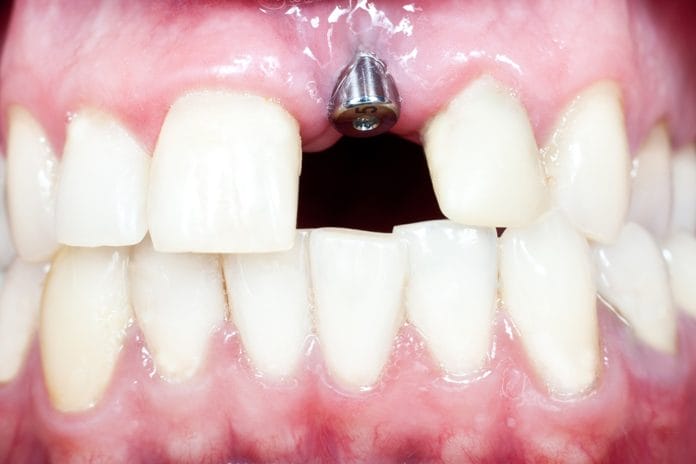
The number of implants placed by dentists and dental specialists is increasing based on a predictable outcome of success. A comprehensive treatment plan includes advising the patient of the risk of failure based on smoking, history of radiotherapy, systemic health issues, and local bone quality and quantity. Peri-implant disease is a combination of poor oral hygiene, placement of a non-cleansable prosthetic, or recommendations that are not effective for implants. Thus, one of the key factors to implant success is the adherence to an effective maintenance program to ensure longevity of the implant.10
Dental hygienists play an intricate role in the overall success of dental implants. With the placement of dental implants becoming more common, it is important for hygienists to have a protocol for maintenance. The following is a review of recent studies with information regarding dental implants and proper maintenance.
Implant Failure
Dental implants yield excellent long-term results with 10-year success and survival rates above 95%.7 The reasons for implant failure are still being studied. A thorough medical history is imperative to weigh risk factors of implant failure. Smoking and radiotherapy have been shown to increase implant failure. Studies have shown diabetes and osteoporosis are also risk factors, though more thorough studies are needed to confirm an association.
Other risk factors include biomechanical overload as well as infection and inflammation. Patients with poorly controlled diabetes suffer from impaired osseointegration, elevated risk of peri-implantitis, and a higher level of implant failure. The influence of duration of the disease is not fully clear. When diabetes is well controlled, implant procedures are safe and predictable with a complication rate like that of healthy patients.1 Always get the patients most recent hbA1c reading, current perio chart to help assess inflammation, smoking history, and history of osteoporosis before implant surgery. With this information, the doctor can better discuss the risk factors of implant failure.
Instrumentation
The impact of scalers on implant abutment surfaces varies between abutment types, presumably due to different surface characteristics, with no apparent advantage of one abutment type over the other with regard to resistance to surface damage. Unfilled resin was found consistently to be the least damaging to abutment surfaces, although all scalers of all compositions caused detectable surface changes to polished surfaces of implant abutments.2
A study conducted in 2014 compared cleaning effectiveness of implant prophylaxis instruments. Instrument types included in the study were a plastic curette, carbon-fiber reinforced plastic curette, a sonic driven device with prophylaxis brush without prophylaxis paste, rotating rubber cup with prophylaxis paste, sonic driven device with a plastic instrument tip, ultrasonic device with a plastic instrument tip, and air polishing using low abrasive amino acid (glycine) powder. Nearly all instruments inflicted at least slight damage such as scratches or rounded edges on surface structure. The best cleaning effectiveness was observed with the sonic and ultrasonic oscillating plastic tips and air polishing. Second most effective was the prophylactic brush and prophylactic cup. The least effective was the manual plastic, and carbon-fiber reinforced plastic curettes.3
Another study conducted compared the impact of different scaler material composition on polished titanium implant abutments. The results were glass filled resin scalers caused significantly more and longer scratches while unfilled resin scalers resulted in the least amount of surface change.4
While plastic implant instruments appear to do the least damage to an implant, they are the least effective at debridement. There is also risk of residues of instruments being left on treated surfaces, which might disturb cell attachment.7 “Residues of various curettes and inserts for ultrasonic devices, as well as powder remnants after the use of air-abrasive devices, have all been found on the titanium surfaces after instrumentation.”7
A study was performed to determine the location of inaccessible implant surface areas during debridement. Again, several prophylactic instruments were used, including a Gracey curette, ultrasonic scaler, and air polisher. The study concluded that regardless of the applied cleaning approach and instrument type, significant differences in cleaning efficacy were found between the distinct implant surface areas. Machined surface areas at the implant shoulder were generally well accessible and showed the least amounts of residual stain detectable. Apically facing thread surfaces showed the most residual stain regardless of approach and instrumentation technique. Although air powder abrasives provided the best cleaning results, still around ¾ of the surface remained uncleaned. This study concluded, the development of new instruments must, therefore, focus on the effective debridement of these crucial areas in order to allow for reliable and predictable results in peri-implantitis treatment.5
