A recent study showed there might be a possible link between periodontal disease and rheumatoid arthritis. The findings, which were presented at the 2018 Annual European Congress of Rheumatology, revealed periodontal diseases might be a key initiator for the chronic disease. The event was organized by the European League Against Rheumatism (EULAR), a non-profit dedicated to sharing the latest news and scientific developments about rheumatoid diseases. The group also promotes and supports the research, treatment, and rehabilitation of the disease.
About Rheumatoid Arthritis
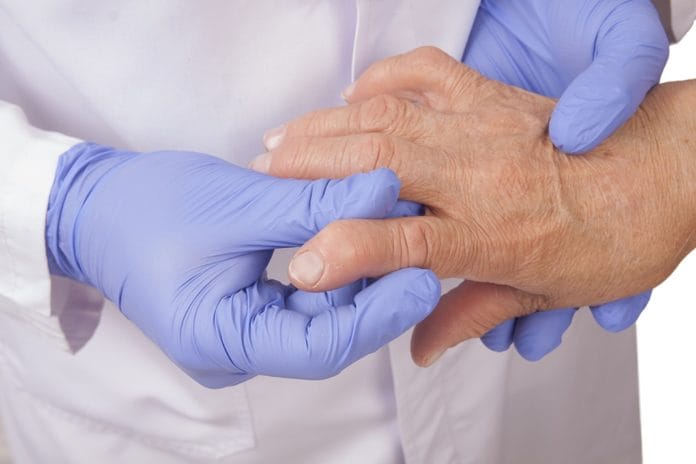
Rheumatoid arthritis is an autoimmune disease which causes inflamed joints. It’s also considered a systemic disease because it can affect other systems in the body like the respiratory system. Patients who are diagnosed with rheumatoid arthritis may feel pain in their back and muscles. It can be very painful for them to move because their joints are stiff and swollen. Other symptoms include nausea, fatigue, dry mouth, and anemia. Patients may develop deformed joints and experience bone erosion over time if it is left untreated.
According to the Arthritis Foundation, an estimated 1.5 million people in the United States have rheumatoid arthritis. Women and patients over the age of 45 are more likely to be diagnosed with the disease.
The Link between Rheumatoid Arthritis and Periodontal Disease
An association between periodontal disease and rheumatoid arthritis was first discovered in 1926. Since then, scientists have uncovered evidence to suggest that poor dental health is also linked to other serious health conditions, including cardiovascular diseases, diabetes, obesity, and pulmonary diseases, among many others.
The research presented at the 2018 Annual European Congress of Rheumatology provided more data to support the claim that there is a correlation between rheumatoid arthritis and periodontal disease. The study was presented by Kulveer Mankia, MD, a professor at the Leeds Institute of Rheumatic and Musculoskeletal Medicine and the Leeds Biomedical Research Centre in England. Mankia organized the study and led the team of researchers.
Mankia decided to examine three different groups of people for the study. The first group included 26 people who were diagnosed with rheumatoid arthritis. The second group included 32 people who were healthy and 48 people who were considered at-risk comprised the third group. The latter group tested positive for anti-citrullinated protein antibodies and musculoskeletal symptoms but showed no signs of clinical synovitis.
The researchers studied six sites per tooth in each participant over the duration of the study. They isolated DNA from subgingival plaque and looked for three different types of bacteria that contribute to periodontal disease: Filifactor alocis, Porphyromonas gingivalis, and Aggregatibacter actinomycetemcomitans.
The Results of the Study
At the end of the study, Mankia concluded patients who were at risk for rheumatoid arthritis displayed higher levels of periodontal bacteria. Based on their findings, he believes the inflammation caused by periodontal disease may be a key initiator of the systemic autoimmunity seen in rheumatoid arthritis.
The researchers found patients who were diagnosed with periodontal disease, with higher levels of Porphyromonas gingivalis and Aggregatibacter actinomycetemcomitans, were 73% more likely to develop rheumatoid arthritis when compared to 38% of the control group. Of the 48 people who were considered at-risk, Porphyromonas gingivalis was most closely linked to severe periodontal disease.
In Conclusion
The researchers hope more scientists will continue to examine the association between rheumatoid arthritis and periodontal disease. Once health professionals have a better understanding of what causes rheumatoid arthritis, they will be able to develop more advanced prevention and treatment options.
SEE ALSO: Ask Kara RDH: What is the Best Way to Suggest Perio Treatment to a Patient?
DON’T MISS: Bridging the Gap Between Medicine and Dentistry