rash stage). During the prodromal stage, one of the first signs of measles occurs in the head and neck region, including the oral cavity.
Koplik spots, an early symptom of measles, appear as tiny grains of white sand surrounded by a red ring. They are especially prevalent on the insides of the cheek adjacent to the first and second molars. These lesions appear two to three days before other symptoms, and they have been noted in 50% to 70% of patients with measles.5 Koplik spots may alarm patients and send them running to their dentist to have these lesions evaluated. Due to vaccines and the suppression of many infectious diseases, including measles, many dental professionals have never seen these lesions firsthand.
Now might be a good time to brush up on your oral pathology, particularly Koplik spots. In addition to observing Koplik spots in the prodromal stage, patients may also present with fever, conjunctivitis (pink eye), coryza (inflammation in the mucous membrane of the nose), and coughing.
The pediatrician, Dr. Henry Koplik, was the first to describe these spots and associate them with early signs of measles. Diagnosing contagious and deadly diseases such as measles without modern-day diagnostic tests was no easy task. In the 19th and 20th century, early diagnosis of measles was crucial in reducing the number of people infected.6
Dr. Koplik’s description of these oral lesions in his own words: “We see a redness of the fauces; perhaps, not in all cases, a few spots on the soft palate. On the buccal mucous membrane and the inside of the lips, we invariably see a distinct eruption. It consists of small, irregular spots, of a bright red color. In the center of each spot, there is noted, in strong daylight, a minute bluish white speck. These red spots, with accompanying specks of a bluish color, are absolutely pathognomonic of beginning measles, and when seen can be relied upon as the forerunner of the skin eruption.”5
By identifying Koplik spots, we can assist in early diagnosis and reduce the number of individuals exposed.
Studies show the measles virus is associated with profound and prolonged immunosuppression for weeks to years following clearance of the virus. This is possibly due to suppression of lymphocyte proliferation.7 This information should make dental professionals hyperaware of the increased risk of oral bacterial infections, viruses, and fungal infections in patients recovering from the measles. Immunosuppression affects defense mechanism found in the oral cavity and creates the perfect conditions for the proliferation of bacteria and the overgrowth of fungus.
The most current reports from 2016 state that 91.1% of the US population has been vaccinated for measles. However, vaccine levels continue to vary with vaccine levels below 90% in some areas. Pockets of unvaccinated people exist in some states with high vaccination rates, causing susceptibility at some local levels.
The World Health Organization has committed to eliminating the measles by the year 2020.8 With the current number of cases, I’m not sure they will meet their goal. Dental professionals can be a front-line defense in reducing the spread of measles by being aware of early symptoms. Though Fordyce granules have been mistaken for Koplik spots in the past, referring patients with suspicious oral lesions to their medical doctor is advised, especially in areas that are experiencing an outbreak.
References
- Centers for Disease Control and Prevention. Measles Cases and Outbreaks: Measles Cases in 2019. https://www.cdc.gov/measles/cases-outbreaks.html
- Guerra, F.M., Bolotin, S., Lim, G., et al. The Basic Reproduction Number (R0) of Measles: A Systemic Review. Lancet Infect Dis. 2017; 17(12): 420-428. https://www.ncbi.nlm.nih.gov/pubmed/28757186
- Centers for Disease Control and Prevention. Transmission of Measles. https://www.cdc.gov/measles/about/transmission.html
- Williams, J. (2015) SCIENCE: Signs of Measles may appear in Oral Cavity Before Other Manifestations of Disease. American Dental Association. https://www.ada.org/en/publications/ada-news/2015-archive/march/symptoms-of-measles-may-appear-in-oral-cavity
- Steichen, O., Dautheville, S. Koplik Spots in Early Measles. CMAJ. 2009; 180(5): 583. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2645467/
- Markel, H. Koplik’s Spots: The Harbinger of a Measles Epidemic. Milbank Q. 2015; 93(2): 223-229. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4462869/
- Permar, S.R., Griffin, D.E., Letvin, N.L. Immune Containment and Consequences of Measles Virus Infection in Healthy and Immunocompromised Individuals. Clin Vaccine Immunol. 2006; 13(4): 437-443. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1459643/
- Centers for Disease Control and Prevention. Frequently Asked Questions about Measles in the U.S. https://www.cdc.gov/measles/about/faqs.html#concern