Dental health professionals are aware of the connection between oral manifestations and systemic disease. We are well versed in having a conversation regarding the connection between periodontal disease and systemic diseases such as cardiovascular disease, type 2 diabetes, and Alzheimer’s disease.
However, there is a condition seen in the dental chair that many dental hygienists may not associate with systemic disease. The oral-systemic connection that will be the focus of this article is tooth agenesis/hypodontia and cancer.
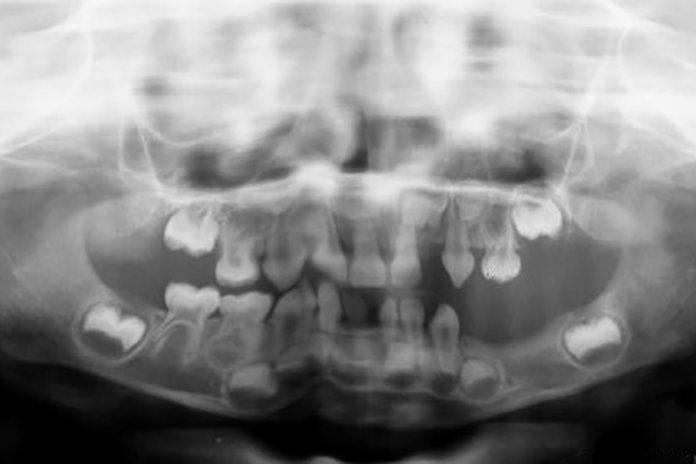
If you recall from histology and embryology, tooth development is a complex process. It involves many regulatory proteins, pathways, and signaling networks. It is impressive how well this process works and how rarely it has a glitch. The reported incidence of tooth agenesis is between 3% to 10%. Although it is the most common developmental dental anomaly, it is still quite rare in the population. Though many people may not see the connection between odontogenesis and tumorigenesis, research has highlighted a connection in the molecular pathways of the two.1
Colorectal Cancer
Several genes have been studied, and mutations in these genes are linked to tooth agenesis. One of these genes, AXIN2, is the common link between tooth agenesis and colorectal cancer.2 A study conducted on a multigeneration Finnish family with a history of tooth agenesis (out of 19 family members, 11 were missing eight permanent teeth, and two of them had only three permanent teeth develop) showed a significant association between tooth agenesis and a family history of cancer. The results indicate a 2.71 times higher incidence of a family history of cancer and tooth agenesis.3
Further studies using genetic analysis support the hypothesis of a genetic link between tooth agenesis and colorectal cancer. The studies showed an increased incidence of colorectal cancer in patients with tooth agenesis, and the genetic link manifests strongly in first-degree relatives.4
Though more research is warranted, this may be yet another screening seen in dental offices. The five-year survival rate of colorectal cancer ranges between 67% to 89%. Early detection through noninvasive screenings may be a key factor in keeping the survival rate high, as early detection increases the five-year survival rate.5 Until further research is available, advising patients of the possible connection between tooth agenesis and colorectal cancer may benefit them by encouraging early screenings or possibly discussing genetic testing to identify markers that would increase their risk of developing colorectal cancer.
Epithelial Ovarian Cancer
Epithelial ovarian cancer is the fifth most common cancer in women with an 18-month prognosis and a 40 to 50% overall survival rate at 10 years; this form of cancer demands attention and research to improve prognosis. The research to date has brought us to look closely at the association of epithelial ovarian cancer (EOC) and tooth agenesis.4
Again, a mutation in AXIN2 seems to be the possible link between tooth agenesis and EOC, though other gene mutations are certainly being investigated as well. The evidence leaves a bit to be desired and needs further research. However, the studies available have shown an association between tooth agenesis and EOC. In a self-reported study, the authors found an eight times higher incidence of tooth agenesis in women diagnosed with EOC.6 A follow-up study published in 2014 supported the previous findings with the results showing a three-fold higher incidence of EOC in women with tooth agenesis, although neither of these studies included genetic testing.7
I encourage all dental professionals to be on the lookout for future studies that may clarify the pathway and identify a causal link.
Multiple Cancers
A study published in 2013 looked at the association between tooth agenesis and multiple cancers. The results indicated that breast cancer was the most reported cancer among the participants, followed by prostate cancer in individuals both with and without tooth agenesis. Participants with tooth agenesis had an increased risk of having a family history of female-specific cancers, including breast, ovarian, cervical, and uterine cancer.
