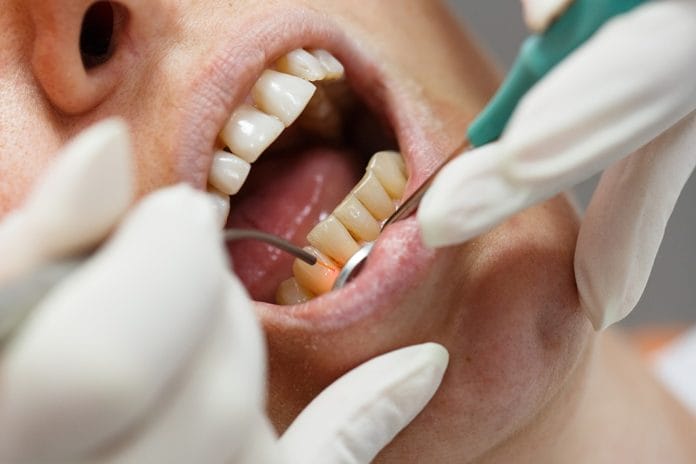
Does your state allow hygienists to use laser as an adjunct to dental treatment? If yes, are you laser certified? If you have access to a laser, look up a class, and get certified! Not only is learning something new super fun, but the laser is also beneficial and straightforward to use.
For many, lasers seem daunting and slightly scary, similar to that very first anesthetic injection. After a couple of patients, though, you will love it! Here are some observations about laser usage in the hygiene operatory.
Mobility − Once you are certified and have access to a laser, make sure it is ready − at hand. The worst part is the setup if you need to leave the room to gather supplies. I have found a small cart on wheels that holds the laser and all supplies, including laser protective glasses, the laser warning signage, and post-operative instructions. In a perfect world, it would always be available, but as many hygienists travel to different operatories, it may not always be so simple.
Time management − At the beginning, discuss a fee for the laser bacterial reduction (LBR) procedure that can be used as an addition to each hygiene appointment. LBR adds about five minutes to each appointment, so be prepared for some additional time management. On the bright side, LBR is completely comfortable and requires no anesthetic.
Excellent verbal skills are going to be required for explaining the treatment procedure and benefits, as well as the fee. The cost of the laser itself is high, and the disposable tips, if used, are costly too. The course fee and time for implementation chairside must also be included in patient cost.
We always tell patients that insurance will not cover laser treatments, so there is no expectation of reimbursement. We do include the laser treatment on any insurance filed in hopes of payment, but it is rarely reimbursed as either bacterial reduction or periodontal pocket therapy. The benefit of treatment with the laser outweighs the additional fee, and the ease of its use makes for a very successful treatment adjunct.
Patients are instructed to return about six weeks later for full periodontal probing. Some computer systems will allow you to print the before and after depths to show the patient the areas of improvement and any remaining areas that may need re-treatment and improved home care. The probing before and after sheet is working well as an increased motivational tool and to add value for the laser service. Most patients are enjoying the newer technology and the procedure overall.
Health benefits − The LBR procedure is noninvasive and painless. Reducing the number of bacteria in the pocket increases healing and reduces the strain on the immune system. Even healthy mouths may have some bleeding during routine preventive care; the use of LBR reduces the possibility of infection and irritation while giving all patients a head start on the journey to improved home care.
As a clinician, the greatest achievement is that, after thorough debridement, the laser removes the diseased tissue and pocket lining leaving this wonderful, healthy tissue to heal beautifully. So far, I personally am seeing amazing results of 2 mm average pocket reduction and tissue that is more toned, stippled, and improved color with significantly less bleeding.
Pain control − When using the laser for periodontal pocket reduction, the patient must be anesthetized to make the procedure completely comfortable. Some clinicians will use topical applications while others choose anesthetic injections. Just be aware of how your patient is feeling as some may already be slightly turned off by the unique smell of the laser tip being activated and the scent of the tissue as it is heated and removed from the pocket.
Patients are reporting minimal post-operative discomfort. For some, not smoking immediately afterward is challenging.
Some follow-up instructions include:
“Rinse with warm salt water. One teaspoon of salt mixed with eight ounces of warm water. You may brush gently tonight. No flossing (string floss, floss aids, interdental brush, etc.) for three days.
“Discomfort. On the rare occasion that you have discomfort, ibuprofen, or Tylenol is usually sufficient in helping.
“Eating. Eat a softer diet to allow for maximum healing. Avoid hard, crunchy foods like chips and popcorn for three days.
“Smoking. Smoking is an irritant to any healing and should be avoided as much as possible for three days after treatment.”