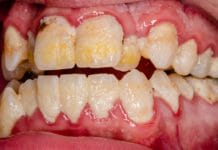
Malocclusion is defined as “irregular contact of opposing teeth in the upper and lower jaws.”1 Most people with minimal knowledge of dentistry view it as an esthetic problem and not an oral health problem. Not only are there oral health implications, but general health can be affected too. It is estimated that about 65% of the U.S. population has some degree of malocclusion.
Some of the general health problems affected by malocclusion include airway obstructions, sleep apnea, gastric disturbance, immune deficiencies, and delayed developmental growth.2
Dr. Edward Angle is regarded as “the father of American orthodontics,” and he developed a classification system for malocclusion in 1899. This is the same malocclusion system we use today in dentistry. The classification is based on molar position and is an important tool in the diagnosis and treatment of malocclusion.2
The etiology of malocclusion is attributed to heredity in most cases. However, overbite and overjet are less likely to be attributed to heredity, which leaves the possibility of environmental factors as the cause.3
Orthodontic treatment has evolved and is readily available to most individuals. Helping patients understand the oral health and general health implications of malocclusion may assist in the decision to have treatment. I would like to review some research that can be shared with patients in this regard.
Periodontal Disease
Periodontal disease is known to be caused by certain bacteria in biofilm, but this should not be considered the only etiology. Biomechanical misfunction, a fancy way to describe malocclusion, has also been shown to be a contributing factor. Malocclusion can cause an overload on certain teeth, causing an inflammatory response. If left untreated, the inflammatory response will cause progressive atrophy to the bone.4
A 35-year longitudinal study published in American Journal of Orthodontics and Dentofacial Orthopedics concluded, “Certain incisor malalignment traits (i.e., maxillary incisor crowding, maxillary incisor spacing, mandibular incisor mild crowding, mandibular incisor moderate-to-severe crowding, mandibular incisor moderate irregularity, and mandibular incisor severe irregularity) are associated with significant periodontal disease progression.”5
Malocclusion should be considered when treating periodontal disease. If left untreated, malocclusion can contribute to relapse in periodontal disease and should be discussed with the patient.
Sleep Apnea
Although the research on the relationship between malocclusion and sleep apnea in adults seems to be ongoing (along with some contradictory conclusions), the relationship between malocclusion and sleep apnea in children is much clearer. It has been shown with great certainty that posterior crossbite, overjet, and overbite in children has a significant correlation with obstructive sleep apnea.7
The research that concludes there is a relationship between malocclusion and sleep apnea in adults states, “Overjet was also found to be associated with the severity of obstructive sleep apnea syndrome in nonobese patients, and this leads the researcher to suggest that malocclusion may play an important role in the development of sleep apnea/hypopnea.”8 More research is needed to clarify this association.
Gastric Disturbance
Several studies have linked malocclusion with delayed gastric emptying. This is caused by the decreased masticatory function that malocclusion presents. Symptoms of delayed gastric emptying can range from heartburn, indigestion, vomiting, bloat, and feeling full quickly when eating.9
A pilot study published just last year followed seven women from pre-treatment to post-treatment with orthodontics and assessed any improvement in gastric disturbances. The researchers concluded, “We provide evidence of improvement of masticatory function after orthodontic treatment, which was associated with a faster rate of gastric emptying.”10
Vision Problems
Studies have found a correlation between malocclusion and myopia (nearsightedness) in pediatric patients. Higher prevalence of myopia was found in children with class II division 1 malocclusion. It is hypothesized that “skeletal pattern may attribute to altered development of the structures linked with the vision.”
It is important to mention this is just a correlation; further studies are needed to assess the mechanism by which malocclusion contributes to myopia if there is indeed one.11, 12
Speech
Malocclusion has been associated with speech errors. The severity of malocclusion is directly related to the severity of speech sound errors.
Data from a study of 150 subjects age range of 8 years to 36 years found that an open bite was the trait most likely to cause speech sound errors. Second to open bite, bilateral posterior cross-bite showed negative effects on speech sound production.13
Dental Caries
Dental caries is one of the most commonly seen infectious diseases. Dental caries has been shown to be a complication of malocclusion due to the difficulty of achieving proper oral hygiene.
However, the risk of caries as a complication of malocclusion has been determined to be quite small. This alone may not be a big concern for the clinician or patient. If a clinician sees an increase in caries risk, reviewing proper and/or alternative oral hygiene methods may be all that is needed to reduce the slight, increased risk of dental caries associated with malocclusion.6
Quality of Life
In a systemic review of 22 quantitative studies, strong evidence showed malocclusion has a negative effect on quality of life. This was particularly evident in the areas of social and emotional wellbeing.14 This kind of negative feelings can lead to exclusion from activities and play a role in self-esteem and overall mental health. This is particularly true for children and adolescents.
