Approximately 1.7 million cancer cases are expected to be diagnosed in 2019, and over 600,000 are expected to die from cancer this year.1 In fact, 1 in 3 will personally deal with cancer in their lifetime.1 With these kinds of statistics, it is realistic to say each of us will either personally experience cancer or will have a family member/close friend who will deal with cancer.
Most certainly, dental professionals will all see patients who have dealt with or are presently dealing with cancer. One of my best friends had a rare form of cancer. While going through chemotherapy, she texted me one night and asked me if I had any suggestions for the sores in her mouth, which she had developed from the chemotherapy. I felt inadequately prepared to answer her questions, and this led me to do more research on the subject.
Cancer is defined as the “uncontrolled growth and spread of abnormal cells.”1 These cells kill by metastasizing (spreading), invading, and destroying surrounding tissues.2 Fortunately, the survival rate has increased significantly since 1991 due to preventive measures and more advanced treatment.1 Most cancers are treated through one or a combination of the following methods: chemotherapy, radiation therapy, surgery, or immunotherapy such as bone marrow transplant.2,3,4
Unfortunately, these treatments do not come without oral side effects, and we need to be prepared to help our patients through this difficult time.
Cancer Treatments Can Impact Oral Health
Chemotherapy – This treatment works by killing cancer cells, but it also can damage healthy cells and thus cause side effects.4 Chemotherapy targets the whole body, as opposed to radiation therapy, which usually limits the effects to a specific organ or area.3 One side effect of chemotherapy is the decreased formation of white and red blood cells as well as platelets5, which leaves patients susceptible to infection and increased bleeding.
For these reasons, it is best to wait on elective dental treatment (including routine prophys) and consult with the oncologist before emergency treatment.5, 6 This suppressed immune system can cause an increase in periodontal disease or dental abscesses.2
Radiation therapy – This treatment targets a specific part of the body and uses high energy rays to destroy cancer cells. Because cancer cells rapidly divide, radiation therapy damages cell DNA preventing cancer cells from future division and growth.3 Radiation therapy can be provided either externally or internally. This method is frequently used for head and neck cancer.
The side effects are limited to the localized area treated. For this article, the side effects mentioned are specific to head and neck radiation treatment.
Immunotherapy − The last treatment method mentioned is immunotherapy, which includes bone marrow transplant or stem cell transplant. Sometimes, the body doesn’t recognize cancer cells as a problem because they are the individual’s mutated cells. Immunotherapy tries to jump-start the immune system to recognize and fight off cancer cells. Either the patient’s own or a donor’s bone marrow or stem cell is injected into the body. The goal is to either boost the patient’s immune system or help the patient’s body recognize cancer cells and destroy them.3 Some transplant patients experience graft versus host disease (GVHD), which can some side effects.6
Some side effects of this treatment are mucositis, xerostomia, and hemorrhaging.2
Common Side Effects of Cancer Treatment
Mucositis − One of the most common side effects of cancer treatment is mucositis (inflammation and ulceration of the mucous membranes).2,6-10 Mucositis often starts five to 10 days after initial treatment and can be painful enough to interfere with eating and nutrition, and sometimes requires delaying further treatment. Patients often describe burning or discomfort, which is exacerbated if it is accompanied by nausea and vomiting.
Unfortunately, mucositis doesn’t usually resolve itself until the white blood count raises, which can take one to six weeks. The best way to prevent mucositis is to have good oral hygiene. Patients should be encouraged to brush and floss daily. If a normal tooth brushing becomes too painful, an extra soft toothbrush can be used, or even a damp washcloth can remove plaque.
Patients should not use toothpastes that have whitening agents or are irritating, or alcohol mouth rinses. Patients with mucositis can rinse after meals with a mixture of .25 tsp salt, 1.5 tsp baking soda and a cup of warm water. Coating agents such as “magic mouthwash” (viscous lidocaine, Maalox, and diphenhydramine) can provide pain relief as well as sucking on ice pops or ice chips.6,9
Taste changes − Some chemotherapy medications and/or destruction of the taste buds through radiation therapy may cause an altered taste. Taste changes will likely return to normal a few weeks after treatment but may last up to two months.11 If salivary glands are damaged, the altered taste may be permanent.
Patients may complain of foods tasting differently, foods tasting bland, all foods tasting the same, or food that tastes metallic or chemical.11 Unfortunately, there is not a lot to be done for taste changes, but sucking on sugar-free mints may mask the taste.
Additionally, using plastic utensils may help reduce the metallic taste, as well as flavoring food with spices, herbs, and sauces. Sometimes cold or frozen foods may taste better than heated foods.9
Xerostomia − Xerostomia can be a common side effect of cancer treatment, especially those who have been treated with radiation therapy in the head and neck region. As hygienists, we can recommend salivary substitutes and provide education about the hazards of sucking on sugar candies to stimulate saliva flow.
Patients should be encouraged to drink lots of water and suck on ice chips. Rinsing with the baking soda rinse mentioned above will help break down the thick saliva which can accompany xerostomia. Patients should be educated about the risk of radiation caries and encouraged to brush and clean interdentally regularly. A humidifier can help with xerostomia at night2. Additionally, chewing xylitol gum can stimulate saliva as well as reduce decay.4
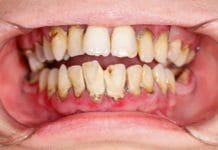
Radiation caries − Radiation caries is related to xerostomia and a lowering of the pH in the mouth. This type of caries often begins in the cervical region of the tooth.12-15 If preventive measures are not taken, severe tooth damage can happen within the three months following radiation therapy.
