In the United States, the Commission on Dental Accreditation (CODA) sets accreditation standards for dental education programs, including dental hygiene. Despite these standards, not all dental hygiene programs are exactly the same because not all dental hygiene program directors or instructors are exactly alike. The knowledge a dental hygiene professional (DHP) has regarding patient care protocols, treatment modalities, current research, and the like also vary due to many factors, such as the continuing education courses each individual takes or how well a DHP actively engages in lifelong learning.
While no two DHPs are alike in the United States, the same can be said for DHPs in other countries. Have you ever wondered about treatment protocols in different countries or how DHPs differ in their treatment protocols in different countries? Researchers from Goethe-University, Frankfurt, Germany, and Tel Aviv University, Israel, set out to do just that in a study published in the International Journal of Dental Hygiene.1
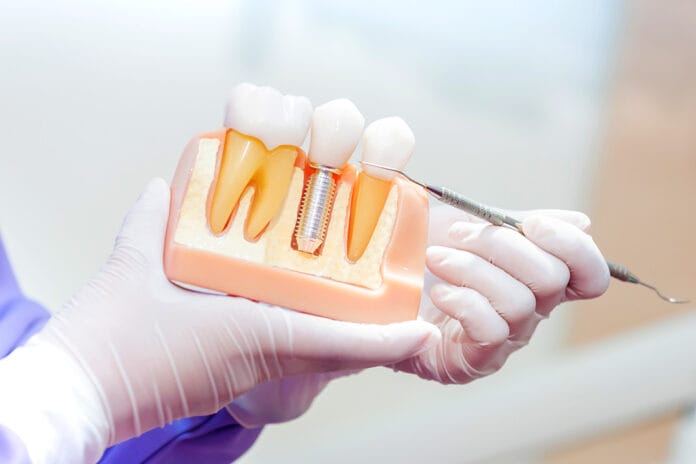
Their research aimed to assess the common practices of DHPs in Germany compared to Israel regarding training on implants in educational programs and implant maintenance to determine differences in practice.
Background on Dental Hygiene Practice in the European Union
Before getting into the research results, a bit of background on dental hygiene practice in the EU might be advantageous. The researchers state, “The work of DHPs is structured differently within the European Union (EU) and in countries of EFP [European Federation of Periodontology] member societies. In 18 EU member states, dental hygienists’ occupational licensing is regulated, while in eight member states (Austria, Bulgaria, Estonia, France, Germany, Luxemburg, Romania, and Cyprus), it is not. Beyond regulations, there may also be differences in education/training regarding peri-implant diseases.”1
As of September 2020, the Israel Central Bureau of Statistics reported the Israeli population was 9.4 million, and in 2020 the number of DHPs was 2663. “In Israel, dental hygienists’ education consists of two full years, or 2000 academic hours, undertaken in one of the four educational institutions recognized by the Ministry of Health. To practice as a DHP, obligatory licensure examinations must be performed.”1 DHPs in Israel must practice under the supervision of a dentist.1
In 2020, Germany’s population was approximately 82 million. “In September 2019, 1820 dental hygienists received education in Germany, of whom 1646 (90%) completed education as a dental assistant and later received a dental hygienist professional certificate after further education. In total, 174 DHPs (10%) had completed a bachelor’s degree in dental hygiene.”1 In Germany, only dentists are allowed to practice dentistry, though they can delegate certain defined treatments to DHPs. DHPs must practice under the direct supervision of a dentist.1
Methods
The researchers used an online questionnaire created by the Periodontology Departments of Goethe-University, Frankfurt, Germany, and Tel Aviv University, Israel. Distributed via social media by DHP associations, the questionnaire collected information on the demographics, training, prevention, and treatment of peri-implant diseases in both countries. The total responses to the questionnaire that were included in the research analysis were 376 DHPs, 169 from Israel, and 207 from Germany. It’s worth mentioning that most participants were female and had received education and worked in their home countries.1
Summary of Results (not all results from the questionnaire are listed)
| Implant Maintenance and Treatment Education
During their primary education: |
German DHPs | Israeli DHPs |
| Received training in treatment of peri-implant infection | 82% | 59% |
| Treated peri-implant infection | 72% | 41% |
| Used mechanical (i.e., instrumentation) and/or chemical (i.e., chlorhexidine irrigation) implant treatment therapies | 62% | 46% |
| Did not perform any treatment of implants | 15% | 38% |
| Implant Assessments in Practice | German DHPs | Israeli DHPs |
| Reported the symptoms of peri-implant infection are redness, edema, exudation/bleeding, mobility, and recession | 71% | 67% |
