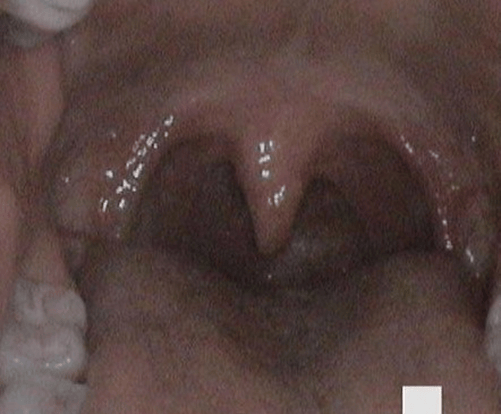
The uvula should not be neglected when evaluating the oral cavity for any discrepancies. The uvula is a fleshy, soft tissue in the middle of the soft palate that hangs down in the back of the throat in front of the tonsils, resembling an oval or teardrop shape (see Figure 1). The uvula’s flexibility prevents food and liquids from entering the nasal cavity, as well as a deterrent for food to go down the windpipe and directing it instead towards the esophagus.
The uvula is comprised of connective tissue, saliva glands, and muscle tissue.1 The serous glands release thin saliva to keep the throat lubricated. The uvula is composed of muscular fibers completely surrounded by mucosa. The muscular fibers are part voluntary and involuntary and derived from cross fibers of the soft palate. The muscular tissue contains an abundance of blood vessels. The muscular portion shortens and broadens the uvula to contribute to closing the nasopharynx during swallowing.2
Speech − A function of the uvula is speech, helping with the consonant sounds (particularly in certain languages such as French, Arabic, and Hebrew).
Velopharyngeal insufficiency is when the uvula doesn’t close against the rear of the throat. This causes extra air through the nose making speech sound more nasal. It also enables the vibrato sound for singers.3
Gag reflex − The uvula is part of the gag reflex. A gag reflex is an action when the muscles of the throat contract by being triggered with something touching the back of the throat. When the area of the soft palate is touched, it may induce a gagging sensation and even vomiting.3
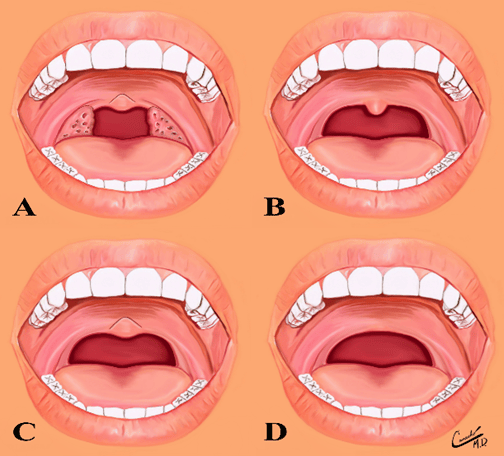
Bifid uvula − A bifid uvula is a split uvula. This occurs during development in the womb and undergoes partial or incomplete fusion, resulting in forked tips. It is more commonly seen in children.
A bifid uvula is associated with a submucous cleft palate that is commonly related to a cleft palate or lip. It contains less muscle than a normal uvula. This could be problematic (or not). If so, impaired speech or food or liquids can move into the nasal cavity causing regurgitation. Since it is a genetic disorder, other issues may be present such as middle ear infections or abdominal aortic aneurysm.4
Uvular elongation − Elongation of the uvula is also a developmental variant. The growth is longer than normal. This condition may be notable if the patient experiences irritation, cough, vomiting, dysphagia, and sleep apnea. Removal of the uvular may be recommended if it interferes with daily activities.5
Hereditary angioedema − Hereditary angioedema is a rare disorder inherited by one or both parents. This condition causes swelling under the skin and lining of the gut and lungs and causes fluid to collect around the blood vessels and blocks the flow of lymph fluid in the body. With this issue, other parts of the body also swell, including the hands, feet, eyelids, lips, face, uvula, and airway.