In summation, “Prevention of peri-implantitis implies keeping smooth surfaces of the implant-supported restoration clean. Ideally, the instruments used to effectively clean smooth surfaces should cause minimal or no surface damage, should not create a surface that is more conducive to bacterial colonization, and should not affect the implant-soft tissue interface. If the soft tissue attachment is disrupted, the instrumentation procedure should maintain a surface that is conducive to the reestablishment of the soft tissue seal.”7 “Regarding smooth surfaces, a roughening of the surface was observed when treated with metal curettes or sonic and ultrasonic devices with metal tips. Although with titanium curettes this occurs to a lesser extent, the use of these instruments on smooth surfaces is not advisable.”7
“The best suitable instrument for any given surface should be chosen depending on the surface properties and localization. From the available instruments, the air polisher seems to currently be the most suitable instrument for both smooth and rough surfaces when preservation of the surface structure is required. In the presence of calcified deposits, the cleaning potential of all mechanical instruments is reduced. Metal instruments are more effective at removing hard deposits; however, it should be kept in mind that these instruments may damage the titanium surface and should be used with caution. If a choice must be made, titanium instruments should be preferred.”7
Suggested Maintenance Protocol
Soft tissue assessment: The soft-tissue assessment includes checking for visual signs of gingival inflammation, such as redness, swelling, alterations of contour and consistency, aberrant gingival form or the presence of fistulas.6
Plaque index: It is recommended that some objective form of plaque monitoring be performed and documented at every maintenance visit, to allow longitudinal assessment of oral hygiene.6
Clinical probing depth: Probing is an important and reliable diagnostic parameter in long-term monitoring of all soft tissues including peri-implant soft tissues. The safety of probing around implant restorations has been well-established, and this procedure does not seem to jeopardize the integrity of oral implants.6 However, less probing force is needed around implants due to the decreased attachment strength to the implant and the connective tissue. It is recommended to wait at least three months after placement before probing implants.10
In the past, plastic probes have been recommended. However, two recent studies suggested conventional metal periodontal probes because they do not appear to cause any damage to either the mucosal attachment or to the implant.6 Though it is acceptable to use either a plastic or metal probe around implants, the use of a plastic probe may have advantages. Plastic probes are more flexible and easier to navigate the contour of the implant.
During the first prophy or periodontal appointment after installation of the prosthesis, it is important to establish the baseline value for clinical probing depths. Again, it is important to make sure the appointment is three months after implant placement. Probing depths for conventionally placed implants, with supraosseous implant platforms, generally range between 2 and 4 mm if the tissues are healthy. Implants placed at bone level or at an intraosseous level may exhibit slightly greater clinical probing depths. Probing depths around implants may be deeper and still be healthy, this is because the sulcus is created surgically and not naturally developed. Increases in both clinical probing depth and bleeding on probing over time are usually associated with loss of attachment and loss of bone and should be viewed as signs of peri-implant disease.6
Bleeding on probing: A study of implants confirmed that absence of bleeding on probing was an accurate indication of stability.6 It has been reported that bleeding on probing alone yields higher diagnostic accuracy at implant sites compared with natural tooth sites.10 These studies highlight the importance of recording bleeding on probing when performing periodontal evaluation to monitor peri-implant soft tissues.
