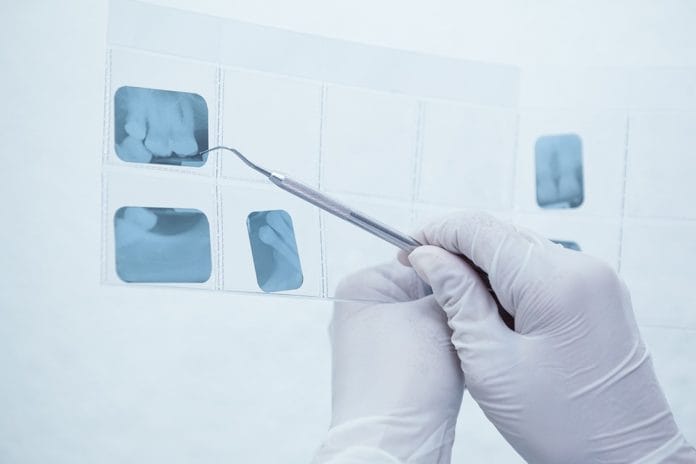
What’s your hygiene moment when you realize you have had an epic fail? Hopefully, none of you will ever have that experience, but I did, and I am on a mission to never let it happen again. Here’s the scenario, the patient presents for routine care. It’s a great appointment – everything status quo; health history reviewed, oral cancer exam, TMJ evaluated, examined for decay, periodontal charting completed, airway evaluated – all great on the exam. Radiographs were exposed and all still looking great. Prophylaxis and fluoride completed, life is great, and I am still on time, smooth sailing into breaking down the room and sterilizing instruments.
Several months later, however, this patient calls in stating after eating, it felt as though something was lodged under the tissue. It started out very painful, but after much flossing, rinsing, and digging with a toothbrush, it was subsiding. The office requested to see the patient to make sure the tissue was truly healing, and there was no treatment needed.
The patient presents back in my hygiene chair for evaluation. After describing the situation, one bitewing and one periapical radiograph are exposed. Here’s what breaks my hygiene heart. There is an area of decay just under the crown margin. This tooth will not be restorable, and the patient is scheduled for extraction and implant placement.
Here is where I am having an issue, four months prior I am the hygienist who treated this patient, I am the hygienist who took his bitewing radiographs specifically to ward off any future issues and treat accordingly. My doctor, very kindly, reminded me why perfection is so important for each and every radiograph. In the last set of bitewings, I was so careful to get the distal of the last molar and as far forward as the distal of the canine; I concentrated on making sure the contacts were open in at least one of the views either molar or bicuspid. What I did not adequately get was the bone level of every posterior tooth. Had I been able to see the bone, perhaps this area of decay would have been noticed earlier, perhaps not, but I would not be left so sad.
Looking back to the bitewings about 18 months prior, no pathology was noted, which gives me some consolation. Yet, I feel I should have been more aware; I feel I should have taken another bitewing to make sure I covered every area. The thing is, for me, it wasn’t even on my radar. I, a licensed hygienist since 1986, with tons of experience, thought the radiographs looked great, moved on with the appointment, satisfied I had completed my hygiene mission.
What I now know, and will encourage all to do, is to take that extra moment to really evaluate, with a more discerning eye, each radiograph. Our office is very particular; we strive to make each radiograph textbook quality as if each patient will need to be referred out for treatment. It is constantly shocking to me when we receive a set of radiographs which are completely useless for diagnosis. How was any treatment need even assessed? Explaining to a patient we prefer only to use radiographs we have taken, explaining digital radiographs have very limited radiation exposure, and we would rather take radiographs complimentary, so we have a comprehensive picture to diagnose their oral health, takes a lot of time and energy, yet is completely worth the investment of time.
We truly do need to see each apex in a full-mouth set of radiographs, which is why we take them. We truly need to see each contact, and as I now know, we do need to see bone levels in the bitewings on each tooth. Please don’t get me wrong; we have all had those patients with huge tori, where access is extremely limited, or patients who are fearful or gaggers, patients who refuse X-rays, or patients that can’t stay still. Not at all am I judging your particular situation or the cooperation of your patient. I am, unfortunately, true-confessing I had an experience that was less than ideal because the patient was perfect, and I was not.