Scleroderma is an autoimmune connective tissue and rheumatic disease that causes inflammation in the skin and other areas of the body, including the face and mouth. Oral manifestations of scleroderma may directly affect a person’s ability to maintain optimal oral health. Dental hygienists may be the first health care provider to note scleroderma.
Early detection, medical referral, and treatment are important to reduce the impact of the disease on the oral tissues and other body systems.
What is Scleroderma?
The cause of scleroderma is unknown. Researchers theorize that the immune system overreacts and causes inflammation and injury to the cells that line blood vessels. This triggers connective tissue cells, especially a cell type called fibroblasts, to make too much collagen in the skin and other organs, leading to the signs and symptoms of scleroderma.7
The American College of Rheumatology and the European League Against Rheumatism collaborated to devise a classification system aimed at delimiting scleroderma against other connective tissue diseases.2 The two main categories of scleroderma are localized and systemic.
Localized Scleroderma
Localized scleroderma affects the skin but not the major organs. Lesions may heal and disappear. There are three types of localized scleroderma:
Circumscribed morphea ‒ Discolored patches of skin that may vary in size and typically have a red border and a thickened yellow center. The lesions might enlarge when active and then flatten and become asymptomatic with treatment.5
Generalized morphea ‒ Indicates more than four patches in areas like the trunk, arms, head, and neck. The lesions are thick, tight patches that may blend in groups.
Linear scleroderma ‒ This type is more common in children aged 10 and younger. Tight, thick bands may appear on the extremities, back, chest, butt, or face. Linear scleroderma may affect bones and muscles, causing a child’s limbs to underdevelop.5,7
Systemic Scleroderma
Systemic scleroderma, also known as systemic sclerosis, has three types:
Limited systemic sclerosis ‒ This is the most common type. The skin hardening and skin tightening are limited to the fingers and sometimes the hands, forearms, or face. Internal damage is less likely.2,7
CREST is a subtype of limited systemic sclerosis that includes calcinosis, Raynaud’s phenomenon, esophageal dysfunction, sclerodactyly, and telangiectasia.7
Diffuse scleroderma ‒ This type presents as skin thickening over large areas of the body ‒ fingers, hands, arms, anterior trunk, legs, and face. This type of scleroderma can be associated with significant organ damage. Patients may experience dryness, itching, and musculoskeletal pain.2,7
Sine sclerosis ‒ This is systemic scleroderma that has features of systemic organ disease, including Raynaud’s phenomenon, but none of the skin symptoms. The patient may experience symptoms and complications of either limited or diffuse sclerosis without any skin thickening.2
Scleroderma Diagnosis and Treatments
Scleroderma is more common in women than men, affecting women 3:1 and usually appearing between the ages of 30 and 50 years old.2,7
Scleroderma can be difficult to diagnose because the symptoms resemble many other diseases. There is no single test to diagnose scleroderma. Scleroderma is most often diagnosed by a rheumatologist or dermatologist by a combination of a thorough exam and medical history, symptoms, biopsy of affected skin areas, urine, blood, and other tests to assess the extent of the disease’s effects.1,6
There is no cure for scleroderma, and patients find pain relief through nonsteroidal anti-inflammatory medications or corticosteroids. Phototherapy, skin lotions, and moisturizers may soothe and heal itchy skin.
Treatment goals are to slow skin thickening and minimize damage to the internal organs with phototherapy and medications such as methotrexate and cyclosporine that:
- Suppress the immune system
- Maintain muscle strength through physical therapy and exercise
- Manage digestive tract function to optimize nutrient intake
- Improve emotional state with counseling
- Improve blood pressure control and blood flow with medication6
Oral Manifestations of Scleroderma
The head and neck are involved in 70% of systemic sclerosis cases.8 There is a high prevalence of abnormalities of the oral cavity and surrounding tissues with one or more features evident in virtually all patients with scleroderma. Patients with early or limited forms of scleroderma may present to a dental professional with detectable clinical features before a formal diagnosis has been established.11
Characteristic extraoral features are a mask-like appearance, pinched nose, atrophy of the ala of the nose, thin and rigid lips, and loss of skin folds on the face.8
Intraoral exams may show an inability to open the mouth wide (microstomia), tongue rigidity, xerostomia, pigmentation, mouth ulcers, telangiectasia, periodontal disease, pulpal calcifications, trigeminal neuralgia, and affected tissues around the temporomandibular joint can result in pseudoankylosis.4,8
Secondary oral manifestations include tooth mobility, dental caries, candidiasis infection, subluxation, and altered mandibular guidance. Esophageal dysmotility may cause acidity due to gastroesophageal reflux that leads to dental erosion and dental caries.8
