Stomatitis, also known as oral mucositis, is an inflammation in the mouth that affects the mucous membranes, and the condition arises from either a local stimulation or a systemic provocation.1 The causes of stomatitis are bacterial, fungal, viral, systemic, medications, physical irritants, allergies, irradiation, and chemotherapy, leading to reactions varying from stinging, soreness, red patches, mouth ulcers, blisters, peeling, swelling, oral numbness, and burning mouth.
Stomatitis plays a role in the oral cavity through many factors and can be caused by injury, infection, allergy, systemic or skin disease. The most relevant suspects are xerostomia, therapeutic radiation, trauma, the toxicity of chemotherapy medications, tobacco smoking, and viral infections, affecting the buccal mucosa, gingiva, tongue, throat, lips, roof, or floor of the mouth.
Stomatitis is grouped into categories depending on where it forms in the mouth.
- Cheilitis is inflammation of the lips around the mouth, specifically the corners of the mouth.
- Gingivitis is inflammation of the gingiva.
- Glossitis is inflammation of the tongue.
- Pharyngitis is inflammation at the back of the throat.
A review of various conditions is below, and dental interactions are also discussed.
Stomatitis Venenata
Stomatitis venenata is also known as allergic contact stomatitis and mucosal allergy. It’s a delayed hypersensitivity where the body reacts to a substance when it’s in contact with an allergen at a localized area. An allergy in the oral cavity arises from a variety of factors, including mouthwash, toothpaste, lip balms, dental materials, foods, gloves, and flavoring agents (commonly cinnamon or mint).
The clinical appearance is circumscribed erythema patches, vesicles, fissures, ulceration, sloughing, and crusting with burning and swelling pain. An acute case presents as redness and edema.2 In comparison, a chronic case presents as white and hyperkeratotic.2 Determining the cause can sometimes be frustrating as the reactions are delayed and nonspecific.
