People who live in developed countries often lack knowledge of some of the serious dental and health issues that persistently trouble residents in developing countries. On an infrequent basis, a horrible disease will surface in a developed country where medical care, nutrition, and sanitation are too often taken for granted.
One of those diseases is noma.
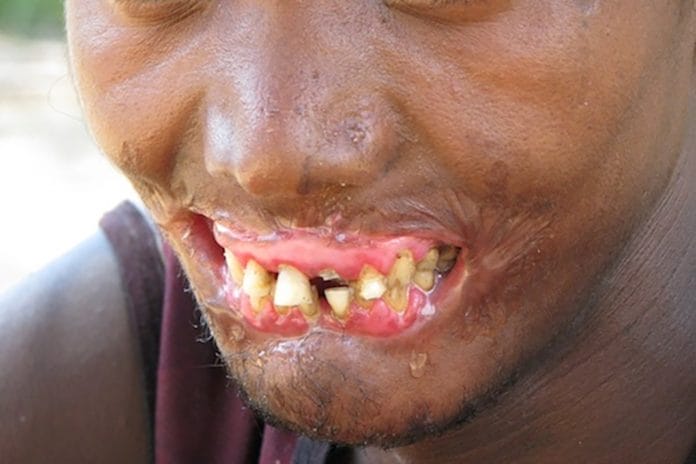
Noma, also known as cancrum oris, is an orofacial gangrene. It is primarily seen in impoverished countries with widespread malnutrition. The etiology of noma is not quite clear. However, it appears to be an opportunistic infection that is seen in patients with a weakened immune system. Diseases associated with noma are measles, malaria, HIV, and poor oral hygiene.
Epidemiological data is lacking; the current estimates of annual cases of noma worldwide is 30,000 to 40,000 cases. The mortality rate is estimated at 85% to 90%. However, with proper medical care, the mortality rate goes down to 8% to 10%. Morbidity is high with complications that include trismus, severe cosmetic disfigurement, difficulty with mastication, fibrous ankylosis of the temporomandibular joint, and reports of high levels of psychiatric issues after recovery.1,2
A case study was published in 2015 on a diagnosis of noma in a 73-year-old African American man. The patient presented to the emergency department in an Atlanta hospital with the following symptoms: “1-day history of fever, altered mental status, and dyspnea.” After assessment, the patient was admitted with a diagnosis of “severe acute respiratory distress syndrome (partial pressure of arterial oxygen/fraction of inspired oxygen = 98), acute kidney injury, and septic shock presumed secondary to aspiration pneumonia.” It was noted that the patient appeared frail and malnourished.
On the fourth day of his hospital stay, “perioral erosions with hemorrhagic crust were noted.” The original treatment of piperacillin/tazobactam was altered, and the patient was started on acyclovir for presumed herpes simplex virus.
By the eighth day, the patient’s white blood cell count had increased from 2,300 per microliter to 19,000 per microliter.3 (For reference, a normal white blood cell count should be between 4,000-11,000 per microliter.) Low white blood cell count is indicative of viral infections and severe bacterial infections, among other things. High white blood cell count is indicative of bacterial infections and tissue damage along with several other health implications.4 Oral surgeons were consulted for this case, and subsequent extractions of the lower right central incisor and upper left cuspid were performed.
By the eleventh day of the patient’s hospital stay, sloughing of dead tissue became disfiguring necrosis. The case study stated, “This necrosis extended superficially from the right philtral crest past the left nasolabial fold and invaded deep through the orbicularis oris to the alveolar mucosa, resulting in exposure of the oral cavity.”
Based on clinical findings and lab results confirming malnutrition, the diagnosis was determined to be noma.3 It is hard to imagine how serious and disfiguring noma can be without a visual. I would recommend viewing the images found in the case study here. Be forewarned, though; the images are very graphic.
Noma is a part of recorded history from as early as the sixteenth century. It wasn’t until the eighteenth century that the connection was made to poverty, malnutrition, and previous illness (primarily measles). By the end of the nineteenth century, noma had almost completely disappeared from the Western world. This decrease was attributed to economic advances, better nutrition, and sanitation. It wasn’t until the twentieth century that effective drugs to treat noma were discovered.5
According to the World Health Organization (WHO), cases of noma are “reported for young children aged 3-5 years in Africa, Latin America, and Asia; with 90% of them dying without having received any care.”6 Noma has been classified as a human rights violation by some. In a review published in International Health, the authors state, “Noma is a biological indicator of multiple human rights violations, including the right to food. International support and national attention in countries with noma are lacking.”7
Though noma is not common in developed countries, I believe it is important to understand that it is still a contributing factor in the deaths of many young children. I hope highlighting this case will bring more attention to the struggles many face in developing countries.
References
- Srour, M.L., Marck, K., Baratti-Mayer, D. Noma: Overview of a Neglected Disease and Human Rights Violation. Am J Trop Med Hyg. 2017 Feb 8; 96(2): 268-274. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5303022/
- Ashok, N., Tarakji, B., Darwish, S., Rodrigues, J.C., Altamimi, M.A. A Review on Noma: A Recent Update. Glob J Health Sci. 2016 Apr; 8(4): 53-59. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5303022/
- Maleyy, A., Desai, M., Parker, S. Noma: A disease of Poverty Presenting at an Urban Hospital int the United States. JAAD Case Rep. 2015 Jan; 1(1): 18-20. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4802558/
- WBC count. U.S. National Library of Medicine. Retrieved from https://medlineplus.gov/ency/article/003643.htm
- Marck, K.W. A History of Noma, the “Face of Poverty.” Plast Reconstr Surg. 2003 Apr 15; 111(5): 1702-7. Retrieved from https://www.ncbi.nlm.nih.gov/pubmed/12655218
- What is the burden of oral disease? World Health Organization. Retrieved from https://www.who.int/oral_health/disease_burden/global/en/
- Srour, L.M., Marck, K.W., Barratti-Mayer, D. Noma: Neglected, Forgotten and a Human Rights Issue. Int Health. 2015 May; 7(3): 149-50. Retrieved from https://www.ncbi.nlm.nih.gov/pubmed/25609756