The bridge between medical and dental health is a hot topic and one we as dental hygienists cannot ignore! A lot is being done to try to build this bridge and shorten this gap, particularly with one of the most well-known and direct oral-systemic connections – diabetes and oral health. Our hygiene profession and the care we provide our diabetic patients will improve greatly by our collaboration with other medical professionals.
Along with our dentists, we can help bridge this gap by:
- Working with and referring our patients to appropriate medical professionals to discover or manage their diabetes
- Collaborating with local certified diabetes educators
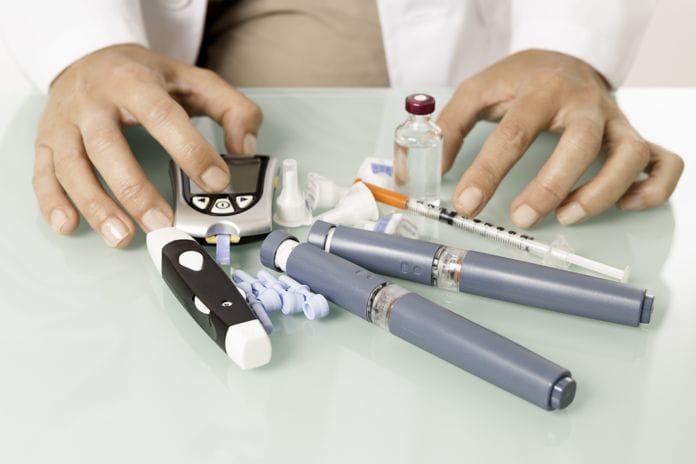
- Incorporating chairside HbA1C screening of our suspected diabetic patients!
As healthcare professionals, dental hygienists know there is a proven connection between the mouth and the rest of the body, particularly in diabetics. We work tirelessly trying to explain the oral-systemic connection to our patients; day in and day out. As dental hygienists’ we know oral manifestations associated with diabetes are1:
- Periodontal disease
- Dental caries
- Burning mouth syndrome
- Oral candidiasis (common in those with poor glycemic control)
- Salivary dysfunction
- Neurosensory disorders
- Soft tissue abnormalities such as stomatitis or lichen planus
- Xerostomia
Our daily role as dental hygienists
We can agree that the treatments, preventative care, and education we render in our operatories every single day, have a direct impact on our diabetic patients’ overall health. Vital things to do in clinical practice:
- Document and regularly update a thorough and complete medical history, looking for clues that a patient could be an undiagnosed prediabetic or diabetic.
- Ask when our patients’ last check-up with a physician was, and encourage them to keep their medical visits current.
- For our known diabetics, we ask what their last A1C reading was, and note changes in medications or other health conditions.
- Perform a thorough and complete initial oral and periodontal examination, and use this for all subsequent thorough and complete periodontal examinations and closely monitor for changes.
- Educate our diabetic patients on how their periodontal health, bacterial plaque control, and nutrition can help control their diabetes and vice-versa. We know that the work of oral health professionals is vital to helping manage diabetes. We realize that a diabetic’s glycemic control can be affected by their periodontal disease and that their periodontal disease can be worsened by poor glycemic control.
- Provide treatments in our office that directly help our diabetic patients. It has been shown that in periodontal patients, scaling and root planing procedures can sometimes be as effective to diabetes management as adding a secondary diabetes medication2.
- Modify their preventive care cycle, scheduling them for periodontal maintenance or dental hygiene visits in our office every 3 to 4 months.
Certified diabetes educators working to bridge the gaps
We can agree that the treatment of chronic systemic diseases such as diabetes are beyond what our profession can handle on its own, and therefore, collaboration with other medical professions is key to helping these patients. The American Academy of Diabetes Educators (AADE) is one such organization focused on bridging the gap between medical and dental professionals for this disease with the clearest oral-systemic links. This organization has more than 14,000 professional members – including nurses, dietitians, pharmacists and exercise specialists.
“Diabetes educators can be found in a variety of settings: hospitals, physician offices, clinics, home health, wellness programs, to name a few. They most often work within accredited or recognized diabetes education programs3.”
In April 2016, an oral health summit was sponsored by Colgate and the American Association of Diabetes Educators, ADHA and ADA and other medical professionals. They sat around a table for two days and came up with a white paper for objectives on collaboration. The “Diabetes and Oral Health” white paper states, “When considering diabetes and oral health, the goal is to create synergy between the diabetes education community and the oral health care community. Both groups can effectively work together as part of the healthcare team to benefit patients’ long-term outcomes. Chronic disease management occurs over decades and is best accomplished when multiple health care providers work together. The likelihood of patients understanding and adhering to treatment suggestions increases when a consistent message is delivered by all healthcare providers4. ”
As dental hygienists, we know we must look at our diabetic patients as a whole. This may mean encouraging them not only to be monitored closely by their primary care doctor but also ask them if they are being evaluated annually by an ophthalmologist, a podiatrist and discussing their eating and exercise behaviors or encouraging referral to an exercise specialist or dietician. Another avenue being explored is having registered dieticians see patients within the dental office – and Medicare may cover this. Medicare covers Diabetes Self-Management Training (DSMT) provided by a registered dietician no matter where these services are performed, but as of now, they will not cover it for caries control.5
To provide the best patient, care we may wish to begin collaborating and networking with certified diabetes educators. This can easily be done by finding a local diabetes education center made up of medical professionals. We can also refer our patients to their local diabetes education center. One such resource to find a diabetes educator is https://www.diabeteseducator.org/patients/find-a-diabetes-educator. These groups work with patients to develop a plan and provide tools to help diabetic patients get and stay healthy. Diabetes education is recognized by Medicare and most health insurance plans when it is offered through an accredited diabetes education program which has met criteria of the U.S. Department of Health & Human Services. We can reach out to these professionals to educate us further on the most current nutrition, medications, and even appropriate exercise for our diabetic patients. Developing such a relationship with such a center means perhaps they can then refer to us for needed periodontal treatment or prevention. Perhaps we can also share with them the treatments and oral hygiene instructions we know so well. Dental professionals have and also may also consider becoming certified diabetes educators themselves.