Stomatitis venenata occurs locally in an already sensitive person. The process of a reaction starts at a localized area by a low molecular weight chemical and infiltrates into the mucosa to bind with epithelial proteins. With the encouragement of Langerhans cells in converting haptens, a prominent antigen is produced. On initial contact of the antigen, immune cells are released for healing and then divided to form memory cells. When the antigen is exposed again, the body triggers the memory cells for a quicker and more aggressive response with chemical mediators to combat inflammation and damage.
Treatment and management are avoiding the culprit if known, and topical steroids to reduce the inflammatory response.2.3
Stomatitis Areata Migrans
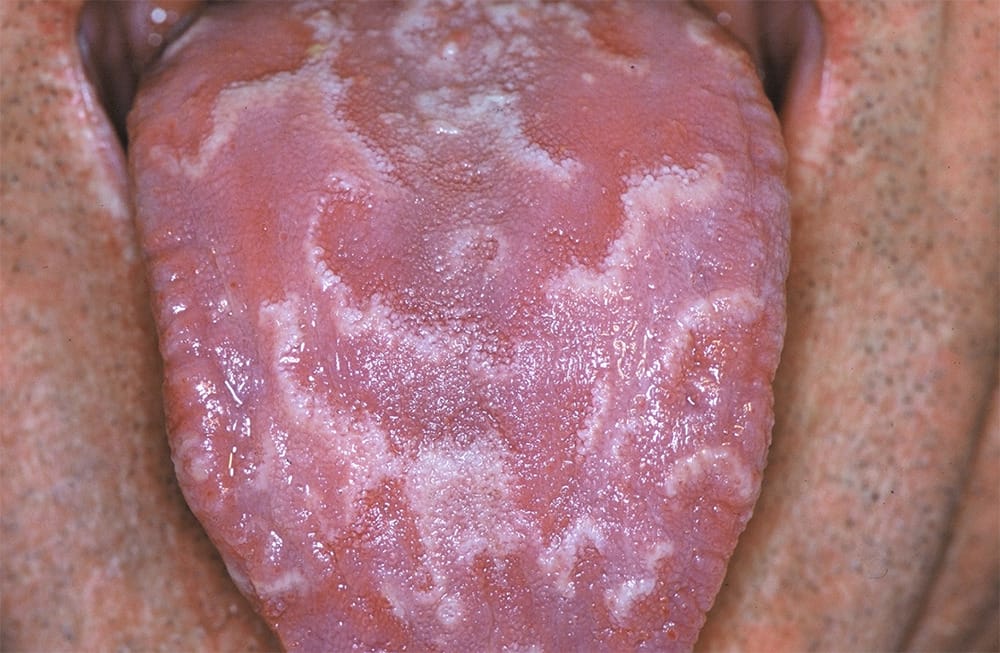
Photo courtesy Dimitrios Malamos, CC BY 4.0 <https://creativecommons.org/licenses/by/4.0>, via Wikimedia Commons
Also known as geographic tongue (see Image 1), the source of stomatitis areata migrans isn’t clear. Some suggestions are hypersensitivity, hormonal or nutritional imbalance, and stress. The appearance is circumscribed, erythematous patches that may be encircled with white or gray margins. The tongue’s fungiform papillae become noticeable due to the loss of filiform papillae. Somatitis areata migrans occurs mainly on the dorsal and ventral parts of the tongue, and its occurrence may be higher in women, diabetic, and psoriasis patients.4
Lesions that move around on the tongue and may have a burning sensation are erythema migrans; the nonlingual form of geographic tongue is migratory stomatitis.
Treatment and management are antihistamine mouthwashes for pain and an oral antibiotic for secondary bacterial infection.4
Angular Stomatitis
© Irena / Adobe Stock
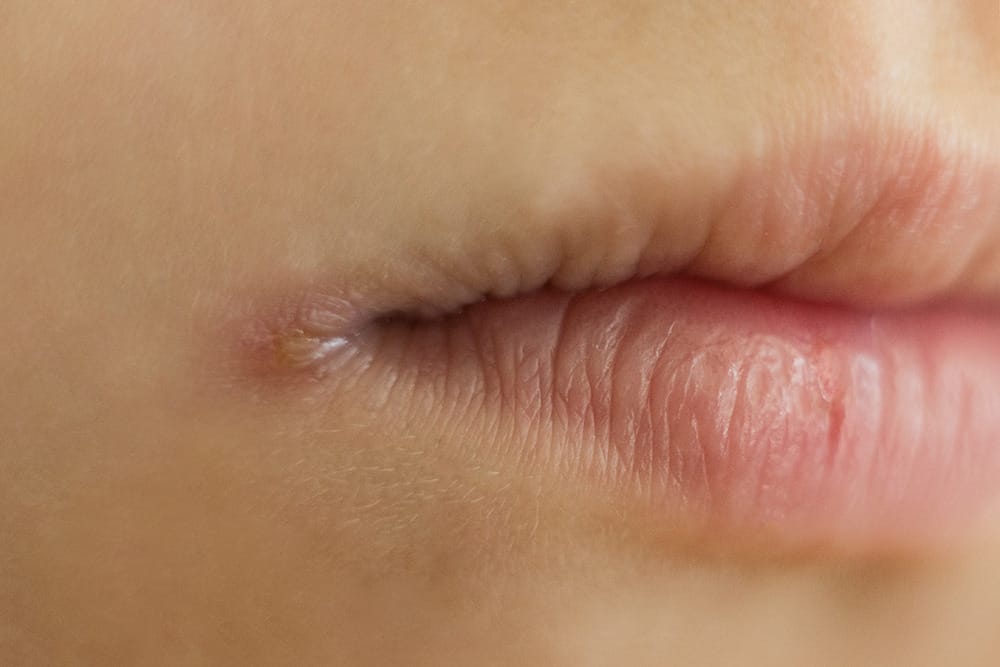