Suppuration: Suppuration should be noted. Suppuration has been associated with peri-implantitis and can be an indicator that anti-infective therapy is warranted.6,10
Stability of the soft tissue margins: Though a correlation between implant failure and stability of soft tissue around implants has not been established, it is important to evaluate and take note of any apical migration of the tissue. Recession can expose rough implant structures, which accumulate more plaque and could lead to inflammation and possible peri-implant mucositis.6
Mobility: Mobility is a primary determining factor for implant health.10 Mobility should be assessed regularly; this can be done manually or by using an automated device. To properly assess mobility for multi-unit implant fixed prosthesis, it is recommended that the prosthesis is periodically removed. By removing the prosthesis, a more accurate assessment can be made regarding mobility, gingival health, and hygiene status. If the prosthesis is not periodically removed mobility could be masked by the stability of the other implants.6
Occlusion: Studies indicate there is a direct correlation between occlusal overload and peri-implant bone loss. Occlusion should be checked at regular intervals to identify and occlusal disharmonies. Premature contacts or other interferences should be identified and corrected.9 A case report published in the International Journal of Oral & Maxillofacial Implants found that “The placement of an unstable removable prosthesis on three well-integrated implants that had been stable for nine years caused noticeable bone loss after six months. The elimination of the traumatic occlusion reversed the situation. The condition has been stable for the past four years”11
Radiographs to monitor bone level: Preservation of crestal bone height is crucial to the long-term success of an implant. Radiographs to monitor crestal bone loss is recommended. To establish baseline bone levels, a radiograph should be taken at implant placement, and again at prosthesis insertion.6 A periapical/vertical bitewing radiograph should be taken at 6-8-month intervals and compared to the baseline to assess crestal bone. If the bone level is stable another periapical/vertical bitewing should be taken after one year and compared. If the bone level continues to be stable periapical/vertical bitewing should be taken every three years. However, any time crestal bone levels change, radiographs should be taken and reviewed every 6-8 months until the bone level is stable for two consecutive periods.10
Homecare
Interproximal cleaning is a must for natural teeth as well as implants. When advising patients on proper homecare, it is important to assess each patients’ individual needs. Due to the contour and shape of implant restorations, plaque removal can be difficult.7 Studies indicate interproximal brushes are superior to traditional floss.
Just one argument against traditional string floss was found in a study conducted in 2016, which tried to determine the relationship between the use of dental floss or superfloss and the development of peri-implantitis. In this study, ten patients with progressive peri-implantitis, who were not responding to professional therapy, including supra and sub-gingival cleanings, were examined. Plaque and bleeding indices, as well as radiographic examinations were performed. In all ten cases, floss remnants were found around the neck and coronal part of the implant. The remnants were removed, and the implant was cleansed, which resulted in significant improvement in 9 out of 10 cases. This study recommends interproximal brushes instead of traditional floss for daily homecare.8
The science seems to be against string floss when it comes to implants. Recommending and showing patients how to properly use interproximal brushes could increase implant success. When recommending interdental brushes, there are a couple of considerations. The first being, the size of the patient’s embrasure spaces; interdental brushes should be correctly sized to fit the interproximal area. Some patients may need multiple sizes of interdental brushes to clean all areas of their dentition, whether it be natural teeth or implants. Another consideration when recommending interdental brushes to implant patients is to recommend brushes that are plastic or metal coated with plastic, as not to scratch the implant. A scratch creates more surface area for bacteria to accumulate and may make proper cleaning harder.
Open contacts between implants and natural teeth should be monitored as well. Five studies indicated that an interproximal gap developed 34% to 66% of the time after an implant restoration was inserted next to a natural tooth. This event occurred as early as three months after prosthetic rehabilitation, usually on the mesial aspect of a restoration. Steps should be taken to check the continuity of the arch periodically. If the clinician detects an open contact, it is prudent to monitor for signs or symptoms of peri-implantitis or peri-implant mucositis. This further enhances the importance of proper homecare instructions and interproximal cleaning instructions.9
Though a lot of implant success is reliant on patient compliance, we as dental professionals are responsible for providing patients with the proper guidance and tools to be successful. It is also our responsibility to take the time to examine and record any changes or concerns we find during implant patients’ regular maintenance appointments. Implants are a great tooth replacement option; it is certainly the one I would choose. The more we know about implant maintenance and care, the better we can serve our patients, which will ultimately make us all better clinicians.
