The Today’s RDH pandemic survey results are based on 2,602 responses to a Today’s RDH, non-scientific questionnaire posted on Facebook. The survey was posted on the Dental Hygiene with Kara RDH Facebook page, and responses were gathered from January 20 through February 11.
Less than 1% of the survey respondents indicated that they were not a resident of the United States. More than half of the respondents graduated from dental hygiene school between 1980 and 1999 (54%). More recent graduates (2000 through 2019) comprised 32% of the responses, and 91% of all responses said they were currently providing clinical treatment.
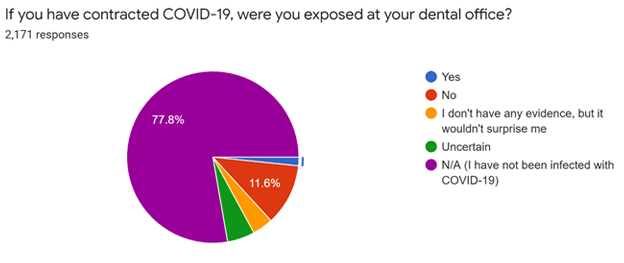
Ten percent of dental hygienists have been diagnosed as being infected with COVID-19. However, only 1.6% said the infection was traced back to their place of employment, according to the Today’s RDH survey.
Six percent of dental hygienists said they aware of incidents of coronavirus transmission in the dental offices where they work, and most hygienists believe employers are striving to provide safe workplaces for patients and staff. A nervousness about working as dental hygienists, though, remains a strong undercurrent in the profession.
“Dentists and office managers are mainly focused on production and not willing to compromise for the safety of their staffs and patients,” lamented one dental hygienist. “The workload is too high despite all the extra steps we need to take to battle with COVID. Many, many, many hygienists are putting their lives at risk because they have to provide for their families.”
Overall, 83% said they had not been infected. The other 7% believe they contracted the virus but were not officially diagnosed for it or think they were asymptomatic.
Employers Focus on Safety
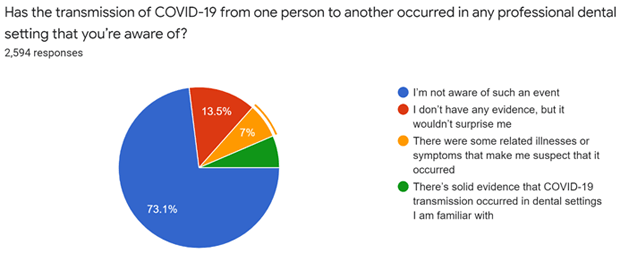
Although only a small percentage of the hygienists verified that they had contracted COVID, 50% of the respondents said they were aware of a professional colleague who had become infected. Again, though, only 7% said a transmission “from one person to another” occurred within the dental setting.
Because of the numerical differences, it may be worthwhile to review the two questions side by side. Figure 1 is the question asked after “Have you been diagnosed as being infected with COVID-19?” Figure 2 reflects the response after being asked, “Do you have any professional colleagues in the dental practice(s) where you work who were infected with COVID-19?” (Only 9% were “uncertain” about whether colleagues had COVID.)
For the most part, dental hygienists’ comfort level with employers providing a safe workplace remains high, according to this survey. Sixty-seven percent said they believe employers schedule patients and check-in arrivals to ensure “a safe flow of safe distancing throughout the dental facility.” Eighty percent said they feel their employer “heeds guidance” from public health experts about “business practices” during the pandemic.
The widespread acknowledgment of support for employers’ efforts may have been dampened, though, with a question regarding personal protective equipment. Only 38% said they were highly comfortable with the employer’s supply of PPE. The survey question asked hygienists to rate their responses on a scale of one to five: 12% chose “2,” which was next to the “highly comfortable” option; 10% chose “3”; 14% chose “4”; and 26% chose the “highly uncomfortable” option.
“Lack of PPE” was a common answer when the survey later asked hygienists about what makes them nervous about practicing dental hygiene during the pandemic.
One hygienist said, “Not being provided the proper PPE, N95 [mask], ability to change outer garment whether disposable or launderable, but also that the rest of the staff/owners feel the same about the importance of proper PPE.”
Many hygienists, of course, are eager to fulfill their role in COVID infection prevention, if they have not already done so; 75% said they will get the vaccine (the remaining 25% were evenly divided between not receiving a shot or being undecided on what to do).
Comfort with Dental Hygiene Treatment
Public health experts were concerned about the transmission of the coronavirus via aerosol droplets within the dental setting. The risk of transmission was a factor when determining whether dental employers needed to close down operations. Many guidance statements issued after offices were allowed to be reopened focused on aerosol generation and ventilation.
The Today’s RDH survey asked dental hygienists about both areas of concern.
Sixty percent of hygienists believe dental offices provide “safe, effective ventilation.” The remaining 40% of the responses were evenly split between “no” and “not sure.”
One hygienist added, “Open concept offices are common in my area. The front desk doesn’t understand their risk due to aerosols. Some offices didn’t allow extra time to clean between patients or let the air settle.”
