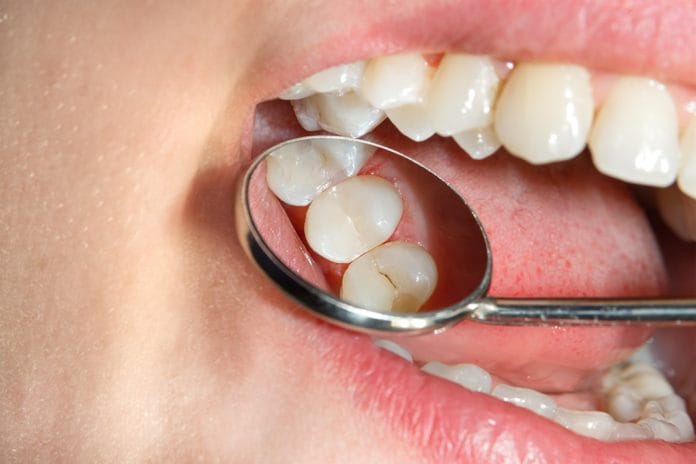
We have all experienced the child patient who sits down in your chair after having sealants placed six months ago … and they’re gone. Just like the mystery behind the establishment of Stonehenge, it’s the curious case of the missing sealants!
Looking back, you were the one who placed them, and the progress notes indicated no issues. You did not note difficulty with isolation, no excessive salivary flow, or any other problem. Where did they go?
Here are the top six reasons your sealants fail that have nothing to do with saliva or keeping a dry field.
1) Hypomineralization
Consider that the teeth are more hypomineralized than they appear. It has been repeatedly demonstrated that spikes in body temperature can affect the development of enamel tubules.1,3 Fevers occur often in underdeveloped immune systems, such as those children under the age of three.
Which teeth are most likely to be affected by fevers under the age of three? The first molars and the central incisors – hence the research term “MIH,” referring to molar-incisor-hypomineralization.3
So what is the significance of enamel hypomineralization in relation to sealant retention? Put simply, they do not etch.1,2 Some scientists suggest that etch times must be increased on a hypomineralized tooth in order to achieve the same level of microporosity of a normal tooth following acid etching.3 No micropores, no retention.
This contrasts with what one would think since hypomineralized teeth are already more porous, right? The chemical makeup of teeth are highly different after an assault such as a high fever during development, causing changes in the amount of proteins present on the surface, as well as changes in the amount of hydroxyapatite in enamel.3
It is not as simple as a hard tooth vs. a soft tooth. The differences in a hypomineralized tooth vs. a normal tooth are not as easily defined as a wavy appearance of the enamel tubule, comparable to an aberration in a diamond. There is more to it than that, and the chemical composition in the weakest areas are actually different than those in stronger areas of enamel.3
So, please keep a record of the length of time you etched in the chart notes. Do not always assume that the tooth simply was not isolated, and that is why they failed. You cannot repeat the same action over and over, expecting different results. You must etch longer.3 If you etched for 60 seconds the first time, etch for a minute and a half.
2) You didn’t rinse off all of the etch
This has been studied well also, and some brands of etch add extra colorant to make sure that you can physically see the fact that the etch still lingers, even after a good rinse. The optimal rinse time is a full 15 seconds of water.7
If the etch is still there in the grooves, the sealant will never adhere. Do not rinse for three seconds until it appears as if the big blue glob is gone. Rinse it, and rinse it well.
3) Technique
Do not be fooled by the tiny lumens of some sealant brand tips. Yes, they are tiny! They are almost the size of an explorer. But they’re not. The lumen tip is blunt, whereas the tip of your explorer is tapered, allowing for more penetration into the deep pits of the tooth.
Don’t expect the sealant material to be so flowable that you don’t have to move it around with the explorer.
4) Pumice
This is a personal choice, and studies have found absolutely no difference in preparing the surface of a tooth with a prophy brush and just water, a regular toothbrush with water, or using pumice.8 I have found that pumice is very difficult to wash away, especially in the pits of a tooth, and I often will find remnants of the pumice when I am drying the tooth for the etch placement.
So, I do not use pumice at all and prep the occlusal of the tooth with a simple, slow-speed powered, angled prophy brush before a sealant.
5) Fissurotomies and stain
If those grooves are badly stained, your retention will be lower because of the inability to truly clean the surface.4 The tooth’s surface has already undergone some microscopic changes, indicated by the dark appearance of the grooves.
Do not be afraid to ask your doctors to perform a quick fissurotomy on a few stained areas before you seal them, thus ensuring your success.4
6) Products
The concentration of your etch must be greater than 35% phosphoric acid to achieve the etch you need to achieve for successful sealants.3 Additionally, consider your sealant material with regard to the percentage of filler. While filled resin sealants are a stronger material after placement, some studies show that its inability to flow well into the microporosities decreases the bond strength.5,6
In conclusion, there are a variety of reasons your sealants may be failing, and they do not necessarily have anything to do with your application technique.
If you are interested in more information regarding molar hypomineralization and management, there is a wonderful free continuing education course from Colgate’s website offered by Erin Mahoney and Mike Hubbard. They are affiliated with the charitable organization called D3- Developmental Dental Defects, and more information can be found for patients at chalkyteeth.org. Their organization is endorsed by the International Association of Paediatric Dentistry, International Federation of Dental Hygienists, Australian Dental Association, New Zealand Dental Association, The Dental Hygienists’ Association of Australia, Inc., among others!
Now Check Out the Peer-Reviewed, Self-Study CE Courses from Today’s RDH!
Listen to the Today’s RDH Dental Hygiene Podcast Below:
References
- Williams, R., Perez, V., Mangum, J., et al. Pathogenesis of molar hypomineralisation: hypomineralised 6-year molars contain traces of fetal serum albumin. Frontiers in Physiology. 2020; 11: 619.
- Krämer, N., Bui Khac, N.N., Lücker, S., Stachniss, V., Frankenberger, R. Bonding strategies for MIH-affected enamel and dentin. Dental Materials. 2018; 34(2): 331-340.
- Hubbard, M.J., Natarajan, A., Antoun, A., et al. The molar hypomineralisation problem: translational science,paediatric and orthodontic perspectives. New Zealand Dental Association News. 2019 Oct; 195: 35-60.
- Bagherian, A., Akbar, M., Rezaeian, M., et al. Micro leakage assessment of fissure sealant following fissurotomy bur or pumice prophylaxis use before etching. Dental Research Journal. 2013 Sept-Oct; 10(5): 643-646.
- Naaman, R., El-Housseiny, A., Alamoudi, N. The use of pit and fissure sealants-a literature review. Dentistry Journal. 2017 Dec; 5(4): 34.
- Reddy, V.R., Chowdhary, N., Makunda, K.S., et al. Retention of resin-based filled and unfilled pit and fissure sealants: a comparative clinical study. Contemporary Clinical Dentistry. 2015 Mar; 6(Suppl 1): S18-S23.
- Fallahzadeh, F., Atai, M., Ghasemi, S., et al. Effect of rinsing time and surface contamination on the bond strength of siloxane-based and dimethacrylate-based composites to enamel. Journal of Clinical and Experimental Dentistry. 2018 Nov; 10(11): e1115-e1122.
- Farsi, P., Uribe, S., Vig, K., et al. How to clean the tooth surface before sealant application. Journal of the American Dental Association. 2009; 140(5): 516-517.