Note: This is Part 1 of Debbi Viger’s series, Special Needs: Everyone Has Special Needs
All of us are special in some way and require adjustments to our treatment and our daily life. Let’s just embrace that concept for a moment, take a deep breath and strive to create excellence for ourselves and our patients. So often we read in blogs the negativity associated with patient requests, but we can turn that around and make every moment a teachable moment. Each of us has experienced the patient that despises everything and has a laundry list of demands. This Crabby Abby usually has sensitivity, hemorrhaging tissues, a strong gag reflex, and needs to remain upright. Our challenge becomes meeting these needs and performing all necessary treatment in the appointed time.
Ready to be a hygiene cheerleader?
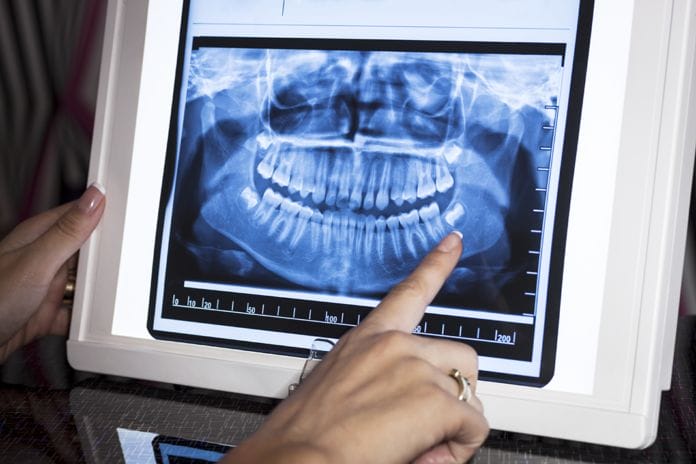
Create exceptional experiences one step at a time. It starts from the moment you greet your patient. Assess the mood, gait, facial expression and then begin making the appointment fabulous. After talking through the medical update, let’s assume radiographs are needed. Your patient is anxious and already needy. We need to ask flat out, what they are anxious about. Is your patient worried about gagging? Are they worried about tori getting banged up? Cost? Radiation exposure? Time? We cannot fix the issue until we understand what the issue is.
Now comes the cheerleading. We all know many tips and tricks to fix particular problems. Express your understanding, empathy and a solution. If gagging is the worry, explain that many gag because the airway is pinched off and breathing becomes difficult and fearful. If you have your patient tip their chin up, the airway is wide open. Hence, the sensor does not feel like it is moving backward and breathing is impaired. If the issue is the tori, demonstrate how you can position the sensor on the tongue, or use a soft wrapper or gauze to cushion the tissues. Having the patient bite slowly and then allowing the patient to open immediately after the beep, gives the patient control. Some clinicians have had success with salt on the back of the tongue or applying topical anesthetic. Try multiple techniques and be sure to make notes in the chart to make the next appointment that much easier and more comfortable for the patient.
Is the Issue Cost?
How long has it been since the last series of radiographs? Explain to the patient why radiographs are needed. Is this patient caries prone? Were there questionable areas in the past? Can they be stalled for today and taken at the next recare appointment? Offer options and rationale. If the patient is concerned about cost, perhaps a decision can be made after the exam if something suspicious is seen. Can fluoride or other charges wait until the next appointment to accommodate the radiographs today? Most importantly, we want to show respect and that we are truly excellent listeners trying to meet their needs. Ultimately if someone refuses treatment based on finances, we must respect that decision. No one should ever feel judged or embarrassed by making a difficult decision based on financial needs. Allow the patient control while accomplishing exactly what you need for a successful outcome.
If radiation is a concern for your patient, ask why.
Have they had multiple exposures recently? Pregnant? If so, can we wait until the next appointment? If there is not an emergent situation that requires immediate radiographs, perhaps you can hold off. Is it a general fear of radiation? Keep a visual aid handy that demonstrates the actual amount of radiation exposure from dental radiographs versus that found in nature or travel. Frequently, patients are afraid of the unknown or are ill-informed, and education can change everything. The more information we have handy, the better we can help create a positive outcome through science and understanding.
If the issue is time, we can perform the prophylaxis first, and take the radiographs in those moments when we may be waiting for the examination.
We have the ability to help patients truly enjoy attending dental visits. Respect, excellent listening, and altering our actions to affirm their special needs, allows our patients to trust us and relax while in the dental chair.