Angular stomatitis is commonly known as angular cheilitis (see Image 2). It is the cracking, crusting, blistering, or oozing of the corners of the mouth caused by a yeast infection such as candida, a bacterial infection such as staphylococcus aureus, or a viral infection such as herpes simplex cold sores. This could cause soreness, redness, or bleeding from constant wetting with saliva, deep furrows, ill-fitting dentures, uncontrolled diabetes, steroid inhalers, or poor nutrition.5
Treatment or management is to maintain blood sugars, a healthy diet, or nutritional supplements, topical anti-fungal ointments or antiseptics, and antibiotics. If it is a bacterial or fungal infection, the infection could eventually spread to the adjacent skin and even lead to oral thrush.6
Aphthous Stomatitis
© Charnsitr / Adobe Stock
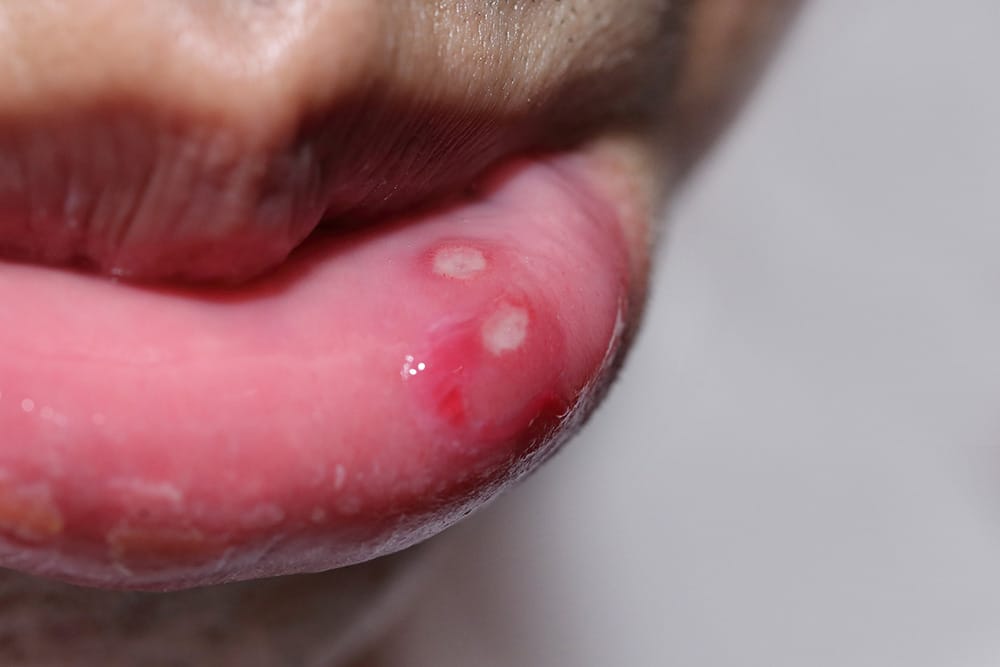
More commonly known as canker sores (see Image 3), aphthous stomatitis occurs in two variants, major and minor. They are benign, noncontagious, well-demarcated, shallow, ovoid, or round-shaped. The center of the aphthous is necrotic with a red halo and slightly raised erythema borders around a yellow-gray pseudo membrane.
Minor aphthous stomatitis is less than eight millimeters (generally 2 to 3 mm). They emerge on the floor of the mouth, buccal mucosa, pharynx, and the lateral and ventral parts of the tongue. They tend to heal in 10 days and leave no scarring, and make up about 85 % of cases.
Major aphthous stomatitis is larger than one centimeter. They appear on the lips, soft palate, and throat. These sores last longer, usually weeks or months, and may be accompanied by fever, dysphagia, malaise, and scarring. This type accounts for about 10 % of cases.
The less common ulcers, herpetiform aphthous, make up the other 5% of cases. They initiate in multiple clusters of 1 to 3 mm and increase in size that may last up to two weeks. These ulcers are painful and form on an erythematous foundation.