Screening for diabetes in the dental office
Not only can we work with our patients and other professionals to help improve their management of diabetes, but dental hygienists are instrumental in helping patients that don’t even realize they are diabetic or pre-diabetic. Dr. Jerry Brown, the first dentist to become a Board-Certified Diabetes Educator, has done much to provide awareness with his lecture “Diabetes Mellitus and the Dental Professional” with Colgate and the American Dental Association. Dr. Brown states, “Dental hygienists can have a major impact on healthcare by having a part in the process,” stated, “They are on the front lines.”
Coming full circle to help us screen for pre-diabetes and diabetes, a new procedure code for simple chairside blood sugar testing is going to be implemented in the American Dental Association’s CDT 2018 – D0411 (HbA1c – in office point of service testing). This code, effective January 1, 2018, has come to fruition due to the hard work and collaboration of very knowledgeable dental professionals as well as healthcare providers that are also certified diabetes educators.
This test can help screen how well a diagnosed diabetic is controlling their diabetes, as it is in an indicator of glucose control for the last 2 to 3 months. Along with health history taking and oral examination, it can help dentists with patients that have undiagnosed diabetes or prediabetes. In one recent study of more than 500 patients, dentists were able to spot 97 percent of those with diabetes by doing a regular dental exam and giving patients an in-office A1C test.6
In a Podcast with the vice president of the Australian Dental Association Vice President Dr. Kathleen Matthews, Dr. Brown states that certain risk factors indicate a person is metabolically challenged. Systemic risk factors that indicate a potential for diabetes or pre-diabetes include:
- Overweight or obese – BMI greater than 25
- High blood pressure
- Familial history of diabetes
- High cholesterol
- History of heart disease
- Other symptoms or complaints may include thirst, urinating frequently, constant fatigue, weight loss (Type 1), blurred vision, and uncontrolled infections even within the mouth (poorly controlled Type 2 diabetics).
Dr. Brown also states that there are dental clues indicating a metabolic challenge. A patient that has 26% of periodontal pockets measuring 5 mms or greater or 4 or more missing teeth (not including the third molars) has a 72% chance of having a metabolic challenge. A chairside diabetes HbA1c (Hemoglobin A1c) test performed in our practice showing a result of 5.7 or greater indicates a 92% chance the patient is metabolically challenged. At this point, the patient should be referred to their physician.
90% of pre-diabetics are unaware of their condition. 25% of type II diabetics are unaware they have the disease. This chairside HbA1C test can be an invaluable tool in helping our patients with prediabetes or diabetes.
*Before incorporating this test into your practice, however, you must check with your state’s Dental Practice Act to see if the testing is within your scope of practice under your license.
Treatment planning for the diabetic patient
Knowing a patient’s most current HbA1c should also absolutely be taken into account when treatment planning for dental care. For patients with a high HbA1c reading, their immune response to dental treatments can be hampered due to the systemic inflammatory response caused by diabetes. A diabetic’s host response becomes dysfunctional, throughout their entire body and subsequently in the mouth. This is very important to know when treatment planning for diabetics and anticipating their healing results – especially with dental implants and other surgical procedures.
| Immune response review:
As we recall, diabetes is an inflammatory disease. Cytokines are released into a diabetic patient’s systemic network and then into the oral capillaries subgingivally. This host response causes problems with tissue destruction. Osteoclasts and osteoblasts are stimulated into destroying bone and connective tissue. The normal periodontal and oral reparative function is hindered by high concentrations of sugar in the blood, causing less fibroblast and osteoblast activity. This then hampers response of neutrophils which are the first blood cells to defend against bacterial invasion, causing a field day for bacterial invasion and bacterial multiplication.7 Also, realizing that untreated periodontal disease may directly affect a diabetic patient’s glycemic control. When a diabetic patient has periodontal disease, you then have inflammation in the gums, with cytokines present subgingivally, and bacterial byproducts make their way into the subgingival capillary network to systemic circulation. This toxic environment reaches the muscles, liver and fat cells, hampering insulin receptors from functioning and this creating insulin resistance. Glucose stays in the blood instead of manufacturing energy in the cells.
|
Since dentists may see patients more frequently than other healthcare providers, they are in a great position to implement this test in their practice for known or potential diabetic or prediabetes patients!
What an exciting time to be a hygienist! We are in a great position to help our diabetic patients both with their oral and systemic health. After all, we do happen to know a thing or two about treating and managing a disease that is considered autoimmune, chronic, and can be treated and managed but not cured, and sometimes prevented with early intervention through diet, exercise, behavior and lifestyle choices!
Now Listen to the Today’s RDH Dental Hygiene Podcast Below:
Resources
- http://clinical.diabetesjournals.org/content/32/4/188.full
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4439629/
- https://www.diabeteseducator.org/education/becoming-a-diabetes-educator
- https://www.diabeteseducator.org/docs/default-source/default-document-library/aade-diabetes-oral-health-white-paper.pdf?sfvrsn=2
- https://www.medicare.gov/coverage/diabetes-self-mgmt-training.html
- http://www.diabetes.org/research-and-practice/patient-access-to-research/smile-dentists-and-doctors.html?referrer=https://www.google.com/
- http://appro.bppcloud.net.au/index.php?option=com_content&view=article&id=672