Patients undergoing head and neck radiation therapy should be fitted with custom trays and apply fluoride gel for 10 minutes each day. Additionally, patients should be encouraged to restrict cariogenic foods, and provided with home care instructions including both brushing and interdental cleaning.12-15 Steps to control xerostomia mentioned above should be followed.
Osteonecrosis − Osteonecrosis can be a side effect of radiation therapy. Signs of osteonecrosis are severe pain, exposed bone in the treatment area that doesn’t heal, and repeated infections. As the name implies, osteonecrosis is the death of the bone and is due to decreased vascularity after radiation therapy.
Similar to patients using bisphosphates, avoiding tooth extractions after radiation therapy is encouraged when possible. Managing osteonecrosis involves treatment with antibiotics, chlorhexidine rinse, and good oral hygiene.12 More advanced cases may need surgery or laser therapy.16
Dental hygienists frequently see patients who are presently going through cancer treatment, are still dealing with residual effects of cancer treatment, or have family members going through cancer treatments. By understanding cancer treatments, identifying potential oral side effects, and providing guidance we can help our patients get through this difficult time.
Author’s note: This article is dedicated to one of my best friends, Jorja Peterson who died from cancer. (1974-2016).
References
- American Cancer Society. (2019) Cancer facts & figures 2019. Retrieved from https://www.cancer.org/content/dam/cancer-org/research/cancer-facts-and-statistics/annual-cancer-facts-and-figures/2019/cancer-facts-and-figures-2019.pdf
- Davis, J. M. (2015). Cancer. In M. L. Darby, & M. M. Walsh (Eds), Dental hygiene in theory and practice (pp. 841-59). St. Louis, MO: El Sevier.
- American Cancer Society. (2019). Treatment and side effects. Retrieved from https://www.cancer.org/treatment/treatments-and-side-effects/treatment-types.html
- Harding, J. (2017). Dental care of cancer patients before, during and after treatment. British Dental Journal, (4). 10-12. https://doi.org/10.1038/bdjteam.2017.8
- UK Medicines Information. (2016). How should adults with cancer be managed by general dental practitioners if they need dental treatment? National Health Services. Retrieved from https://www.sps.nhs.uk/wp-content/uploads/2016/06/NW-QA-70.1-Cancer-in-dental-patients-.pdf
- National Institutes of Health. 2009. Dental Provider’s oncology pocket guide. Retrieved from https://www.nidcr.nih.gov/sites/default/files/2017-09/oncology-guide-dental-provider_0.pdf
- Oral Cancer Foundation. (2019). Mucositis. Retrieved from https://oralcancerfoundation.org/complications/mucositis/
- Beech, N., Robinson, S., Porceddu, S., Batstone, M. (2014). Dental management of patients irradiated for head and neck cancer. Austrailian Dental Journal, 59. 20-28. doi:1111/adj.12134.
- American Society of Clinical Oncology. (2018). Mouth sores or mucositis. Retrieved from https://www.cancer.net/coping-with-cancer/physical-emotional-and-social-effects-cancer/managing-physical-side-effects/mouth-sores-or-mucositis.
- Raber‐Durlacher, J.E., Elad, S., Barasch, A. (2010). Oral mucositis. Oral Oncology, 46(6). 452–456. doi: 10.1016/j.oraloncology.2010.03.012.
- American Society of Clinical Oncology. (2018). Taste changes. Retrieved from: https://www.cancer.net/coping-with-cancer/physical-emotional-and-social-effects-cancer/managing-physical-side-effects/taste-changes
- Gupta, N. et al. (2015). Radiation-induced dental caries, prevention and treatment: A systematic review. National Journal of Maxillofacial Surgery6(2) 160-6. doi:10.4103/0975-5950.183870.
- Walker, M.P., Wichman, B., Cheng A.L., Coster, J., Williams, K.B. (2011). Impact of radiotherapy dose on dentition breakdown in head and neck cancer patients. Practical Radiation Oncology 1. 142–148. https://doi.org/10.1016/j.prro.2011.03.003.
- Vissink, A., Jansma, J., Spijkervet, F.K., Burlage, F.R., Coppes, R.P. (2003). Oral sequelae of head and neck radiotherapy. Critical Reviews in Oral Biology and Medicine14(3). 199–212.
- Jham, B.C., Reis, P.M., Miranda, E.L., Lopes, R.C., Carvalho, A.L., Scheper, M.A., Freire, A.R. (2008). Oral health status of 207 head and neck cancer patients before, during and after radiotherapy. Clinical Oral Investigations 12(1). 19-24. https://doi.org/10.1007/s00784-007-0149-5.
- Rodriguez-Lozano, F.J., Oñate-Sánchez, R.E. (2016). Treatment of osteonecrosis of the jaw related to bisphosphonates and other antiresorptive agents. Medicina Oral Patoogia Oral y Cirugia Bucal 21(5) e595–e600. doi:10.4317/medoral.20980.