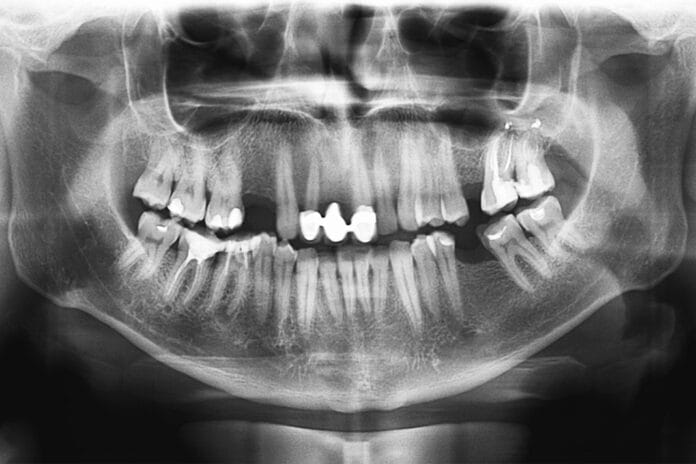
Patients who experience bruxism, or teeth grinding and clenching, often suffer from jaw pain, tooth sensitivity, headaches, and other symptoms. A diagnosis usually starts with a patient’s self-report data, but bruxism may go unnoticed for those who grind their teeth unconsciously. A recent study from Switzerland shows promising results in using panoramic radiographs to diagnose bruxism by looking for changes in the mandible.
What is Bruxism?
Stress, genetics, or other factors may cause bruxism. One type occurs during the day, called awake bruxism. The other happens at night, or sleep bruxism, resulting in various symptoms like worn enamel (wear facets), attrition, cracked teeth, temporomandibular joint (TMJ) clicking, and pain in the temporal, masseter, and medial pterygoid muscles. Sometimes, of interest to this study, bruxism may even cause bone changes along the jawline.
Bruxism is usually diagnosed during a dental examination, together with feedback from the patient. A differential diagnosis may be needed to distinguish bruxism from other disorders that affect bones and teeth, like movement disorders or bone tumors. Special instruments, like an electromyograph that records muscle movement, are helpful but are often hard to come by, unlike readily available panoramic radiograph equipment. Panoramic radiographs, which capture the entire mouth in one image, provide an easy view of potential jawline irregularities and are especially helpful for bruxism patients.
The Study
In this retrospective study, researchers compared panoramic radiographs of 100 bruxism patients, from the University of Basel’s Department of Oral Health and Medicine to a control group of 100 adolescents, from the Department of Pediatric Oral Health and Orthodontics. They chose adolescents for the control group since bruxism-related jawbone changes, they assumed, had not occurred yet due to their young age.
The Cranex D cephalometric radiograph system captured these radiographs between May 2010 and May 2017. Researchers selected radiographs that included the entire jawline and excluded images with blurs or markings, making them non-diagnostic. In order to focus on bruxism, they also excluded patients with other diagnoses, like bone disorders.
Paying special attention to the mandibular angle region and basal cortical bone, researchers looked for bone and jaw-shape changes that may result from extensive biting and clenching forces. They aimed to evaluate and grade these changes, which are common in bruxism patients, on a scale between 0 and 3.
- Grade 0 – No Changes.
- Grade 1 – Angular changes, with no bone changes.
- Grade 2 – Angular changes, plus some bone changes.
- Grade 3 – Angular changes, plus bone changes at several locations.
Researchers graded a total of 200 patients, or 400 mandibular angles, according to the above criteria. Findings were evaluated with MedCalc statistical software.
Results
According to this study, more than half of bruxism patients (59 patients) showed signs of either Grade 2 or Grade 3 bone remodeling. In contrast, the control group showed no signs of bone changes, and some (64 patients) had signs of angular changes under the Grade 1 category.
Bone remodeling may result from repetitive bite force and motion, causing the jawbone to transform and adapt over time, which may be seen on panoramic radiographs. For adolescents, even though approximately half of children have bruxism, they probably don’t experience jawline changes at a young age. However, more studies are needed.
In this study, researchers used an odds ratio calculation to find that bruxism patients were 288 times more likely to experience bone changes when compared to patients without bruxism. Similarly, using the same calculation, bruxism patients were 363 times more likely to experience angular changes along the jawline when compared to non-bruxers.
Patients may be unaware of changes occurring in their mandible, and since they usually obtain radiographs as part of a routine visit, panoramic radiographs show promise in diagnosing or confirming bruxism. An early diagnosis may help us to manage our patient’s condition more closely before they incur irreversible tooth damage or other long-term symptoms.