Tooth enamel is the most mineralized substance within the human body. However, for approximately one in every ten individuals and one-third of children with celiac disease, the enamel exhibits defects. Enamel defects, as seen in amelogenesis imperfecta, render teeth more sensitive to temperature fluctuations and acidic foods, increasing caries risk. The cause of the enamel defects associated with celiac disease has remained largely elusive.1,2
A study published in Nature by Professor Jakub Abramson and his team at the Weizmann Institute of Science aimed to identify the association between celiac disease and amelogenesis imperfecta. The study revealed a previously unidentified type of IgA-dependent autoimmune disorder primarily affecting children, which impedes the proper development of tooth enamel. This disorder is particularly prevalent in individuals with a rare genetic syndrome and children who have celiac disease.1,2
The findings hold promise for developing early detection and preventive strategies for this perplexing dental disorder.1,2
The Study
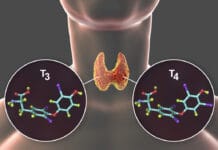
Tooth enamel is comprised primarily of mineral crystals that gradually accumulate on protein scaffolds during the developmental stages. Subsequently, the protein scaffold disintegrates, leaving a remarkably robust and protective layer. However, an intriguing anomaly emerges in the case of individuals afflicted by autoimmune polyendocrine syndrome type 1 (APS-1). While the enamel of their primary teeth forms normally, something disrupts the development of enamel in their permanent teeth.1,2
As patients with APS-1 typically grapple with various autoimmune diseases, Prof. Abramson’s team postulated that the enamel defects might also possess an autoimmune origin. Specifically, they suspected the immune system might improperly target proteins or cells necessary for enamel formation.1,2
Autoimmune diseases materialize when the immune system’s T cells or antibodies mistakenly incite an immune response against the body’s tissues. To prevent such “friendly fire,” T cells undergo education within the thymus gland, learning to differentiate between the body’s self-proteins and foreign entities. This educational process involves exposing T cells to fragments of self-proteins representing various bodily tissues and organs. Any T cell incorrectly identifying a self-protein in the thymus is flagged as a threat and subsequently eliminated, preventing potential damage upon release from the thymus.1,2
In patients with APS-1, this critical education phase is impaired due to a mutation in the autoimmune regulator (Aire) gene. The Aire gene is pivotal for facilitating the presentation of self-proteins to T cells in the thymus. The researchers discovered that in the absence of Aire, crucial enamel development proteins remain unexposed to T cells in the thymus, releasing T cells capable of recognizing these proteins as targets. This event prompts the production of autoantibodies against enamel proteins.1,2
An intriguing question arises: Why do these autoantibodies harm permanent teeth but not primary teeth? The answer lies in the timing of tooth development. Primary teeth form during the embryonic stage when the immune system is not fully developed and thus unable to generate autoantibodies.1,2
In contrast, permanent teeth begin enamel development at birth, continuing until around age six, coinciding with the maturation of the immune system. Consequently, the researchers observed a correlation between elevated levels of enamel-specific antibodies in childhood and the severity of enamel damage in children with APS-1.1,2
The researchers expanded their investigation to explore enamel development deficiencies in individuals with other autoimmune conditions, particularly celiac disease. Celiac disease, affecting roughly one percent of Western populations, triggers the immune system’s attack on the small intestine’s cellular lining upon exposure to gluten. Astonishingly, the study revealed a similar phenomenon in children with celiac disease, as they exhibited enamel defects akin to those seen in patients with APS-1.1,2
To identify the connection between celiac disease and enamel defects, the researchers investigated whether patients with celiac disease possessed autoantibodies targeting enamel. Notably, they found a substantial proportion of patients with celiac disease harboring these autoantibodies, mirroring the findings in APS-1 cases. Interestingly, the education process occurring in the thymus appeared normal in patients with celiac disease.1,2
The Results
The researchers proposed a hypothesis rooted in shared proteins between the intestine and dental tissue. They surmised that specific proteins, common to both locations, play a pivotal role in enamel development. Consequently, antibodies against proteins in the intestine might enter the bloodstream, infiltrating dental tissue and hindering enamel production.1,2
Given the prevalence of dairy sensitivity in patients with celiac disease, the researchers focused on k-casein, a prominent component of dairy products. Remarkably, they found that the human equivalent of k-casein constitutes a vital component of the enamel formation scaffold. This discovery prompted the notion that antibodies generated in the intestines of patients with celiac disease in response to specific food antigens, such as k-casein, might inadvertently disrupt enamel development in teeth. Notably, a significant number of children diagnosed with celiac disease exhibited elevated levels of antibodies against cow’s milk k-casein, which, in many cases, cross-reacted with the human k-casein present in the enamel matrix.1,2
Further, the pathogenesis of most autoimmune disorders is generally associated with IgG/IgM autoantibodies. However, recent research suggests that IgA autoantibodies primarily mediate certain epithelial and/or mucosal tissues. The researchers state, “finding IgA (rather than IgG) autoantibodies against the enamel matrix, which develops in the mucosal environment of the oral epithelium, seems to be well in line with these observations.”1 The researchers conclude, “Here we define an autoimmune disorder—autoimmune amelogenesis imperfecta—that is characterized by IgA autoantibodies against multiple enamel matrix proteins and impaired enamel development.”1
The implications of these findings extend beyond dental health, potentially impacting the food industry. Abramson cautioned that akin to the lessons learned from gluten, consuming copious amounts of dairy products might induce the production of antibodies against k-casein. While k-casein boosts cheese production, this research suggests it may be a potent immunogen, potentially triggering harmful immune responses.2
Conclusion
Tooth enamel defects are not limited to individuals with celiac disease or APS-1. Many people contend with enamel development impairments of unknown origin. The discovery of this new autoimmune disorder and the prospect of diagnosing it through blood or saliva tests holds the potential to shed light on these enigmatic conditions.1,2
More importantly, early diagnosis in children may pave the way for preventive treatments in the future, safeguarding their dental health and overall well-being.1,2
Before you leave, check out the Today’s RDH self-study CE courses. All courses are peer-reviewed and non-sponsored to focus solely on high-quality education. Click here now.
Listen to the Today’s RDH Dental Hygiene Podcast Below:
References
- Gruper, Y., Wolff, A.S.B., Glanz, L., et al. Autoimmune Amelogenesis Imperfecta in Patients with APS-1 and Coeliac Disease. Nature. 2023; 624(7992): 653-662. https://doi.org/10.1038/s41586-023-06776-0
- Weizmann Institute of Science. (2023, December 13). Newly Discovered Autoimmune Disorder Disrupts Tooth Enamel Development. ScienceDaily. www.sciencedaily.com/releases/2023/12/231213112542.htm