The authors’ conclusion indicates their findings show an increased frequency of almost all tumor types in families with a history of tooth agenesis. The highest risk was associated with the brain/nervous system and prostate and breast cancers. A slightly increased risk was associated with lung and intestine/colon cancers, while a reduced risk was associated with head/neck, liver, and stomach cancers. The evidence of reduced risk associated with head/neck, liver, and stomach cancer may suggest these types of cancers do not share the same genetic contributors. This study further supports the hypothesis of an association between tooth agenesis and cancer.8
Clinical Relevance
Though further studies are needed to determine causality and identify the mechanism by which tooth agenesis and cancer development are connected, the research available is substantial enough to start the conversation with patients regarding the possible increased risk of cancer development associated with tooth agenesis. This may be in the form of encouraging early screenings for colorectal, prostate, and most female-specific cancers. If the patient is a child, making the parents aware of the connection may be helpful in that the parent will hopefully encourage their child to get early screening as they become adults. Screenings for children have not been advised since most cancers develop in adulthood.
Early detection is the key to a better quality of life and increased survival rates among those that develop cancer. This is also an area of research dental professionals should be aware of and follow for future research that may clarify our role in the screening process. Genetic tests identify markers such as AXIN2 in both blood tests and salivary tests. This may be an option for patients in the future that present with tooth agenesis—one more step in bridging the gap between medicine and dentistry.
Need CE? Click Here to Check Out the Self-Study CE Courses from Today’s RDH!
Listen to the Today’s RDH Dental Hygiene Podcast Below:
References
- Ritwik, P., Patterson, K.K. Diagnosis of Tooth Agenesis in Childhood and Risk for Neoplasms in Adulthood. Ochsner J. 2018; 18(4): 345-350. doi:10.31486/toj.18.0060. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6292463/
- Callahan, N., Modesto, A., Meira, R., Seymen, F., Patir, A., Vieira, A.R. Axis Inhibition Protein 2 (AXIN2) Polymorphisms and Tooth Agenesis. Arch Oral Biol. 2009; 54(1): 45-49. doi:10.1016/j.archoralbio.2008.08.002. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2643013/
- Lammi, L., Arte, S., Somer, M., et al. Mutations in AXIN2 Cause Familial Tooth Agenesis and Predispose to Colorectal Cancer. Am J Hum Genet. 2004; 74(5): 1043-1050. doi:10.1086/386293. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1181967/
- Medina, M.C.G., Bastos, R.T.D.R.M., Mecenas, P., Pinheiro, J.J.V., Normando, D. Association between Tooth Agenesis and Cancer: A Systematic Review. J Appl Oral Sci. 2021;29:e20200955. Published 2021 Aug 9. doi:10.1590/1678-7757-2020-0955. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8360625/
- Survival Rates for Colorectal Cancer. (2021, January 29). American Cancer Society. Retrieved from https://www.cancer.org/cancer/colon-rectal-cancer/detection-diagnosis-staging/survival-rates.html
- Chalothorn, L.A., Beeman, C.S., Ebersole, J.L., Kluemper, G.T., Hicks, E.P., Kryscio, R.J., DeSimone, C.P., Modesitt, S.C. Hypodontia as a risk marker for epithelial ovarian cancer: a case-controlled study. Journal of the American Dental Association (1939). 2008; 139(2): 163–169. Retrieved from https://pubmed.ncbi.nlm.nih.gov/18245684/
- Fekonja, A., Čretnik, A., Takač, I. Hypodontia Prevalence and Pattern in Women with Epithelial Ovarian Cancer. The Angle orthodontist. 2014; 84(5): 810–814. https://doi.org/10.2319/112813-876.1. Retrieved from https://pubmed.ncbi.nlm.nih.gov/24689849/
- Küchler, E.C., Lips, A., Tannure, P.N., Ho, B., Costa, M.C., Granjeiro, J.M., Vieira, A.R. (2013). Tooth Agenesis Association with Self-reported Family History of Cancer. Journal of Dental Research. 2013; 92(2): 149–155. https://doi.org/10.1177/0022034512468750. Retrieved from https://pubmed.ncbi.nlm.nih.gov/23169889/