As clinicians, it is our job to help patients and parents understand the multifaceted role malocclusion plays in oral, physical, and mental health. With the recent explosion of mail order clear aligners, we must also discuss the importance of good quality orthodontic care when addressing malocclusion. Orthodontic treatment by a qualified provider can change lives in more way than one.
I have never in my career had a patient regret having orthodontic treatment to address malocclusion. Helping patients value the treatment is the most important step in the journey to improving their smile, oral health, physical health, and quality of life.
Resources
- Dictionary.com. Retrieved from https://www.dictionary.com/browse/malocclusion
- Joshi, N., Hamdan, A.M., Fakhouri, W.D. Skeletal Malocclusion: A Developmental Disorder with a Life-long Morbidity. J Clin Med Res. 2014 Dec; 6(6): 399-408. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4169080/
- Moreno Uribe, L.M., Miller, S.F. Genetics of the Dentofacial Variation in Human Malocclusion. Orthod Craniofac Res. 2015 Apr; 18(0 1): 91-99. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4418210/
- Meynardi, F., Lauritano, D., Pasqualini, M., et al. The importance of occlusal trauma in the primary etiology of periodontal disease. Journal of Biological Regulators and Homeostatic Agents. 2018 Mar; 32(2 Suppl 1): 27-34. Retrieved from https://www.researchgate.net/publication/323318336_The_importance_of_occlusal_trauma_in_the_primary_etiology_of_periodontal_disease
- Alsulaiman, A.A., Kaye, E., Jones, J. Cabral, H., Leone, C., Will, L., Garcia, R. Incisor Malalignment and the Risk of Periodontal Disease Progression. Am J Orthod Dentofacial Orthop. 2018 Apr; 153(4): 512-522. Retrieved from https://www.ncbi.nlm.nih.gov/pubmed/29602343
- Brignardello-Peterson, R. Evidence Suggests a Small Association Between Malocclusion and Caries in Adolescents. The Journal of the American Dental Association. 2018 Nov; 149(11): e150. Retrieved from https://jada.ada.org/article/S0002-8177(18)30348-9/abstract
- Galeotti, A., Festa, P., Viarani, V., D’Anto, V., Sitzia, E., Piga, S., Pavone, M. Prevalence of Malocclusion in Children with Obstructive Sleep Apnea. Orthod Craniofac Res. 2018 Nov; 21(4): 242-247. Retrieved from https://www.ncbi.nlm.nih.gov/pubmed/30188002
- Banabilh, S.M. Orthodontic View in the Diagnosis of Obstructive Sleep Apnea. J. Orthod Sci. 2017 Jul-Sep; 6(3): 81-85. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5508407/
- Koike, S., Sujino, T., Ohmori, H., Shimazaki, K., Fukuyama, E., Kanai, T., Hibi, T., Ono, T. Gastric Emptying Rate in Subjects with Malocclusion Examined by [(13)C] Breath Test. J Oral Rehabil. 2013 Aug; 40(8): 574-81. Retrieved from https://www.ncbi.nlm.nih.gov/pubmed/23675963
- Suzuki, J., Shimazaki, K., Koike, S., Ono, T. Gastric Emptying Rate Before and After orthodontic Treatment Examined with the [13C] Breath Test: A Pilot Study. Am J Orthod Dentofacial Orthop. 2018 Mar; 153(3):347-354. Retrieved from https://www.ncbi.nlm.nih.gov/pubmed/29501109
- Monaco, A., Sgolastra, F., Cattaneo, R., Petrucci, A., Marci, M.C., D’Andrea, P.D., Gatto, R. Prevalence of Myopia in a Population with Malocclusion. Eur J Paediatr Dent. 2012 Oct; 13(3 Suppl): 256-8. Retrieved from https://www.ncbi.nlm.nih.gov/pubmed/23046255
- Amitha, M., Hedge, Y. Shetty, R., Kar, A. Prevalence of Vision Defects inn a School Based Population with Malocclusion. Int J Dent Med Res. 2015 Jan-Feb; 1(5): 53-55. Retrieved from http://www.ijohmr.com/upload/Prevalence%20of%20Vision%20Defects%20in%20a%20School%20Based%20Population%20with%20Malocclusion.pdf
- Leavy, K.M., Cisneros, G.J., LeBlanc, E.M. Malocclusion and its Relationship to Speech Sound Production; Redefining the Effect of Malocclusion Traits on Sound Production. Am J Orthod Dentofacial Orthop. 2016 Jul; 150(1): 116-23. Retrieved from https://www.ncbi.nlm.nih.gov/pubmed/27364213
- Dimberg, L., Arnrup, K., Bondemark, L. The Impact of Malocclusion on the Quality of Life among Children and Adolescents: A Systemic Review of Quantitative Studies. Eur J Orthod. 2015 Jun; 37(3): 238-47. Retrieved from https://academic.oup.com/ejo/article/37/3/238/2756146