Factors include oral trauma, stress, and certain foods. Oral trauma from dental work, sharp tooth surfaces, dentures, and orthodontics may cause breakouts. Certain foods such as citrus fruits, coffee, eggs, chocolate, and nuts along with deficiencies with vitamin B, iron, and zinc, can promote triggers. Medical conditions contributing to aphthous stomatitis are celiac disease, inflammatory bowel disease, autoimmune diseases, and a weakened immune system, and a clinical diagnosis is based on appearance.7
Treatments using topical chlorhexidine and corticosteroids are more efficient at the beginning stages of development of burning pain and tingling. Supplements of vitamin B or iron and avoiding any known food reactions may help lessen breakouts.7
Chronic Ulcerative Stomatitis
Chronic ulcerative stomatitis (CUS) primarily occurs in the mucous membranes and is painful and exacerbating with recurring ulcerations. It is not fully understood but may be related to autoimmune diseases.8 According to a Tufts University of Dental Medicine research of chronic ulcerative stomatitis, when high concentrations of antibodies were apparent, there was a complete detachment of the epithelium. A lack of damage to the surface epithelial cells and a change in the cell-binding proteins allows the surface layer to attach to the connective tissue beneath. The promotion of a weakened attachment and tissue breakdown causes ulcerative sores in the mouth.9
Treatment and management use hydroxychloroquine in keeping this condition at bay.8,9
Denture-related Stomatitis
Also referred to as thrush, denture-related stomatitis is caused by candida. It is not contagious nor caused by an allergy to the material in a denture. Stomatitis mainly occurs with the maxillary denture and rarely with the mandibular denture.
The appearance may be bright red with swelling under the denture. The patient may experience halitosis, altered taste, xerostomia, burning sensations, or bleeding, and sometimes it may correlate with angular cheilitis.
Treatment and prevention are removing the denture daily for the tissue to breathe and keeping it really clean. If left untreated, it could become very sore and cause ill-fitting dentures.10
According to the European Association of Oral Medicine Newtons, the classifications of denture stomatitis are:
- Type 1: Pin-point hyperemic lesions, localized simple inflammation.
- Type 2: Diffuse erythema confined to the mucosa contacting the denture, generalized simple inflammation.
- Type 3: Granular surface.11
Necrotizing Ulcerative Gingivostomatitis
Better known as ANUG or trench mouth, necrotizing ulcerative gingivostomatitis is also called Vincent’s stomatitis. This condition is the rapid destruction of periodontal tissues and is considered a relentless condition of gingivitis leading to necrosis of gum tissue. It can advance into nearby tissues of the tonsils, pharynx, cheeks, lips, and jawbone.
This condition is not contagious.12 The causative anaerobic bacteria are mainly Fusobacterium, P. intermedia, Borrelia vincentii, and spirochetes. Factors include poor hygiene, weakened immune system, stress, poor nutrition, smoking, and methamphetamine and ecstasy use.
The symptoms for the patient will happen in progression. Beginning manifestations that may occur are regular gingivitis of painful red, inflamed gingiva with mild bleeding and a bad taste in the mouth. Progressive and more serious symptoms include bleeding gingiva to gentle stimulation, severe discomfort with eating or swallowing, interproximal crater-like ulcers, tissue destruction around the teeth, swollen head and neck lymph nodes, and mild fever and fatigue. The notable characteristic is the grayish film on the gingiva from the decaying of the gingival tissue.
A severe variant of necrotizing ulcerative gingivostomatitis is called noma, which is a rapidly progressive gangrenous stomatitis, an accelerated infection of the mouth and face. As ANUG is a precursor to noma, this progressive stage can cause full-thickness tissue destruction of the mucous membranes of the mouth, which degrades tissues of the bones in the face. It commonly affects a debilitated or malnourished patient.
