Are you in need of CE credits? If so, check out our peer-reviewed, self-study CE courses here.
Test Your Dry Socket Knowledge
1. What is another name for dry socket?
Alveolar osteitis, commonly called dry socket, is one of the most common complications after tooth extraction. Most studies report it affects between 0.5% to 5% of patients, but some studies have reported rates as high as 68%.1
Dry socket causes ongoing moderate to severe pain at the extraction site and often leads to multiple follow-up visits for pain relief and management.1
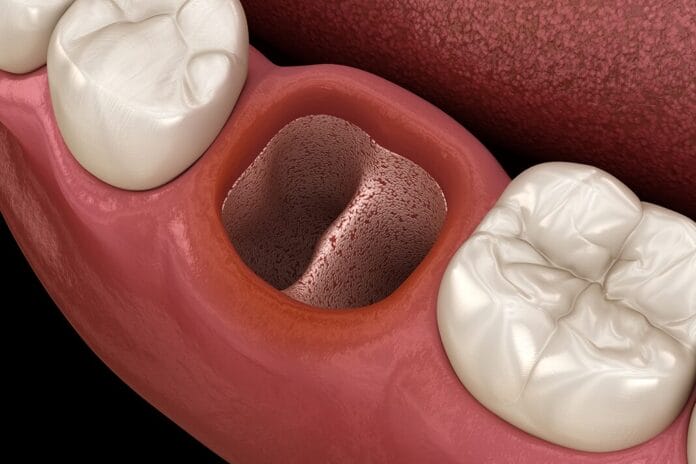
The most widely accepted explanation for dry socket is the fibrinolytic theory. Normally, a blood clot forms in the socket, serving as a scaffold for healing. In a dry socket, this clot does not form or is lost, leaving the bone exposed and causing pain.1
While the fibrinolytic theory is the leading explanation, its exact cause remains under debate. Because of this, many methods have been proposed to prevent and treat it, but there is no clear, evidence-based consensus on the best approach.1
Reference
1. Rohe, C., Schlam, M. (2023, May 29). Alveolar Osteitis. StatPearls. https://www.ncbi.nlm.nih.gov/books/NBK582137/
2. Dry socket is considered a true infection because bacteria break down the blood clot and produce classic signs of infection, such as edema, purulence, and erythema.
Bacteria may influence the development of dry socket. Studies show that people with dry socket have a significantly different microbiota than those who present without postoperative complications. Certain bacteria, such as Prevotella, Fusobacterium, Parvimonas, and Peptostreptococcus, were the most common among patients with dry socket, while Treponema denticola has also been identified as a likely culprit.1
In order for bacteria to be a causative agent, they must be capable of fibrinolysis (breaking down blood clots) but not cause typical signs of infection, such as edema, purulence, or erythema. These bacteria thrive in conditions of poor oral hygiene and remain on the surface of the bone. Because of this, dry socket is not considered a true infection, even though bacteria may contribute to its development.1
Reference
1. Rohe, C., Schlam, M. (2023, May 29). Alveolar Osteitis. StatPearls. https://www.ncbi.nlm.nih.gov/books/NBK582137/
3. Dry socket occurs much more frequently after mandibular third molar extraction than after any other tooth extraction. This is due to the lack of blood flow to mandibular molars.
Mandibular third molar extractions have a significantly higher risk of dry socket than all other sites combined, with an incidence rate of about 30%. Because mandibular molars have greater vascularity than anterior teeth, this challenges the belief that dry socket is caused by a lack of blood flow – a hypothesis often used to explain why it is less common in the maxilla.1
Reference
1. Rohe, C., Schlam, M. (2023, May 29). Alveolar Osteitis. StatPearls. https://www.ncbi.nlm.nih.gov/books/NBK582137/
4. Which of the following increases the risk of dry socket?
Research shows that women who take oral contraceptives or have extractions mid-menstrual cycle are at higher risk of developing dry socket. This is likely because hormonal changes contribute to increased levels of plasminogen and decreased levels of plasminogen activator inhibitor, which increase fibrinolysis. This supports the fibrinolytic theory that dry socket is caused by early clot loss.1
Other documented factors that may raise the risk include tobacco use, poor oral hygiene, difficult extractions, surgical technique, and clinician experience. While multiple studies support these factors, evidence for other proposed risks has not been demonstrated.1
Reference
1. Rohe, C., Schlam, M. (2023, May 29). Alveolar Osteitis. StatPearls. https://www.ncbi.nlm.nih.gov/books/NBK582137/
5. Dry socket is characterized by localized pain that begins immediately after tooth extraction, often accompanied by halitosis.