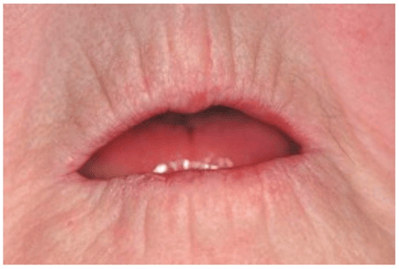
Microstomia is a reduction in the size of the oral aperture caused by tissue remodeling of the TMJ capsule (see Figure 1). Reduced ability to open a person’s mouth complicates the maintenance of oral hygiene, dental treatment, and prosthetic rehabilitation and can also lead to difficulty with chewing and swallowing. Patients may also lose strength in their face and lips, causing difficulty with speech, facial expression, and saliva control.11
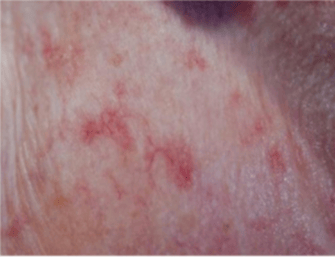
Telangiectasias are small, widened blood vessels on the skin and develop in exposed cutaneous regions of the hands and face, which has aesthetic implications (see Figure 2). They can also be found on oral mucosal surfaces (typically the labial mucosa) but are not a significant clinical risk when found intraorally.11
Xerostomia is reported in two-thirds of patients with scleroderma, with moderate to severe cases in over half of those patients. Xerostomia is caused by two mechanisms in scleroderma. The first is immune-mediated destruction of acinar tissues, and the second is fibrosis of salivary glands themselves, reducing their exocrine capacity.
Xerostomia may additionally be exacerbated by medications that do not damage the salivary glands but block the nerves that stimulate salivary glands to work. The loss of lubrication to oral tissues causes patients to experience difficulties with speech and swallowing, and their sense of taste becomes blunted.11
Thrush, which is white patches that wipe off, is a common fungal infection unlikely to be painful and can be a side effect of immunosuppressant and steroid medication. Lichen planus is white patches that do not wipe off that may become painful. Lichen planus affects the buccal mucosa, tongue, and gingiva. Mouth ulcers, tingling or numbness of the lower lip called trigeminal neuropathy, reduction in tongue size, and in extremely rare cases, fibrosis of the tongue may present in patients with scleroderma.10
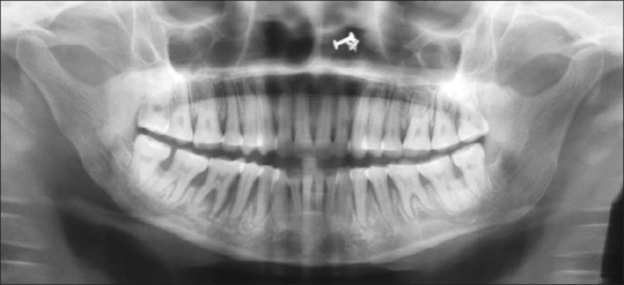
Radiographs may show varying degrees of bone resorption in patients with scleroderma. Mandibular resorption has been reported in 10% to 33% of patients with systemic sclerosis.11 Osteolysis is documented resorption of the mandibular angle and condyle of adult patients with scleroderma (see Figure 3). The etiology is not known. However, it is theorized that:
- Tightening of facial skin may exert excessive pressure on the mandible and induce bone loss
- Vasculopathy associated with systemic scleroderma may diminish the blood supply to the mandible and induce bone loss
- Atrophy of the muscles of mastication may lead to cone necrosis.
Uniform widening of the periodontal ligament space, especially around posterior teeth, is common.4,11
Dental Treatment Considerations
There are three main issues identified that play a critical role in patients with scleroderma in the context of dental therapies. Xerostomia-induced ulcerations and inflammation of oral mucosa, functional impairment of the masticatory organ and associated dysphagia, and variably configured fibrosis leading to retraction of the lips with hallmark perioral wrinkles and impaired mouth opening are all factors to be considered at dental appointments.2
A medical consult prior to dental treatment is generally not advised for patients with scleroderma, assuming the patient is under medical care. Systemic manifestations are well-controlled, and there are no stem cell transplant considerations. Medical clearance may be needed for some dental procedures if the patient is being treated with medications associated with immunosuppression. Antibiotic prophylaxis is not typically recommended for patients with scleroderma.3
Oral hygiene at home and dental appointments may be difficult for patients with scleroderma due to microstomia and reduced manual dexterity and finger flexion. Scleroderma may compromise a person’s ability to use a toothbrush or interdental aids. Dental hygienists might consider adjusting appointment times, implementing orofacial exercises, and adapting dental tools such as adding a larger grip to a toothbrush.11
Daily exercises that aim to stretch the tissues of the face and neck have been shown to improve mouth opening, but long-term outcomes are influenced by compliance and consistency.9,11 Dental hygienists may suggest oral stretching exercises like exaggerated facial expressions or manual cheek stretching one to two times a day with brushing or under a warm shower. Patients may also warm the muscles in the face and around the mouth with a warm compress before a dental appointment.9
Oral hygiene education for a patient with scleroderma should take into consideration loss of manual dexterity and strength secondary to fibrosis of the fingers.3 A dental hygienist might include suggestions on nutrition, avoiding sugar, good home care instruction, hand stretches, small head toothbrush, fluoride use, interproximal care, mouthwash, at least twice a year professional dental preventative care, and advise patients to seek medical advice if changes in the head or neck become concerning.10
When treating a patient with scleroderma:
- Keep appointments short.