Treatment and management of ANUG include irrigation and debridement, mouth rinses, pain medication, and antibiotics. Good home care will prevent it from occurring. It is treatable, but it can have major complications with the spread of infection and tooth loss if left untreated.13
Nicotine Stomatitis
Nicotine stomatitis is also called smokers palate, and it occurs from exposure to heat from tobacco, cigar, and cigarettes ─ but more so in pipe smoking. Its appearance is a diffused, white, thickening of the palatal mucosa with interspersed, elevated white, papules each with a red central depression. The red dot-like appearance is inflamed openings of minor salivary glands. If dentures are worn, nicotine stomatitis will be beyond the denture plate in the back of the mouth.
Treatment and management are smoking cessation, and the tissue will usually reverse in one to two weeks. Any suspicious areas should be biopsied even though nicotine stomatitis is not considered premalignant except with reverse smoking (the lit end is placed in the mouth). Smoking itself, however, is a higher risk for oral cancer.13
Plasma-cell Gingivostomatitis
Also called atypical gingivitis, plasma-cell gingivostomatitis is atypical as it is a rare, benign inflammatory condition where an abundance of plasma cells infiltrate within the connective tissue. The clinical appearance will present with a sharply demarcated, edematous, erythematous, and diffused gingivitis spreading into the mucogingival junction. It appears more often on the maxillary than the mandibular arch and is not contagious.
This immunological reaction is commonly from allergens with flavors such as mint or cinnamon. Known causes are toothpaste, chewing gum, lozenges, and some herbs and strong spices such as chili, pepper, and cardamom. Poor home care may worsen the condition.
Treatment or management is avoiding the allergens. The process of elimination or changing oral health products may lead to success along with good home care for plaque control.14
Pyostomatitis Vegetans
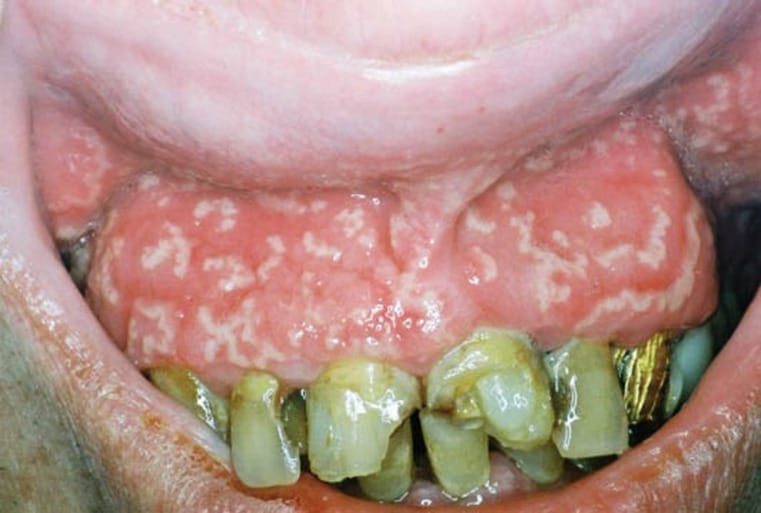
This is an exceedingly rare inflammatory cutaneous condition involving the oral cavity and other skin areas on the body. Pyostomatitis vegetans affect the mucosal layers of the oral cavity, and this condition can have a quick, aggressive eruption of multiple yellowish pustules on the erythematic and swelling tissue. This necrosis may happen under vulnerable conditions, forming a snail track appearance (see Image 4).
Other clinical appearances of the tissue are inflammation, thickening, redness, cobblestoned, elevated growths, and lymph node enlargement under the chin, and there may be mild to severe pain involvement. As it rarely affects the tongue and floor of the mouth, it does primarily affect the gingiva, palate, and throat. The buccal mucosa and lips may become folded.