In rare cases, it can become so severe that the airway can be compromised due to the extent of closure. While there’s no cure, medications can help prevent attacks.6,7
Quincke’s disease is angioedema in the upper airway and maybe local just to the uvula (see Figure 2). Spontaneous swelling is typically caused by an immediate type I hypersensitivity reaction. Other causes are trauma, thermal injury, and infections.
Marijuana usage may become a rare, yet life-threatening complication, with localized swelling of the deeper layers of the skin and fatty tissues beneath the skin. Marijuana use, burning at higher temperatures than tobacco, can be more irritating to the mucous membranes, causing blockage and closure of the airway.8
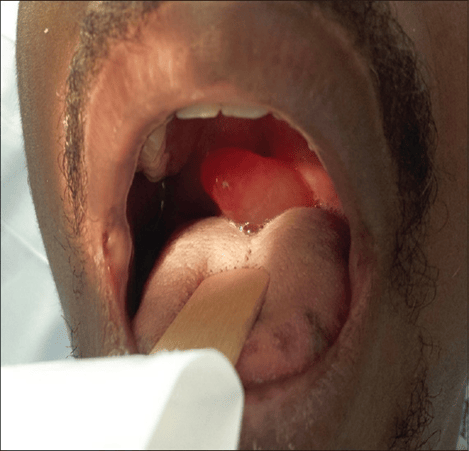
Image courtesy: Mohammadi, L., Miller, A., Ashurst, J.V. Quincke’s Disease. J Family Med Prim Care. 2016; 5: 677-9.
Piercing − A pierced uvula is a form of body modification. It is rarely seen due to the gagging reflex and challenges of applying it to the uvula, possibly taking several attempts to complete. Piercings are usually horizontal, although they could be from front to back.
During the piercing process, the uvula can easily be crushed, resulting in swelling and infection. The weight of the piercing may pull the uvula down into the throat, reducing the airway. Other concerns are biofilm accumulation around the jewelry, accidental inhaling or swallowing if dislodged, and the jewelry rubbing on the back of the throat.9
Uvulitis − Uvulitis is a red, sore, and inflamed uvula. The causes are bacterial and viral infections, along with genetics, allergies, injury, acid reflux, dry mouth, smoking, and alcohol consumption.
The symptoms are difficulty in swallowing, a sensation of something stuck in the throat, sore throat, vocal changes, swollen tonsils, excessive saliva, gagging, pain, and fever.9
Snoring − The uvula vibrates when sleeping, causing vibration in the upper airways while breathing. The noise is caused by a flabby, fleshy, or longer uvula that causes heavy vibrations during sleep, inducing the snoring sounds. This repetitive vibration could cause vibratory trauma (the vibration over time could cause the uvula to lengthen and widen to promote more snoring sounds).10
Sleep apnea − Obstructive sleep apnea occurs when the airway is covered and blocks airflow into the lungs. This is common with an enlarged or elongated uvula. Generally, if it disrupts sleep and breathing during the night, the removal of the uvula is recommended.1
Cancer − Cancer of the uvula is rare. If it happens, the most common forms are papillomas that are a result of a viral infection, namely HPV-6 and HPV- 11. It is very rare for uvula cancer to be a carcinoma; but if it is, it’s usually very aggressive. The uvula will have a fibrous cancerous protrusion, which may cause elongation or a choking and gagging feeling. The resolution is the removal of the uvula.5
Uvular necrosis − Uvular necrosis is when it becomes light-colored or whitened. The portion that becomes light may fall eventually fall off. Reasons that may cause this is impingement with devices and suctioning.12
Uvula Surgeries
Uvulectomy is the removal of the uvula. It is recommended if it has growths, papillomas, cysts, cancer, or interferes with breathing or sleeping such as snoring and obstructive sleep apnea. If the uvula is longer than 1.5 centimeters, it may be recommended to reduce the size.
There is partial and complete uvulectomy, and, within those procedures, there are stages. The removal of the uvula may be dependent on the reason for removal. If there’s snoring correlated with sleep apnea, partial removal may be suggested. If obstructive sleep apnea is uvula related, complete removal may be suggested.