Need CE? Check Out the Self-Study CE Courses from Today’s RDH!
Listen to the Today’s RDH Dental Hygiene Podcast Below:
References
- Naujokat, H., Kunzendorf, B., Wiltfang, J. Dental implants and diabetes mellitus—a systematic review. Int J Implant Dent. 2016 Dec; 2(1): 5. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5005734/
- Hasturk, H., Nguyen, D.H., Sherzai, H., Song, X., Soukos, N., Bidlack, F.B., Van Dyke, T.E. Comparison of the impact of scaler material composition on polished titanium implant abutment surfaces. J Dent Hyg.2013 Aug;87(4):200-11. Retrieved from https://www.ncbi.nlm.nih.gov/pubmed/239864134
- Schmage, P., Kahili, F., Nergiz, I., Scorziello, T.M., Platzer, U., Pfeiffer, P. Cleaning effectiveness of implant prophylaxis instruments. Int J Oral Maxillofac Implants.2014 Mar-Apr;29(2):331-7. Retrieved from https://www.ncbi.nlm.nih.gov/pubmed/24683558
- Hasturk, H., Nguyen, D.H., Sherzai, H., Song, X., Soukos, N., Bidlack, F.B., Van Dyke, T.E. Comparison of the impact of scaler material composition on polished titanium implant abutment surfaces. J Dent Hyg.2013 Aug;87(4):200-11. Retrieved from https://www.ncbi.nlm.nih.gov/pubmed/23986413
- Steiger-Ronay, V., Merlini, A., Wiedemeier, D.B., Schmidlin, P.R., Attin, T., Sahrmann, P. Location of unaccessible implant surface areas during debridement in simulated peri-implantitis therapy. BMC Oral Health. 2017; 17: 137. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5706147/
- Todescan, S., Lavigne, S., Kelekis-Cholakis, A. Guidance for the maintenance care of dental implants: clinical review. J Can Dent Assoc.2012;78:c107. Retrieved from https://www.ncbi.nlm.nih.gov/pubmed/23306040
- Louropoulou, A., Slot, D.E., Barendregt, D.S., van der Weijdent, F.A. Prevention and Treatment of Peri-implant Diseases: Current Evidence on Cleaning of Titanium Dental Implant Surfaces. Int J of Evid Based Pract Dent Hygienist. 2017;3(2): 128-141. Doi: 10.1111607/ebh.137.
- Van Velzen, F.J., Lang, N.P., Schulten, E.A., Ten Bruggenkate, C.M. Dentalfloss as a possible risk for the development of peri-implant disease: an observational study of 10 cases. Clin Oral Implants Res.2016 May;27(5):618-21 Retrieved from https://www.ncbi.nlm.nih.gov/pubmed/26261052
- Greenstein, G., Carpentieri, J., Cavallaro J. Open contacts adjacent to dental implant restorations: Etiology, incidence, consequences, and correction. J Am Dent Assoc.2016 Jan;147(1):28-34. Retrieved from https://www.ncbi.nlm.nih.gov/pubmed/26562738
- Gulati, M., Govila, V., Anand, V., Anand, B. Implant Maintenance: A Clinical Update. Int Sch Res Notices. 2014 Jul 9. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4897104/
- Tawil, G. Peri-implant Bone Loss Caused by Occlusal Overload: Repair of the Peri-implant Defect Following Correction of Traumatic Occlusion. A Case Report. Int J Maxillofac Implants 2008 Jan-Feb;23(1): 153-7. Retrieved from https://www.ncbi.nlm.nih.gov/pubmed/?term=Peri-implant+Bone+Loss+Caused+by+Occlusal+Overload%3A+Repair+of+the+Peri-implant+Defect+Following+Correction+of+the+Traumatic+Occlusion.+A+Case+Report