This condition is considered idiopathic with no major underlying cause, and pyostomatitis vegetans could be considered a marker for inflammatory bowel disorders (Crohn’s and ulcerative colitis). The above symptoms tend to show up after a few years of ulcerative colitis, and it may be the cause of a rare condition of orofacial granulomatosis.15
Treatment or management is resolving the underlying cause for inflammatory bowel disease if that’s the reason. Topical options are antiseptic mouthwashes, topical steroids, or tacrolimus. Systemic options are oral corticosteroids, azathioprine (immunosuppressive), dapsone, cyclosporine (IBS), sulfasalazine (IBS), mesalazine (IBS), sulfamethoxypyridazine (antibacterial), oral or intramuscular methotrexate, and infliximab infusions.16
Herpetic Gingivostomatitis
© Ocskay Bence / Adobe Stock
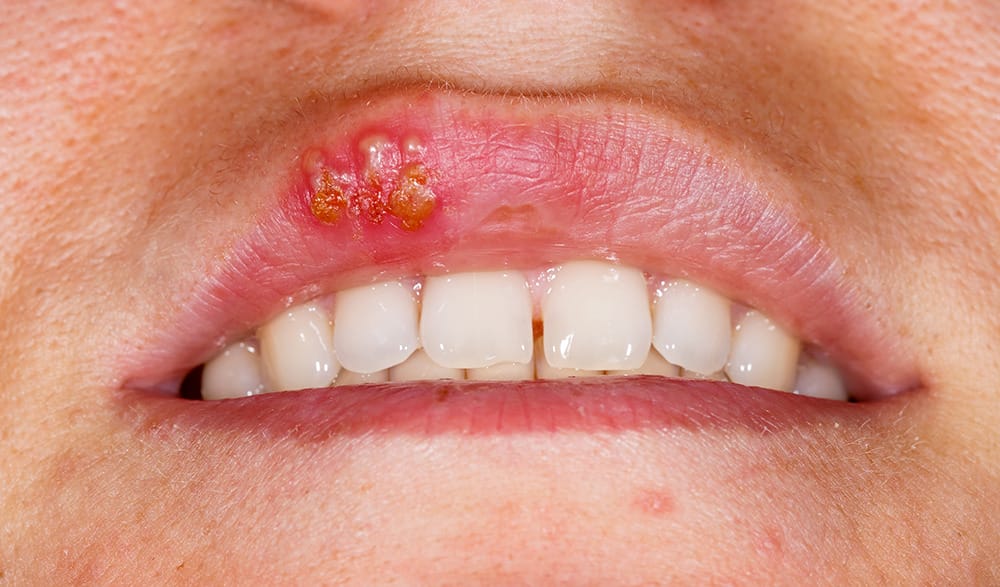
This is an acute infection associated with herpes simplex virus type 1. Herpetic gingivostomatitis presents with a high-grade fever along with painful oral lesions. It is contagious and transferred by infected droplets or direct contact from an asymptomatic or nonsymptomatic patient. The infection lasts a lifetime, and intermittent breakouts can recur.
The appearance of these lesions is flat, yellowish, and about 2 to 5 mm vesicles, which quickly rupture to form small superficial ulcers. The healing time is about two to three weeks, and the condition is non-scarring. The gingival tissue may be enlarged and erythematous, affecting both keratinized and nonkeratinized mucosa. It tends to be more common in children under the age of five than adults.
Treatment and management are hydration and analgesics for pain, as well as petroleum jelly to prevent adhesions with active herpetic gingivostomatitis.17
Stomatitis treatment depends on the cause. If it’s allergy-related, then eliminating the allergy-causing agent will help. If it’s infection-related, medication or specialized treatment is needed. If it’s disease-related, diagnosing and treating the disease will treat the source and not the symptoms. If it’s a nutritional deficiency, adjusting the diet will be needed to improve vitamin deficiencies.
A thorough health history with lifestyle questions will be beneficial in distinguishing the conditions of stomatitis, as many of them have a differential diagnosis. While many patients will wait to report breakouts until their next cleaning appointment, encouraging a patient to go to the dentist during the breakout (except during a herpetic outbreak) provides a true perspective for the dental professional, ensuring a more efficient treatment.
Need CE? Check Out the Self-Study CE Courses from Today’s RDH!