The main symptom of dry socket is increasing pain at or near the tooth extraction site, beginning one to five days after extraction. Because the pain follows the path of the trigeminal nerve, it often radiates from the socket to other areas of the head and neck. This pain typically does not improve with pain medication, and patients commonly report halitosis.1
On examination, the area often looks mostly normal. Some erythema and edema are expected after surgery, but there are no clear signs of infection. Occasionally, patients may have a mild fever or enlarged lymph nodes, but this is uncommon.1
The combination of severe pain and the total or partial absence of a blood clot is sufficient to diagnose dry socket, but it can be difficult to visualize. Blood tests are not needed because dry socket is a healing problem, not an infection, and therefore does not cause elevated white blood cell counts. While radiographs are not necessary to diagnose dry socket, they are sometimes used to rule out other concerns, such as retained root fragments.1
Reference
1. Rohe, C., Schlam, M. (2023, May 29). Alveolar Osteitis. StatPearls. https://www.ncbi.nlm.nih.gov/books/NBK582137/
6. The primary differential diagnosis for dry socket is infection. Ongoing or late-onset pain may indicate osteomyelitis.
Some sources claim that pain lasting more than one week is less typical of dry socket, and that pain that persists beyond three weeks suggests a different diagnosis.1
The primary differential diagnosis to consider is infection, particularly if symptoms spread beyond the socket or involve signs of disease elsewhere in the jaw. Ongoing or late-appearing pain may indicate acute osteomyelitis, subperiosteal (occurring between the bone and periosteum) infection, or sequestra (dead bone). In these cases, a panoramic radiograph may be needed to evaluate healing.1
Dry socket is a self-limiting condition that resolves on its own. The outlook is excellent, and symptoms usually improve within a few days of treatment. Even without treatment, dry socket does not cause long-term damage.1
Reference
1. Rohe, C., Schlam, M. (2023, May 29). Alveolar Osteitis. StatPearls. https://www.ncbi.nlm.nih.gov/books/NBK582137/
7. Which of the following is the most widely supported first step in the treatment of dry socket?
The most widely supported first step in treatment is gentle irrigation of the extraction socket. This helps remove necrotic tissue and clot debris, which reduces the bacterial load. Irrigation alone may not fully relieve pain, but it is an important starting step and can be supplemented with other strategies. Topical anesthetic gels and long-acting local anesthetics can be utilized for immediate pain relief, while non-steroidal anti-inflammatory drugs (NSAIDs) may be used to supplement local anesthetics for further improved pain relief. Unlike irrigation, curettage is not recommended, as it can further expose the bone and potentially worsen symptoms.1
Hyaluronic acid administration after irrigation has also been shown to reduce pain and inflammation. Other treatments involve placing medicated dressings into the socket, such as zinc oxide-eugenol or other obtudent (soothing) materials with pain-relieving or antibacterial properties. While many studies show these can help reduce pain, they often need to be removed to avoid irritation and may slow down healing.1
Chlorhexidine rinses or gels have been studied for both prevention and treatment. While chlorhexidine is effective at preventing dry socket, there is currently not enough evidence to recommend it for treating a dry socket that has already formed.1
Platelet-rich fibrin (PRF) has also been studied. It may improve soft-tissue healing, but it does not reduce pain more effectively than irrigation alone, and its value as a treatment remains uncertain. Generally, PRF is utilized for prevention rather than treatment.1
Reference
1. Rohe, C., Schlam, M. (2023, May 29). Alveolar Osteitis. StatPearls. https://www.ncbi.nlm.nih.gov/books/NBK582137/