| Plaque, bleeding, and probing depths are assessed | 74% | 67% |
| Do not assess plaque, bleeding, or probe depths | 1% | 5% |
| Routinely monitor implant health with radiographs | 56% | 17% |
| Only take radiographs if problems are assumed | 43% | 43% |
| Do not take radiographs of implants | 1% | 40% |
| Do not probe implants at all* | 5% | 22% |
| Use metal probes on implants | 33% | 49% |
| Use plastic probes on implants | 44% | 22% |
*Researchers state, “Occasional peri-implant probing at low force (0.25 N) does not harm peri-implant tissues, similar to periodontal probing, which does not harm periodontal tissues. However, the benefits and therapeutic consequences of peri-implant probing as well as BOP are still debated.”1
| Oral Hygiene Instruction given to Patients with Implants | German DHPs | Israeli DHPs |
| Education given about risk factors that contribute to peri-implantitis | 98% | 94% |
| Provide oral hygiene instruction at each maintenance appointment independent of oral health status | 73% | 66% |
| Give no oral hygiene instruction at all | 4% | 0.6% |
| Treatment of Implants | German DHPs | Israeli DHPs |
| Do not perform hand instrumentation | 8% | 1% |
| Perform subgingival instrumentation | 56% | 86% |
| Use steel instruments | 23% | 80% |
| Use titanium instruments | 30% | 14% |
| Use plastic instruments | 23% | 28% |
| Do not use devices other than hand instruments
(i.e., prophy jet) |
2% | 77% |
| Do not use ultrasonics | 23% | 19% |
| Use prophy jet with or without nozzle | 96% | 18% |
| Use laser | 14% | 1% |
In Closing
Despite advancements in dental care, many people suffer tooth loss. This is mainly caused by dental caries, injury, or periodontal disease. For many years, bridges, partials, and dentures were the only way to replace missing teeth. But today, dental implants are available, and placement is increasing.
According to a 2018 study, the prevalence of dental implants increased from 0.7% in 1999 to 5.7% in 2016 in the United States.2 According to the researchers of this summarized study, “3.4% of individuals aged 35–44 years, 8.1% aged 65–74 years, and 8% aged 75–100 years presented with dental implants” in Germany.1
“With increasing numbers of dental implants inserted and the mean prevalence of peri-implant mucositis and peri-implantitis of 43% and 22%, respectively, these diseases represent growing oral health problems. The prevention and treatment of peri-implant mucositis consequently prevent peri-implantitis.”1
The researchers conclude further information regarding DHPs training on implants in educational programs and implant maintenance to determine differences in practice should take place in other countries.1 Perhaps a similar study in the United States should take place and focus on the differences between each state. Knowing where dental hygienists are in their implant knowledge and how they maintain the oral health of patients with implants could guide what education they may need. This data could not only help guide CODA accreditation standards of dental hygiene programs but also guide state dental boards on required continuing education courses.
Lastly, I will conclude with this: What I found especially profound that the researchers stated in this study was, “Considering the high prevalence of severe periodontal diseases, the prevention, treatment, and maintenance of periodontal diseases can only be provided at the population level if dentists are supported by dental hygiene professionals.”1 Dental hygienists are necessary, indeed.
Before you leave, check out the Today’s RDH self-study CE courses. All courses are peer-reviewed and non-sponsored to focus solely on high-quality education. Click here now.
Listen to the Today’s RDH Dental Hygiene Podcast Below:
References
- Eickholz, P., Winkler, P., Elez, I., et al. Common Practices of Dental Implants Maintenance among Dental Hygiene Professionals in Isreal and Germany. International Journal of Dental Hygiene. Aug 2022: Epub ahead of print. https://onlinelibrary.wiley.com/doi/10.1111/idh.12612
- Elani, H.W., Starr, J.R., Da Silva, J.D., Gallucci, G.O. Trents in Dental Implant Use in the U.S., 1999-2016, and Projections to 2026. Journal of Dental Research. 2018; 97(13): 1424-1430. https://pubmed.ncbi.nlm.nih.gov/30075090/