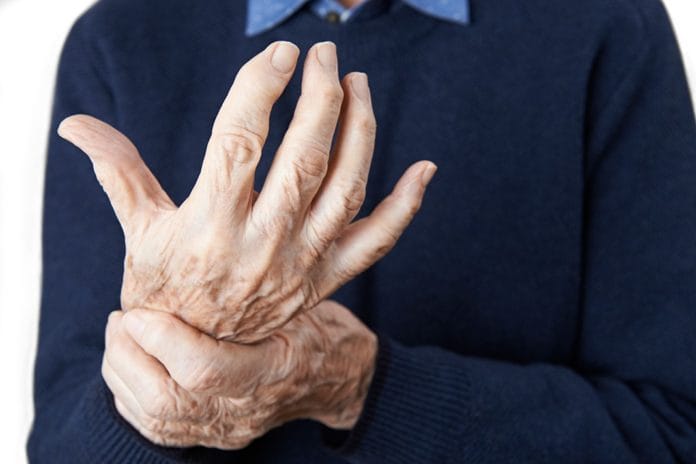
What is Rheumatoid Arthritis?
Commonly referred to as RA, this disease is an autoimmune disorder. The immune system mistakenly attacks the joints, thinking a bacterial or viral infection is present. When the body attacks joints, it results in inflammation of the joints and usually is bilateral, meaning if one hand hurts the other one will too. The most common joints affected are hands, feet, wrists, knees, and elbows.3 Joints usually become very painful, and if left untreated, can cause deformities. This disease can come and go with minimal flare-ups if treated early. RA is manageable with medication and taking care of oneself properly. Professional dental cleanings and having a healthy mouth can be the difference between manageable pain versus severe pain, according to research.3
How Does Rheumatoid Arthritis Affect the Oral Cavity?
RA causes joints to become inflamed because the body attacks the joints thinking there is a bacterium or a virus which needs to be fought off. Current research on this topic has no conclusive evidence of which comes first; whether RA causes periodontal disease or periodontal disease triggers RA. “Research in the area of periodontal disease and rheumatoid arthritis in the last two years has confirmed long-standing observed associations between the two disease processes. New observations have demonstrated that periodontal disease is present, and severe, early in the rheumatoid arthritis disease process providing further evidence toward a causal or permissive event.1”
This is what we do know about the two diseases: RA and periodontal disease both cause inflammation. Studies show people who have RA are eight times more likely to have periodontal disease and to be missing teeth.3 Research also shows patients who receive professional dental cleanings, and who are taking RA medication, had more significant pain relief and RA became more manageable than those who were on medication alone.3
One tricky thing with RA is patients who suffer from this autoimmune disease often end up having dexterity issues, which often leads to patients unable to effectively practice proper oral hygiene. While it is recommended RA patients keep regular dental care appointments and take special care with preventive measures, many patients don’t keep regular dental appointments. This could possibly be because they don’t feel like they are doing an adequate job with home care and may be embarrassed. Like any patient suffering from RA or not, this results in patients being diagnosed with periodontal disease later than they would have if they were keeping regular appointments.
Most research states periodontal disease is likely to occur in those with RA; how progressive the periodontal disease becomes and how bad the RA is for that particular patient is a challenging timeline to nail down because everyone develops symptoms differently.3 This also limits the education which can be provided to patients; for instance, tools which can be used to help with dexterity issues, proper oral health care, and disease management.
“RA can lead to tooth loss and other health complications like heart disease.1” Patients who suffer from RA are also more likely to develop Sjorgens Syndrome or Sicca Syndrome, which attack the glands in the mouth leading to xerostomia.3 Xerostomia increases issues with root caries and periodontal disease. RA patients need to be evaluated by a dentist twice a year to monitor progress and alert patients if periodontal disease is present. Regular maintenance can help lessen the severity of periodontal disease and reduce the incidence and severity of RA.
