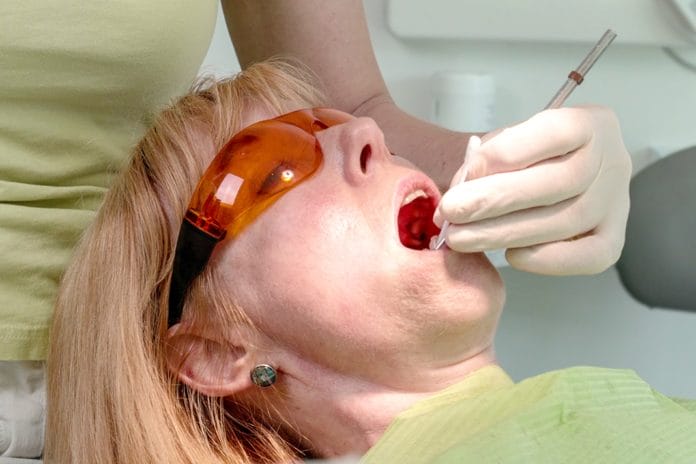
In our line of work, many dental hygiene patients present with varying levels of anxiety. While fears range from gagging to feeling pain during procedures, one of the most common fears seems to be injections.
Pain management is an important aspect of a successful dental appointment, but many patients tend to overlook the advantages of being anesthetized during treatment. As an extra step to ensure a painless experience, a topical gel is usually used before the injection. However, according to a study in The American Dental Society of Local Anesthesia, there is no significant evidence suggesting the decrease of pain when using a topical gel before an injection.1 Are we wasting our time by using a topical gel, or do patients actually benefit from it?
Two Minutes Lost?
When using a traditional benzocaine 20% topical gel, the effective application time is two minutes. While other topical options are available, such as a refrigerant spray with an impressive application time of five seconds, most clinicians stick to the familiar traditional gel.
If the proper guidelines are followed, the clinician must wait two minutes after applying the gel before giving the injection to assure the maximum effectiveness of the gel. If there is no significant benefit to the gel, however, the clinician just lost two minutes of working time, which we all know can be a big deal in dentistry.
If multiple injections are required for treatment, the working time for the clinician can potentially be decreased even more depending on if the injections are given at once or at different sequences during the appointment. Although a topical may not be necessary for proper treatment, I believe the extra time should still be taken to use it for the patient’s benefit.
How Patients Benefit
When my class learned how to administer the injections in hygiene school, I was one of those patients who feared the needle. Aside from having my wisdom teeth extracted, I hadn’t received any injections during dental treatment before. After my partner gave her first injection to me, however, I was thankful to know that I’m one of the lucky over-responders to local anesthesia. The traditional topical gel made me so numb that I never even felt the needle.
While the data in the above-mentioned study found no overall significant decrease in pain, I can vouch that some patients like me actually do benefit from the topical. While not all patients will notice a difference, the ones that respond well to the topical will be thankful that you used it.
Another reason to continue using the topical gel is to make patients believe that it prevents pain from the injection. Many studies have been conducted supporting both the power of positive thought and the placebo effect. Saying something like, “I’ll put this gel where the injection is going so that you won’t feel it,” allows the patient to think positively about the effectiveness of the gel, which actually makes it more effective from the patient’s perspective.
While not all patients will be numbed by the topical gel, it is still a good tool to use in pain management. If the only benefit is a placebo effect, patient comfort has still been prioritized. If a patient believes that the gel will make the injection more comfortable, they will be less anxious about being anesthetized, and both the patient and clinician will have a more pleasant experience.
When it comes to overall treatment time, doing product research can be important. If time is the main factor in cutting out a topical, using an accelerated agent can decrease the amount of potential time lost during application while still giving the patient optimum peace of mind. No matter what product is used, your patients will be thankful that you took the time (no matter how long or short) to use a topical to ensure their utmost comfort.
Before you leave, check out the Today’s RDH self-study CE courses. All courses are peer-reviewed and non-sponsored to focus solely on high-quality education. Click here now.
Listen to the Today’s RDH Dental Hygiene Podcast Below:
Reference
- DiMarco, A., Wetmore, A. (2016). Clinical comparison: fast-acting and traditional topical dental anesthetic. The American Dental Society of Local Anesthesia. 63: 55-61.