The different stages of removal are:
- Low: Very little of the uvula is removed
- Middle: Half the uvula is removed
- High: The whole uvula is removed
The temporary side effects of removing the whole uvula are difficulty in swallowing and breathing, throat dryness, a feeling of a lump in the throat, halitosis, fever, earache, and voice changes.11 These symptoms may last a few days or a few weeks.
Uvulopalatopharyngoplasty (UPPP) may be an option for shrinking the palate and clearing the blockage of the throat for isolated obstructive sleep apnea (see Figure 3). The UPPP procedure removes excess tissue from the soft palate and pharynx.
In more serious cases, the tonsils and adenoids may also be removed. It is the most common procedure for isolated obstructive sleep apnea, meaning that only the uvula and no other issues cause sleep apnea. The UPPP procedure is more successful in patients who are not obese.1
An uvulopalatal flap shortens the uvula by folding the distal palate with the uvula forward upon itself (see figure 4). The procedure folds and sutures the uvula to the soft palate. It’s commonly used for elongated or enlarged uvulas. The uvulopalatal flap preserves the uvula muscle as it’s repositioned and stabilized anteriorly. This procedure could be reversed or adjusted.
The uvulopalatal flap is mainly used to relieve snoring. With other procedures, uvula removal is permanent since the uvula is a muscle that does not grow back after surgery.12,13
The uvula is generally not problematic, but it is greatly overlooked. Many times, it’s hard to even see it at the back of the throat, depending on a dental patient’s mouth. If any concerns from the patient are noted with the throat area, it could be the throat or tonsils, but the uvula shouldn’t be ruled out.
Before you leave, check out the Today’s RDH self-study CE courses. All courses are peer-reviewed and non-sponsored to focus solely on high-quality education. Click here now.
Listen to the Today’s RDH Dental Hygiene Podcast Below:
References
- Watson, S. Uvula Removal Surgery. September 27, 2018. Retrieved from https://www.healthline.com/health/uvula-removal#purpose.
- Hays, H. Circumcision of the Uvula. The Laryngoscope. 1912; 22(7): 965-969. Retrieved from https://onlinelibrary.wiley.com/doi/abs/10.1288/00005537-191207000-00009
- Medic8. Retrieved from https://www.medic8.com/healthguide/sore-throat/uvula.html
- Bifid Uvula. Healthy Hearty. Retrieved from https://healthhearty.com/bifid-uvula
- Disease Presentations of the Uvula. Relias Media. July 13, 2014. Retrieved from https://www.reliasmedia.com/articles/16933-disease-presentations-of-the-uvula
- What Causes a Swollen Uvula? Retrieved from https://www.webmd.com/oral-health/causes-swollen-uvula#3-6
- S. Hereditary Angioedema Association. Retrieved from https://www.haea.org/page/disease
- Mohammadi, L., Miller, A., Ashurst, J.V. Quincke’s Disease. J Family Med Prim Care. 2016; 5: 677-9. Retrieved from http://www.jfmpc.com/article.asp?issn=2249-4863;year=2016;volume=5;issue=3;spage=677;epage=679;aulast=Mohammadi;type=0
- Higuera, V. What causes a swollen uvula? Medical News Today. January 12, 2020. Retrieved from https://www.medicalnewstoday.com/articles/315997#Causes
- Enoz, M. Elongated (Long) Uvula Causes, Symptoms, and Treatment. Retrieved from https://www.ent-istanbul.com/2019/07/elongated-long-uvula-causes-symptoms.html
- Hayes, K. Reasons for Performing Uvulectomy. Very Well. Retrieved from https://www.verywellhealth.com/what-is-a-uvulectomy-1192058 W
- Camacho, M. Surgeries. TV Uvula Surgery: Illustrations and What You Need to Know. Retrieved from https://surgeries.tv/uvula-surgery/
- Huntley, T.C. The Uvulopalatal Flap. 2015. Retrieved from https://clinicalgate.com/the-uvulopalatal-flap/