Rheumatoid Arthritis Medication Oral Effects
Patients with RA are often prescribed immunosuppressant medication(s) to help manage the progression of the disease. However, immunosuppressant medications can have oral side effects and oral implications. Oral ulcerations have been found to occur in patients taking these types of medications and can be quite painful.“Oral mucosal symptoms caused by drugs can be further divided as follows: (1) lichenoid reaction/lichen planus; (2) ulcers; (3) erythema multiforme; (4) pigmentation; (5) autoimmune vesiculobullous disease; (6) infections; (7) tumors (fibrovascular hyperplasia); (8) swellings (angioedema); and (9) keratosis.5”
Immunosuppressants can also lead to other diseases and opportunistic infections. “Some drugs they use now are aimed at blocking an inflammatory marker made by the white blood cells called tumor necrosis factor (TNF). The TNF alpha blockers are often used now with great effect.4” Diseases, such as cancer, and opportunistic infections, such as Candida albicans (thrush), may affect the oral cavity. I’ve often treated patients on TNF blockers who develop Candida infections. Candida is an “opportunistic infection that’s actually linked with rheumatoid.4”
Home Care Tips
Patients who suffer from RA may develop dexterity issues due to deformity and joint pain. As clinicians, there are many options we can recommend to help patients maintain their oral hygiene at home. For instance, building up the base of a toothbrush with a tennis ball or putty, using an electric toothbrush, recommending interdental aides such as flossers with a handle or interdental brushes might be good options. Other items which can be helpful are toothpaste with a pump, or a mechanism attached to make the toothpaste come out easier without having to squeeze the tube. It will take some time to figure out which item works best for each patient, and is important patients give themselves time to get used to a new home care product.
Xerostomia is another complication patients with RA may suffer. Figuring out the best product to help with this issue is vital. Dry mouth can put a patient at higher risk for caries, especially root caries Again, finding a product which works for each patient as an individual is key. A prescription fluoride toothpaste might be beneficial to RA patients as well.
With any product, I always recommend patients use it every day as directed for seven days before they decide it is or isn’t the product for them. I explain to patients the effects don’t always happen immediately, which is important to point out, because many patients expect immediate results, then ultimately don’t use the product long enough for the benefits to take place.
Maintenance
Patients who have autoimmune diseases, periodontal disease, and other oral health complications like xerostomia, a three-month recall is recommended to help reduce the colonization of bacteria and help maintain the disease the disease process. A tightened recall also gives the clinician the opportunity to educate more often and find out earlier if something isn’t working for the patient. It’s important to listen to patients’ concerns and work to address them in their treatment plan. We all want to be heard and feel our concerns are important, so don’t forget our patients feel that way too. Listening to and addressing each concern can be an immense help in regards to patient compliance and treatment outcomes.
Living with RA and periodontal disease can be manageable by seeing medical and dental professionals regularly to help prevent unmanageable pain from occurring and maintaining the disease. Patients still don’t understand the systemic links between oral health and overall health and why medical histories are so important; many “just want their teeth cleaned.” Bridging that gap has proven to be difficult; however, continuing to educate patients is imperative to close the mouth-body link gap.
SEE ALSO: Periodontal Disease Link to Rheumatoid Arthritis
Now Listen to the Today’s RDH Dental Hygiene Podcast Below:
Resources
- Bingham, C.O., Moni, M. Periodontal Disease and Rheumatoid Arthritis: The Evidence Accumulates for Complex Pathobiologic Interactions. Current Neurology and Neuroscience Reports. U.S. National Library of Medicine, May 2013. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4495574/
- Garrard, Cathy. Rheumatoid Arthritis and Gum Disease: What You Need to Know. Stroke Center – EverydayHealth.com, 18 Oct 2016. Retrieved from https://www.everydayhealth.com/rheumatoid-arthritis/living-with/the-link-between-gum-disease-and-rheumatoid-arthritis/
- Rheumatoid Arthritis. Arthritis Foundation. Retrieved from https://www.arthritis.org/about-arthritis/types/rheumatoid-arthritis/
- Bakker, E. Rheumatoid Arthritis and the Candida Connection. Retrieved from https://www.candidacrusher.com/rheumatoid-arthritis-and-candida-connection/
- 5.Jinbu, Y., Demitsu, T. (May 2014). Oral Ulcerations Due To Drug Medications. Japanese Dental Science Review. 50(2): 40-46. Retrieved from https://www.sciencedirect.com/science/article/pii/S1882761613000811