Listen to the Today’s RDH Dental Hygiene Podcast Below:
Stomatitis References
- Seymour, T. (2017, June 09). Everything You Need to Know About Stomatitis. Medical News Today. Retrieved from https://www.medicalnewstoday.com/articles/317839
- Desai, V. Pratik, P. Stomatitis Venenata a Rarity. Universal Research Journal of Dentistry. 2016; 6: 39 -40. Retrieved from https://www.researchgate.net/publication/344152121_UnivResJDent_2016_Stomatitis_Venenata_A_Rarity
- Prakash, K. Biswas, P.G., Prabhakar, M., Shanmugapriya, P.S. A Case Report on Stomatitis Venenata due to the Use of Lip Balm. Medical Archives. 2020; 74(1): 65. 10.5455/medarh.2020.74.65-68. Retrieved from https://www.researchgate.net/publication/339878717_A_Case_Report_on_Stomatitis_Venenata_Due_to_the_Use_of_Lip_Balm
- Lawson, W. Erythematous Oral Lesions: When to Treat, When to Leave Alone. Consultant360. 2012; 52(6): 449-456. Retrieved from https://www.consultant360.com/article/erythematous-oral-lesions-when-treat-when-leave-alone
- Angular Cheilitis. (2018, October). Sheffield Teaching Hospitals Retrieved from https://publicdocuments.sth.nhs.uk/pil2642.pdf
- Gotter, A. (2020, March 19). What You Need to Know about Angular Cheilitis. Healthline. Retrieved from https://www.healthline.com/health/angular-cheilitis#diagnosis
- Hennessy, B.J. (2020, May). Recurrent Aphthous Stomatitis. Merck Manual. Retrieved from https://www.merckmanuals.com/professional/dental-disorders/symptoms-of-dental-and-oral-disorders/recurrent-aphthous-stomatitis
- Ferrisse, T.M., Travassos, D.C., Rocha, A.F., Massucato, E.M., Bufalino, A. Chronic Ulcerative Stomatitis: A Systematic Review of the Clinical and Microscopic Features. Medicina oral, patologia oral y cirugia buccal. 2019; 24(6): e698–e703. Retrieved from https://doi.org/10.4317/medoral.22213
- Chronic Ulcerative Stomatitis is an Autoimmune Disorder, Research Shows. The Journal of the American Dental Association. 2011; 142(7): 797-798. ISSN 0002-8177. Retrieved from https://jada.ada.org/article/S0002-8177(14)62258-3/fulltext
- Denture Stomatitis. (n.d.). Oral Health Foundation. Retrieved from https://www.dentalhealth.org/denture-stomatitis
- Denture Related Stomatitis. (n.d.). European Association of Oral Medicine. Retrieved from https://eaom.eu/education/eaom-handbook/denture-related-stomatitis/?v=7516fd43adaa
- Acute Necrotizing Ulcerative Gingivitis (ANUG). (n.d.). Dental Disease. Retrieved from https://www.dentaldiseases.org/conditions/gums/acute-necrotizing-ulcerative-gingivitis.htm
- Dyall-Smith, D. (2010) Nicotine Stomatitis. DermNet NZ. Retrieved from https://www.dermnetnz.org/topics/nicotine-stomatitis
- S., Gujjari, S.K., Hegde, U., Kumar, V. (2011). Unusual Clinical Presentation of a Case of Localized Plasma Cell Gingivitis. Journal of Clinical and Diagnostic Research. 2011; 5(5), 1125-1127. Retrieved from https://www.jcdr.net/articles/pdf/1543/56%20-%203208.pdf
- Pyostomatitis Vegetans Definition, Oral Lesions, Diagnosis, Treatment. (2013.) Health and Care Information. Retrieved from https://healthncare.info/pyostomatitis/
- Dyall-Smith, D. (2010). Pyodermatitis-pyostomatitis Vegetans. Retrieved from https://www.dermnetnz.org/topics/pyodermatitis-pyostomatitis-vegetans/
- Aslanova, M., Ali, R., Zito, P.M. Herpetic Gingivostomatitis. [Updated 2020 Sep 29]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan. Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK526068/.