- Use a mouth prop or dental hygiene assistant to suction and retract.
- Semi-supine position to avoid gastrointestinal problems like reflux.
- Supplemental oxygen may be indicated in patients with severe restrictive lung disease due to scleroderma.
- A room humidifier may help with excessive dryness.
- Keep a blanket available for those with Raynaud’s phenomenon (patients are often cold).
- Ultrasonic scaling and air polishing may not be appropriate if there is significant fibrosis of the hard and soft palate.
- Injections may be difficult due to induration, or the oral tissues and epinephrine may also exacerbate microangiopathy found in patients with scleroderma.
- Microstomia may increase difficulty in taking radiographs; use a size 0 or 1 sensor and regular panoramic radiographs to screen for bone resorption.3
Due to poor communication between dental professionals and rheumatologists, surveys have identified a high proportion of scleroderma patients who have had difficulty accessing a dental professional with knowledge of the disease. Oral manifestations may be overlooked and undertreated due to the focus on life-threatening internal organ involvement. Still, oral manifestations of scleroderma are common and negatively affect a patient’s quality of life.
A dental hygienist may be the first to note these manifestations and is an integral part of early detection and helping patients create a plan for optimal oral health outcomes in the presence of scleroderma.11
Now Check Out the Peer-Reviewed, Self-Study CE Courses from Today’s RDH!
Listen to the Today’s RDH Dental Hygiene Podcast Below:
References
- Scleroderma: Diagnosis and treatment. (n.d.). American Academy of Dermatology Association. https://www.aad.org/public/diseases/a-z/scleroderma-treatment
- Benz, K., Baulig, C., Knippschild, S., et al. Prevalence of Oral and Maxillofacial Disorders in Patients with Systemic Scleroderma-A Systematic Review. International Journal of Environmental Research and Public Health. 2021; 18(10): 5238. https://doi.org/10.3390/ijerph18105238
- Scleroderma. (2017, February 3). College of Dental Hygienists of Ontario. https://www.cdho.org/Advisories/CDHO_Factsheet_Scleroderma.pdf
- Jagadish, R., Mehta, D.S., Jagadish, P. Oral and periodontal manifestations associated with systemic sclerosis: A case series and review. Journal of Indian Society of Periodontology. 2012; 16(2): 271–274. https://doi.org/10.4103/0972-124X.99275
- Types of Scleroderma. (n.d.). Johns Hopkins Medicine. https://www.hopkinsmedicine.org/health/conditions-and-diseases/scleroderma/types-of-scleroderma
- Scleroderma Diagnosis. (n.d.). Johns Hopkins Medicine. https://www.hopkinsmedicine.org/health/conditions-and-diseases/scleroderma/scleroderma-diagnosis
- Scleroderma. (2020, February). National Institute of Arthritis and Musculoskeletal and Skin Diseases. https://www.niams.nih.gov/health-topics/scleroderma
- Panchbhai, A., Pawar, S., Barad, A., Kazi, Z. Review of orofacial considerations of systemic sclerosis or scleroderma with report of analysis of 3 cases. Indian Journal of Dentistry. 2016; 7(3): 134–139. https://doi.org/10.4103/0975-962X.186702
- Poole, J. L., Leader, D.M. (2017). Oral Exercises. Self-Manage Scleroderma. https://www.selfmanagescleroderma.com/lessons/oral-exercises.html
- Porter, S. (2021, May 12). Scleroderma symptoms – oral and dental. Scleroderma and Raynaud’s UK. https://www.sruk.co.uk/scleroderma/scleroderma-and-your-body/oral-and-dental/
- Veale, B.J., Jablonski, R.Y., Frech, T.M., Pauling, J.D. Orofacial manifestations of systemic sclerosis. British Dental Journal. 2016; 221: 305-310. https://www.nature.com/articles/sj.bdj.2016.678