Two separate questions were raised about ultrasonic scaler use and air polishing. The responses to dental hygiene treatment regarding the former included:
- Not using ultrasonics, only hand scaling (22%)
- Using HVE suction with no assistant (52%)
- Using HVE suction with an assistant (7%)
- Only using saliva ejector (28%)
- Wearing N95 respirator, fit-tested (15%)
- Wearing N95 respirator, not fit-tested (35%)
- Wearing ASTM level 3 mask (53%)
- Wearing ASTM level 1 or 2 mask (14%)
- Wearing face shield (71%)
The same responses (except for the first two options below) were offered regarding air polishing:
- Not air polishing due to pandemic (31%)
- I did not use an air polisher before pandemic (55%)
- Using HVE suction with no assistant (7%)
- Using HVE suction with an assistant (1%)
- Only using saliva ejector (11%)
- Wearing N95 respirator, fit-tested (3%)
- Wearing N95 respirator, not fit-tested (8%)
- Wearing ASTM level 3 mask (12%)
- Wearing ASTM level 1 or 2 mask (4%)
- Wearing face shield (16%)
In regard to air polishing, it’s important to note that 55% of dental hygienists did not use an air polisher even before COVID-19. The responses likely influenced the percentages above.
“Use of the ultrasonic device” was a common answer to a question about what makes dental hygienists “most nervous.”
Job Security
Dental hygienists did not seem to be terribly concerned about the impact of the pandemic on job security.
One question asked, “How concerned are you the number of doctors performing their own dental hygiene services will increase dramatically due to the pandemic?”
- 7% were “highly concerned”
- 47% were “not concerned at all”
- The question asked for a rating of one to five, with the latter being “unconcerned.” The other three groups trended downward toward being unconcerned by 21%, 18%, and 8%.
Another question asked, “How concerned are you that dental assistants will absorb greater responsibilities in providing dental hygiene treatment due to the pandemic?”
- 11% were “highly concerned”
- 47% were “not concerned at all”
- The question asked for a rating of one to five, with the latter being “unconcerned.” The other three groups trended downward toward being unconcerned by 19%, 14%, and 8%.
Nervous, More Nervous, and Gone
As mentioned above, the survey asked how many dental hygienists were still practicing clinically (91%). The questionnaire also asked the other 9% about why they were not practicing. The most common reasons cited by the 230 hygienists not practicing were:
- Retire early due to the pandemic (24%)
- Did not feel safe working clinically “at this time” (21%)
- Laid off or fired due to the pandemic (10%)
- Employer did not provide PPE or safe work environment (4%)
- Needed to stay home with children (3%)
The survey contained one open-ended question, asking dental hygienists what would “make you the most nervous about performing your duties as a dental hygienist during the pandemic?” Answers were optional, and 119 dental hygienists offered additional insights. The editors chose to include the responses below (limiting the word count devoted to this article):
- Aerosols, the physical burdens of high vac on my retracting arm, and more hand scaling. Also, hearing loss from high vacs and air purifiers.
- Everything makes me nervous. There is so much we really don’t know. Reminds me of the HIV days in the 1990s.
- Absolutely nothing.
- Being able to breathe with the masks and being very warm with all the PPE.
- Patients not being honest with their medical history.
- Not being allowed to use the ultrasonic due to aerosols.
- The large percentage of asymptomatic carriers.
- Not feeling air quality in office is good.
- There are many dentists that are not following the guidelines or being truthful to their patients. The doctor I was working for believes COVID is a political scam! A hygienist had COVID and then a front desk person had it within days. She was only out of work less than one week! She was not a mask wearer.
- Appointment scheduling. Practice universal precaution but when you aren’t scheduled with enough time per patient, you may get careless trying to stay on time putting yourself at risk.
- Coworkers not following COVID protocols.
- Patients not taking the pandemic seriously, not taking precautions, and coming into the office while they are infectious.
- Aerosols, sitting so close to the patient for close to an hour! Also, worried that mutations of the virus may make the vaccine ineffective.
- Lack of necessary appointment time in order to be thorough and sanitize properly between patients.
- The things we do not know about COVID transmission yet.
- Being exposed to 8-10 patients per day.
- Using the ultrasonic scaler, which is a necessary piece of equipment. Also, I have no faith in the ADA. It was obvious they put lobbying pressure on the CDC to force workers back, saying we could be safe. Of course, there was no way of knowing that.
- The front desk not correctly validating symptoms. “We wear masks, it’s OK” attitude from the doctor/owner/office manager. Not getting appropriate time off/pay if exposed or positive.
- I am immunocompromised and I worry about patients lying and front desk not screening properly.
- The state board recommended hygienists back to work, and we did not yet know enough about the long-term effects of the COVID virus.
- I do not feel comfortable around all the aerosols and do not want to wear all the extra PPE. It was already too hot and hard to breathe before the pandemic.
- Coworkers not following COVID-19 protocol (away from patients) such as not wearing a mask when not with a patient, in staff room, etc. Corrective action was not taken by employer after I brought this to the dentist’s attention, so I retired.
- Lack of access to vaccine, lack of safety measures.
- Coworkers who don’t do all they can to stay safe. My employer has gone above and beyond to create a safe environment while providing care to patients. So it’s not really those risks I worry most about.
- Exposure, bringing it home to family.
- Time allotment for hygienists is being double booked. I was not and would not allow it. Very sad at this occurrence.
- I would not be nervous because I practice as if everyone is infected with something. That’s how I was trained.
- Front desk was not screening appropriately and did not take it seriously. DDS did not want to reappoint and didn’t care. Wanted patients seen regardless. Tried to tell of concerns about front desk and nothing was done. So I left.